Table of Contents
Definition / general | Essential features | Anatomy & physiology | Diagrams / tables | Clinical features | Gross description | Gross images | Microscopic (histologic) description | Microscopic (histologic) images | Virtual slides | Positive stains | Negative stains | Electron microscopy description | Electron microscopy images | Videos | Board review style question #1 | Board review style answer #1 | Board review style question #2 | Board review style answer #2Cite this page: Stringham N. Histology-fibrous tissue & nerve. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/softtissuefibrousnormal.html. Accessed April 2nd, 2025.
Definition / general
- Fibrous connective tissue is composed of fibroblasts and extracellular matrix (ECM; i.e., collagen, elastin, ground substance)
- Nerves are composed of many nerve fibers (axons, myelin) bound together with connective tissue sheaths (epineurium, perineurium, endoneurium)
Essential features
- Fibroblasts are the primary functional cell in connective tissue and are involved in maintaining homeostasis within the ECM, producing collagen and healing wounds
- Dense (fibrous) connective tissue creates the framework for tissues and organs; it also forms tendons and ligaments throughout the musculoskeletal system
- Nerves comprise bundles of nerve fibers, connective tissue and a blood supply; peripheral nerves appear grossly as solid, white to yellowish bands of tissue
- Primary function of neurons is to send information throughout the body via electrochemical signals; nerve fibers are formed from the neural axons and their myelin sheath
- Connective tissue component of the peripheral nervous system (PNS) comprises the epineurium, perineurium and endoneurium (Schapira: Neurology and Clinical Neuroscience, 2007)
Anatomy & physiology
Connective tissue
Fibroblasts
Nerve
- Loose (cellular) and reticular connective tissue
- Higher number of cells compared to collagen fibers
- Cell types: fibroblasts, mast cells, lymphocytes, plasma cells (activated B cells), granulocytes, adipose
- Lamina propria is a loose connective tissue under a moist epithelium
- Dense (fibrous) connective tissue
- Mostly collagen but shows some fibroblasts (nuclei are visible)
- Dense, irregular connective tissue: not well ordered, gaps between fibers, nuclei are outside collagen fibers
- Found in many areas; e.g., submucosa of GI tract, lymph nodes, tunica albuginea of testis, periosteum, reticular layer of dermis
- Fascia is a specialized connective tissue that connects and encapsulates tissues and organs throughout the body; it can have a role in pain regulation, organ inflammation, trauma and fibrotic diseases (Am J Physiol Cell Physiol 2024;327:C357)
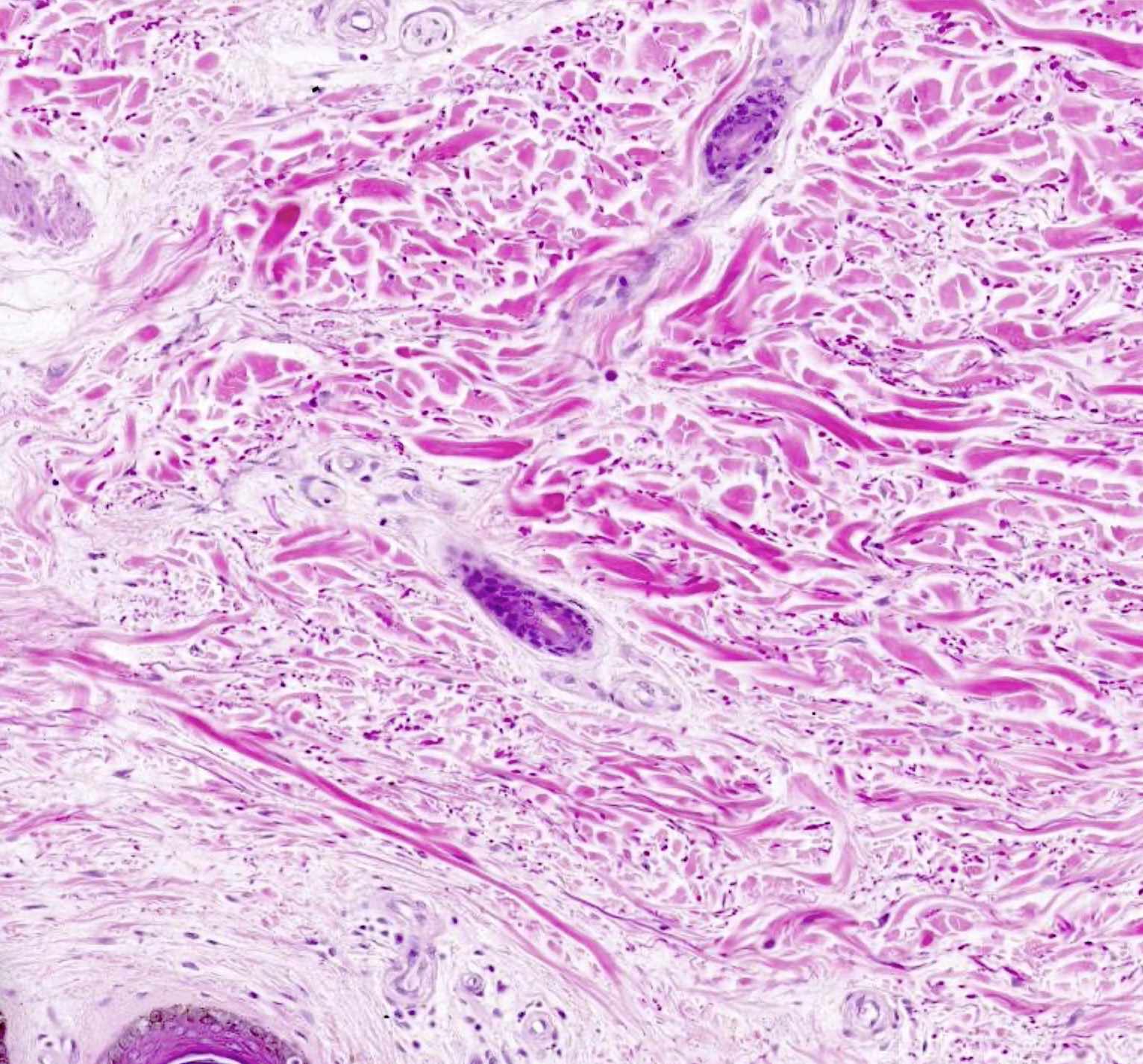
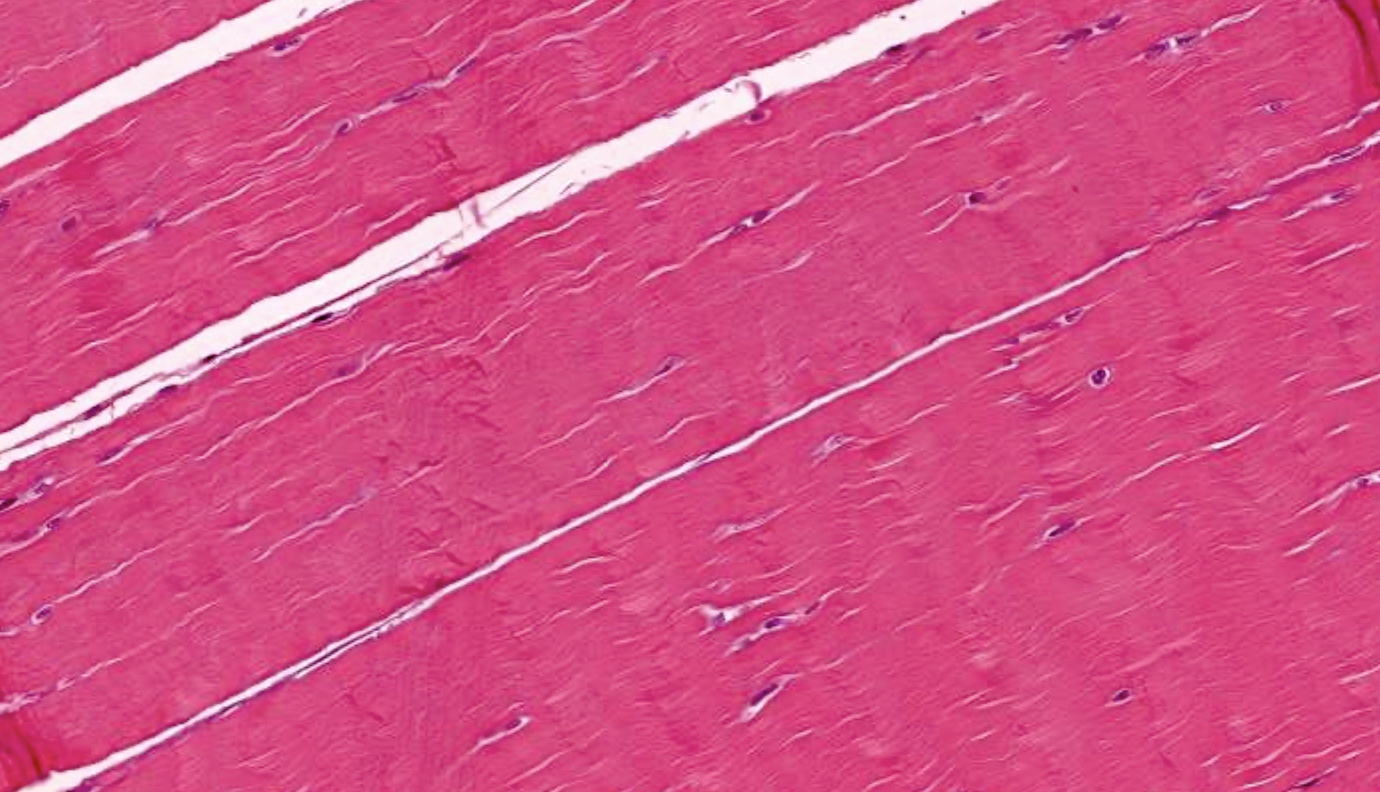
- Dense, regular connective tissue: collagen fibers are densely packed and running in one direction; nuclei are outside collagen fibers
- Found in tendons (connect muscle to bone), ligaments (connect bones or cartilage to each other), aponeuroses (ribbon-like tendinous expansion)
- References: StatPearls: Physiology, Connective Tissue [Accessed 10 October 2024], Adv Drug Deliv Rev 2003;55:1531
Fibroblasts
- Most common cell type in stroma and connective tissue
- Comprises the framework for tissues and organs (e.g., skin, lung, heart, kidney, liver, eye)
- Function
- Maintaining extracellular matrix (ECM) homeostatic environment
- Involved in all stages of wound healing (inflammation, cell proliferation, ECM deposition, remodeling)
- Shape: spindled shape along collagen fibers to stellate in myxoid areas
- Origin: mesenchyme, which originates from mesoderm
- Products
- Collagens (type I, III, IV)
- Proteoglycans, fibronectin, laminins, glycosaminoglycans, metalloproteinases, prostaglandins
- Can underlie organ pathogenesis via dysregulated collagen deposition
- Respond to both autocrine and paracrine signals (Int Rev Cytol 2007;257:143)
- Proinflammatory cytokines and growth factors can activate matrix reorganization via degradation and fibroblast mediated enzyme crosslinking
- Fibrocyte is a fibroblast in a quiescent state
- In adults, fibroblasts remain quiescent until stimulated
- Cellular plasticity
- Terminally differentiated cells (i.e., adipocytes, pericytes, epithelial and endothelial cells) can dedifferentiate into fibroblasts
- Fibroblast stimulation increases the likelihood of epigenetic changes
- Myofibroblast is a modified fibroblast that transitions from fibroblasts during tissue repair (J Invest Dermatol 2007;127:526, Int Rev Cytol 2007;257:143)
- Features are intermediate between fibroblasts and smooth muscle cells
- Work to form granulation tissue during wound healing
- Reference: StatPearls: Histology, Fibroblast [Accessed 10 October 2024]
Nerve
- Peripheral nerves contain bundles of nerve fibers (i.e., an axon and its myelin sheath), connective tissue and a blood supply
- Most peripheral nerve fibers are myelinated by Schwann cells, which are glia that wrap around the axon and increase its conduction velocity
- Nodes of Ranvier are ion channel rich gaps between Schwann cells where the axon potential can be regenerated; these can be appreciated at a microscopic level and are areas that are vulnerable to immune mediated neuropathies (J Peripher Nerv Syst 2023;28:S12)
- Peripheral nerves contain both motor (efferent) and sensory (afferent) nerve fibers
- Peripheral sensory nerves transmit information about the external environment to the central nervous system; they are derived embryologically from neural crest (StatPearls: Neuroanatomy, Sensory Nerves [Accessed 10 October 2024])
- Sensory nerve transmission velocity is determined by its diameter and whether or not it is myelinated; large diameter myelinated fibers are the fastest
- Proprioceptors: largest diameter fibers (A alpha, A beta)
- Mechanoreceptors: medium diameter fibers (A beta, A delta)
- Nociceptors and thermoreceptors: smallest diameter fibers (A delta, C fibers)
- C fibers are unmyelinated and therefore have the slowest velocity
- Neurons are the functional cells of nerves (StatPearls: Physiology, Nerve [Accessed 10 October 2024])
- Composed of a cell body (soma), axon (sends information away from cell body via action potential) and dendrites (receives information into cell body)
- Cell bodies of neurons reside in the central nervous system in cortex and nuclei and in the peripheral nervous system in ganglia
- Unipolar cell bodies of most sensory neurons reside in the dorsal root ganglia of the spinal cord
- Cell bodies contain organelles with prominent rough endoplasmic reticulum, called Nissl substance, due to the large amount of membrane that must be produced
- Primary function is to send information throughout the body via electrochemical signals
- Connective tissue component of nerves (Barral: Manual Therapy for the Cranial Nerves, 2013)
- Epineurium: forms the sheath that surrounds all peripheral nerve trunks (i.e., whole nerve)
- Continuous with dura mater
- Internal epineurium separates fascicles while external epineurium forms a sheath around the fascicles
- Contains fibrous connective tissue, adipose, microvasculature (i.e., vasa nervorum), perivascular plexus (i.e., nervi nervorum)
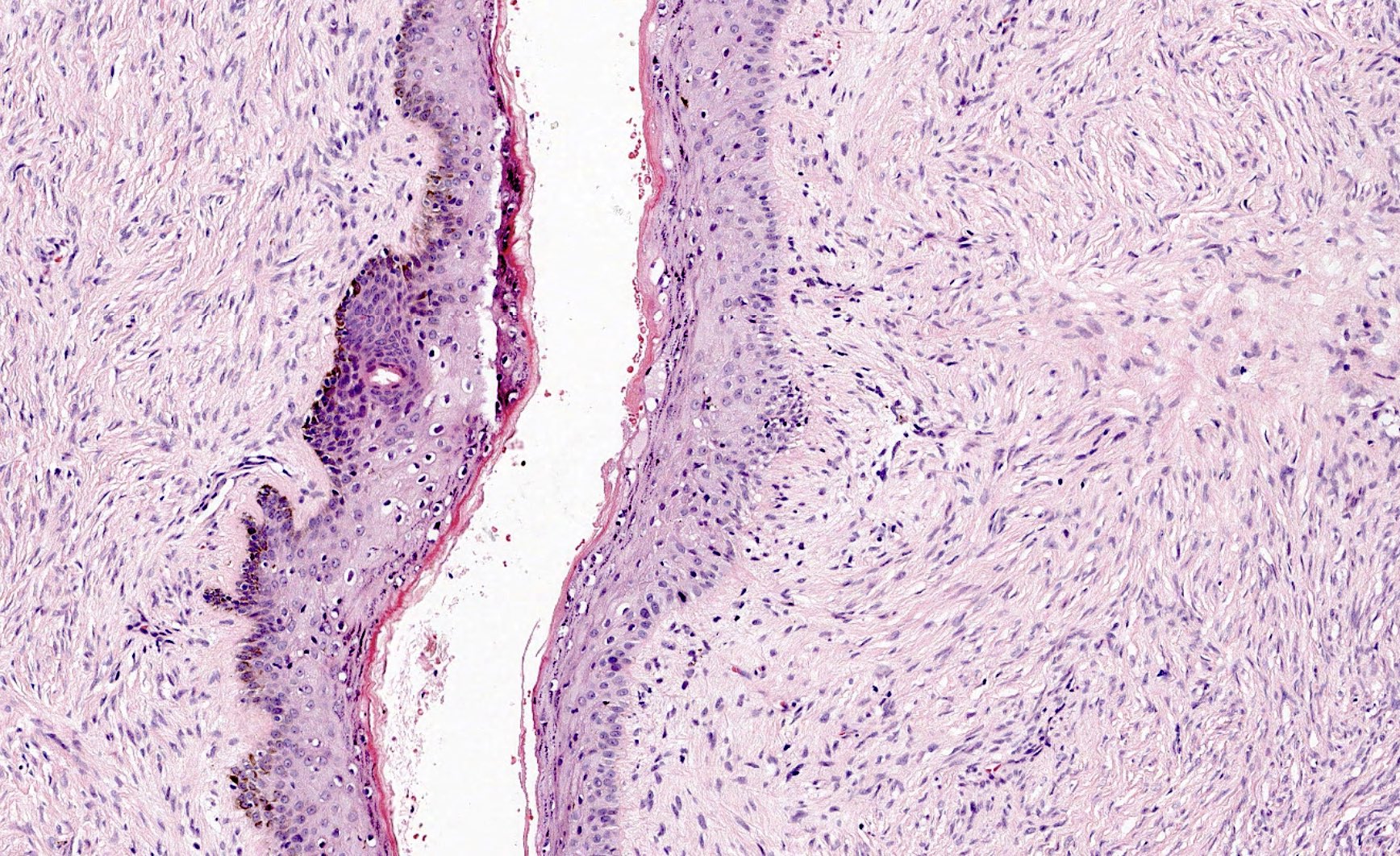
- Perineurium: surrounds individual fascicles of nerve fibers
- Continuous with the leptomeningeal layers of the CNS (i.e., arachnoid and pia) (Standring: Gray's Anatomy - The Anatomical Basis of Clinical Practice, 42nd Edition, 2020)
- 7 - 8 layers of connective tissue with dense fibroblasts
- Forms blood / nerve barrier and protects against foreign substances
- Last layer to break when a nerve is subjected to traction
- Contains specialized myoepithelial cells
- Endoneurium: intrafascicular connective tissue that surrounds nerve fibers
- Plays a role in maintaining a slight positive fluid pressure and constant environment for the nerve
- Contains a dense matrix of collagen, fibroblasts and reticular fibers
- Endoneurial tube is made of basal laminar sheets arranged around the axon Schwann cells units
- Epineurium: forms the sheath that surrounds all peripheral nerve trunks (i.e., whole nerve)
Diagrams / tables
Clinical features
- Pathologic or hypertrophic scar formation occurs as the result of excessive proliferation of fibroblasts and subsequent deposition of excess ECM (Int Wound J 2023;20:2190)
- Nerve can be acutely damaged via stretching, compression or laceration
- Indications for peripheral nerve surgery include nerve entrapment, nerve sheath tumor, acute injury and trauma
- Demyelination of nerves within the peripheral nervous system can occur via autoimmune processes resulting in polyneuropathy
- Axon degeneration and loss can occur as a result of metabolic conditions (e.g., diabetes, organ failure, nutritional deficiency) and most often present as peripheral neuropathy (Expert Rev Neurother 2008;8:1807)
- Axon degeneration (i.e., Wallarian degeneration) occurs in the distal portion of an axon if the axon is severed, thus separating it from its cell body; this degeneration occurs due to the lack of ribosomes within the axon and the discontinuation of axonal flow to the severed portion of the cell
Gross description
- Fibrous connective tissue is found throughout the body and supports various organs and cells (StatPearls: Anatomy, Connective Tissue [Accessed 11 October 2024])
- Dense, irregular connective tissue appears grossly as tough, white or web-like tissue with multidirectional fibers; it is often seen as fibrous sheets that provide strength and support
- Forms the capsules that enclose organs (Suvarna: Bancroft's Theory and Practice of Histological Techniques, 7th Edition, 2012)
- Found in deep layers of skin and comprises most fascia
- Dense, regular connective tissue appears grossly as a white, flexible tissue with unidirectional, parallel fibers running in the direction of the force exerted on the body part where it is located (Stecco: Functional Atlas of the Human Fascial System, 1st Edition, 2015)
- Comprises tendons and ligaments; fibers have a high density parallel arrangement
- Deep fascia (e.g., thoracolumbar) (Surg Radiol Anat 2011;33:855)
- Epimysium and perimysium (J Bodyw Mov Ther 2010;14:411)
- Scar tissue is fibrous tissue that appears firm, hypopigmented or discolored, sometimes slightly raised and with an irregular texture
- Dense, irregular connective tissue appears grossly as tough, white or web-like tissue with multidirectional fibers; it is often seen as fibrous sheets that provide strength and support
- Nerves appear grossly as cord-like, solid, white bands embedded in adipose or other connective tissue
- When transected the myelin may be apparent as a white-yellow fatty substance, especially in larger nerves
Gross images
Microscopic (histologic) description
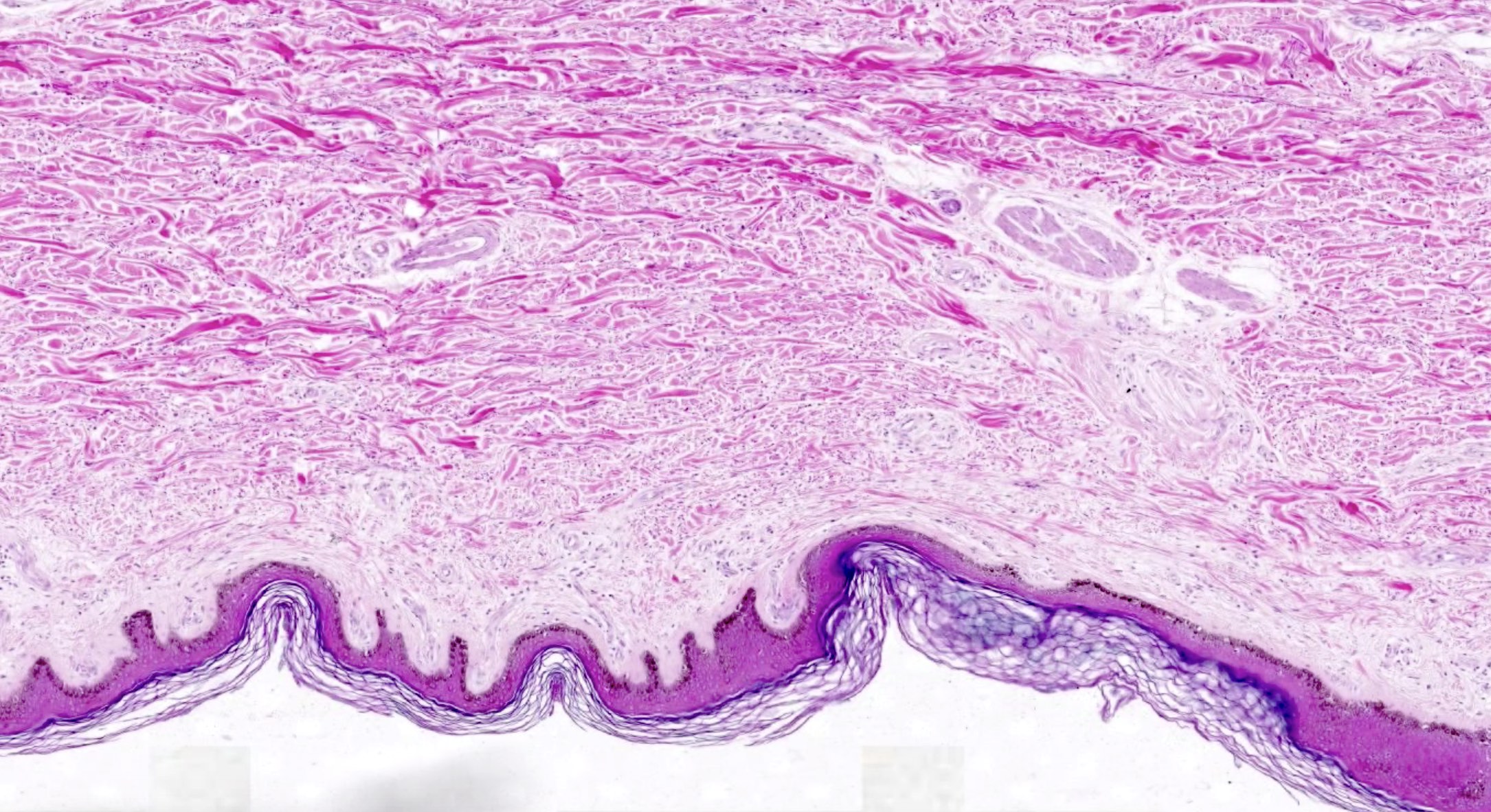
- Fibroblasts
- Spindle shaped along collagen fibers and stellate in myxoid areas
- Distinct nucleus with long, thin, pale staining processes
- Not easily observed on standard light microscopy (only fibroblast nuclei and collagen are typically seen)
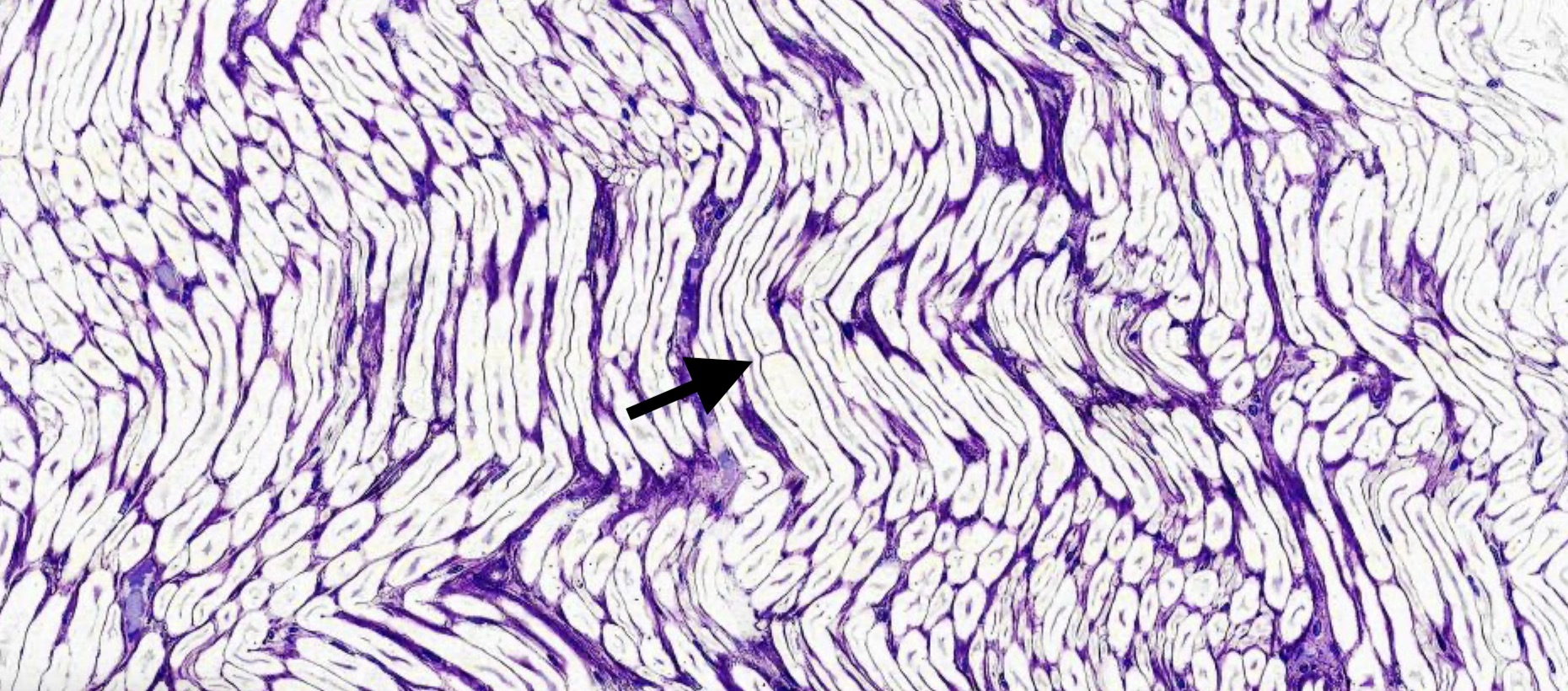
- Axons (StatPearls: Histology, Axon [Accessed 11 October 2024])
- Cylindrical structure; progressively tapers toward synaptic terminal end and may occasionally bifurcate
- Diameter range: 1 - 25 μM; propagation speed is directly proportional to the diameter of the axon
- No rough endoplasmic reticulum in the axon (only in the cell body / soma)
- Interneurons have a reduced amount of cytoplasm / axoplasm
- Axons can be myelinated or nonmyelinated
- Myelin / Schwann cells (StatPearls: Histology, Schwann Cells [Accessed 11 October 2024])
- Myelin is formed by concentric wrapping of plasma membrane of Schwann cells around an axon
- Nodes of Ranvier are gaps in the myelin sheath between adjacent Schwann cells; the axon is unmyelinated in these gaps and allows for saltatory conduction and a faster propagation of the action potential
- Can be visualized microscopically as a membrane demarcation between Schwann cells; gaps are not usually apparent
Microscopic (histologic) images
Contributed by Nicole Stringham, Ph.D. (source: Duke University virtual slide collection and University of Michigan virtual slide box)
Positive stains
- Fibroblasts: vimentin (intense, 100%), IB10 (weak, 100%), 5B5 (moderate to intense, 90 - 100%), smooth muscle actin (100% lung, 10% dermal), TE7 (moderate, 50%; in formalin / paraffin) (J Histochem Cytochem 2008;56:347)
- Peripheral nerve: toluidine blue (J Vis Exp 2018;137:58031)
- Motor axons: ChAT (J Transl Med 2021;19:207)
- Primary afferent neurons: CGRP
- Peptidergic and nonpeptidergic nociceptors: TVRP1
- Axon specific intermediate filament: NF200
- Myelin sheath: osmium tetroxide (J Vis Exp 2018;137:58031)
- Perineurial cells: EMA
- Schwann cells: S100 (strong)
Negative stains
- Fibroblasts: CD68 (Verh Dtsch Ges Pathol 2003;87:215)
- Immunofluorescence can distinguish fibroblast (alpha smooth muscle actin [αSMA] negative) from myofibroblast, which is αSMA positive (with the exception of protomyofibroblasts, which do not express SMA) (Nat Rev Mol Cell Biol 2002;3:349)
- Perineurial cells: S100
Electron microscopy description
- Fibroblasts and collagen
- Fibroblasts have abundant rough endoplasmic reticulum and Golgi apparatus as well as a nuclei rich in euchromatin (StatPearls: Histology, Fibroblast [Accessed 10 October 2024], Arch Dermatol Res 2017;309:389)
- Proximity of fibroblast to collagen fibers can be easily seen, both in longitudinal and transverse sections
- Nerve and glia
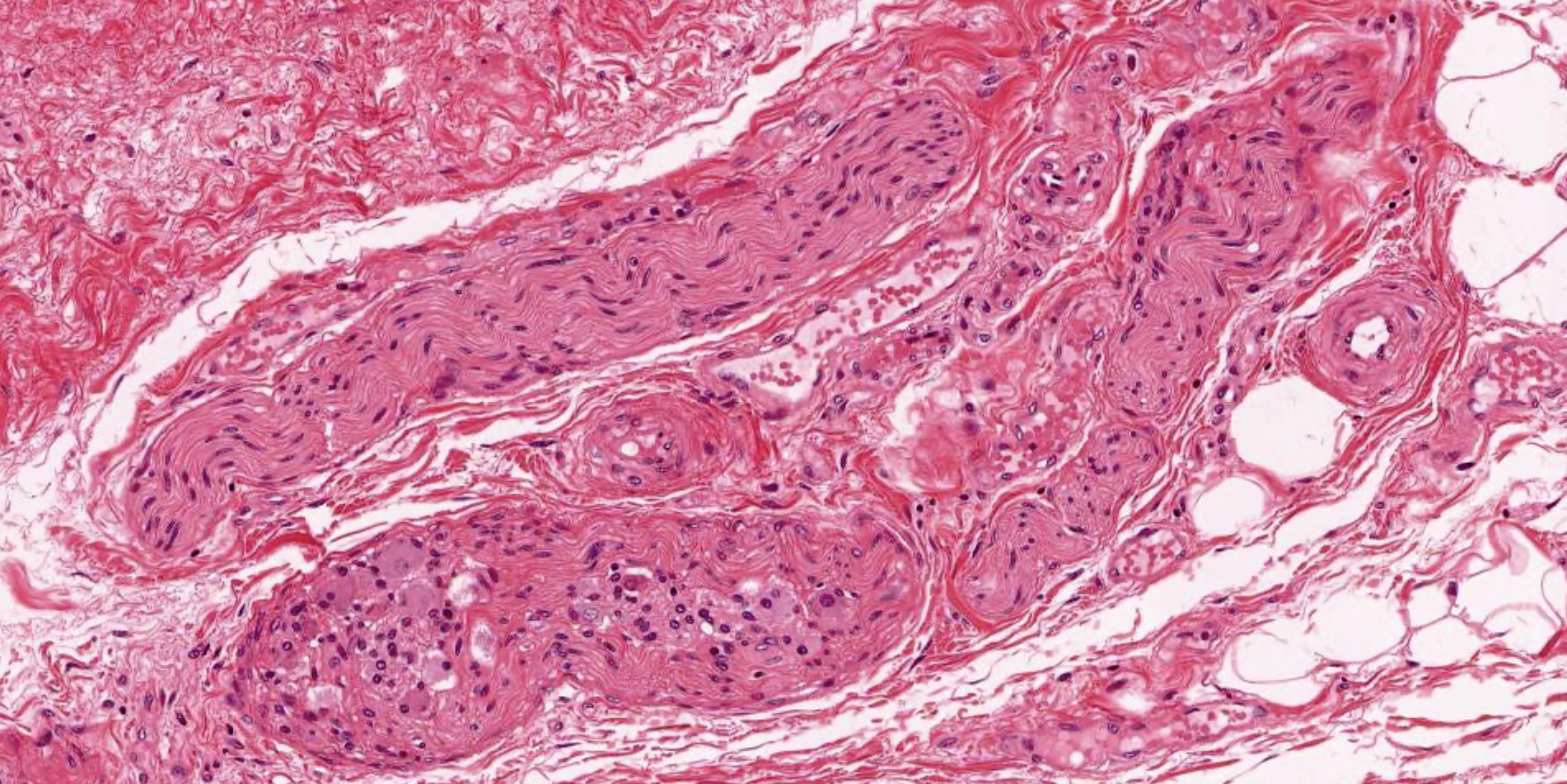
- Parallel bundles of nerve fibers (axons) arranged in fascicles
- Connective tissue wraps each fascicle (perineurium) and surrounds each nerve (epineurium)
- Blood vessels are seen in the space between fascicles
- Interdigitating Schwann cell processes are frequently seen (J Neurosci 2004;24:9250)
Electron microscopy images
Videos
Connective tissue overview
Histology of nerve
Peripheral nerve
Board review style question #1
A 25 year old man is found to have a hypertrophic scar at the site of a previous laparoscopic surgery. Biopsy of the lesion demonstrates histology shown in the image above. Which of the following cell types is primarily responsible for the formation of this lesion?
- Epidermal keratinocytes
- Fibroblasts
- Granulocytes
- Melanocytes
- Myofibroblasts
Board review style answer #1
B. Fibroblasts are primarily responsible for the pathological formation of hypertrophic (keloid) scars due to their production of excess collagen during wound healing. Answer A and D are incorrect because although epidermal keratinocytes and melanocytes overlie the lesion, they are not responsible for the scar overgrowth. Answer C is incorrect because while granulocytes are involved in wound healing and inflammation, they are not directly responsible for scar formation. Answer E is incorrect because although myofibroblasts reside in the middle dermis of keloid scars and are thought to contribute to pathological scar formation, they are not the primary collagen producing cell type that form these lesions (Front Med (Lausanne) 2024;11:1293028).
Comment Here
Reference: Histology-fibrous tissue & nerve
Comment Here
Reference: Histology-fibrous tissue & nerve
Board review style question #2
Which of the following components of a peripheral nerve is continuous with the dura mater of the central nervous system (CNS)?
- Endoneurium
- Epineurium
- Myelin sheath
- Perineurium
Board review style answer #2
B. Epineurium is the most superficial connective tissue covering of peripheral nerve and is continuous with the dura mater of the central nervous system. Answer A is incorrect because endoneurium is the deepest layer of connective tissue within a nerve and surrounds the nerve fibers within the nerve fascicles. Answer C is incorrect because the myelin sheath is formed by glia that, together with the axon, form each nerve fiber. Answer D is incorrect because perineurium surrounds each nerve fascicle and is continuous with the leptomeningeal layers (i.e., pia and arachnoid) of the CNS.
Comment Here
Reference: Histology-fibrous tissue & nerve
Comment Here
Reference: Histology-fibrous tissue & nerve