Table of Contents
Definition / general | Essential features | Terminology | ICD coding | Epidemiology | Sites | Pathophysiology | Etiology | Clinical features | Diagnosis | Case reports | Treatment | Clinical images | Microscopic (histologic) description | Microscopic (histologic) images | Positive stains | Negative stains | Electron microscopy description | Videos | Sample pathology report | Differential diagnosis | Additional references | Board review style question #1 | Board review style answer #1 | Board review style question #2 | Board review style answer #2Cite this page: Kramer K, Logemann NF. Sclerotic fibroma. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/skintumornonmelanocyticsclerosingfibroma.html. Accessed April 3rd, 2025.
Definition / general
- Benign neoplasm of thickened collagen bundles in a characteristic storiform pattern with CD34+ spindle cell component (Am J Surg Pathol 2024;48:150)
Essential features
- Solitary or in association with Cowden syndrome (CS) (Am J Surg Pathol 2024;48:150, J Am Acad Dermatol 1989;20:266)
- Whorled collagen bundles with a plywood or starry night appearance (J Cutan Pathol 2008;35:74)
- CD34+ (Am J Surg Pathol 2024;48:150)
Terminology
- Storiform collagenoma (Am J Dermatopathol 1991;13:122)
- Plywood fibroma (J Cutan Pathol 2008;35:74)
- Hypocellular fibroma
- Circumscribed, storiform collagenoma
ICD coding
Epidemiology
- Solitary lesions present in adults of either sex (J Am Acad Dermatol 1989;20:266)
- Multiple lesions can be associated with Cowden syndrome (Am J Surg Pathol 2024;48:150, J Am Acad Dermatol 1989;20:266)
Sites
- Wide anatomic distribution including trunk, extremities and mucosal surfaces (Br J Oral Maxillofac Surg 2020;58:231, J Am Acad Dermatol 1989;20:266)
Pathophysiology
- PTEN (phosphate and tensin homolog) alterations (Am J Surg Pathol 2024;48:150)
- Cowden associated with germline mutations
- Sporadic cases also demonstrate PTEN alterations
- PTEN is a tumor suppressor gene that regulates a number of cellular processes
- Recurrent activating mutations in PDGFRB (platelet derived growth factor receptor beta) (Am J Surg Pathol 2024;48:150)
- PDGFRB is a receptor tyrosine kinase involved in the regulation of cell proliferation and migration
Etiology
- Proliferating neoplasm with type I collagen synthesis and deposition (Am J Dermatopathol 1995;17:339)
- PTEN mutations in both sporadic and Cowden syndrome associated lesions (Am J Surg Pathol 2024;48:150)
Clinical features
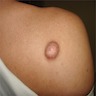
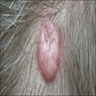
- 0.5 - 3 cm skin colored papules or plaques (Br J Dermatol 2003;149:433, Am J Dermatopathol 2004;26:519, J Am Acad Dermatol 1989;20:266)
- Trunk, extremities or mucosal surfaces (Am J Dermatopathol 2004;26:519, J Am Acad Dermatol 1989;20:266)
- Solitary or multiple (J Am Acad Dermatol 1989;20:266)
- Cowden syndrome is a PTEN hamartoma tumor syndrome (PHTS), a group of autosomal dominant disorders characterized by mutations in PTEN, a negative regulator of the PIK3 / AKT and mTOR pathways
- Cowden syndrome cutaneous findings include sclerotic fibromas, facial trichilemmomas, punctate palmoplantar keratoses, keratotic papules and lipomas
- While sclerotic fibromas can be seen in Cowden syndrome, they are not major diagnostic criteria; the diagnostic criteria are below
- Major criteria
- Breast cancer
- Endometrial cancer
- Follicular carcinoma of the thyroid gland
- Gastrointestinal hamartomas (including ganglioneuromas but excluding hyperplastic polyps; ≥ 3)
- Adult onset Lhermitte-Duclos disease
- Macrocephaly (> 97th percentile: 58 cm in women and 60 cm in men)
- Macular pigmentation of the glans penis
- Multiple mucocutaneous lesions (any of the following)
- Multiple trichilemmomas (≥ 3, at least 1 biopsy proven)
- Acral keratoses (≥ 3, palmoplantar keratotic pits or acral hyperkeratotic papules)
- Mucocutaneous neuroma (≥ 3)
- Oral papillomas (≥ 3, particularly on gingiva and tongue)
- Minor criteria
- Autism spectrum disorder
- Colorectal cancer
- Esophageal glycogenic acanthosis (≥ 3)
- Lipoma (≥ 3)
- Intellectual disability (IQ ≤ 75)
- Renal cell carcinoma
- Testicular lipomatosis
- Thyroid cancer (papillary carcinoma or follicular variant of papillary)
- Thyroid structural lesions (adenoma, adenomatous goiter, etc.)
- Vascular anomalies (e.g., multiple developmental venous anomalies)
- Diagnosis of Cowden syndrome is established if the patient fulfills 1 of the following criteria
- 3 or more major criteria, one of which is macrocephaly, adult onset Lhermitte-Duclos disease or gastrointestinal malrotation
- 2 or more major criteria and 3 or more minor criteria
- Patient's family members would be diagnosed with Cowden syndrome / PTEN hamartoma tumor syndrome if they meet 1 of the following criteria
- 2 or more major criteria
- 1 major criterion and at least 2 minor criteria
- At least 3 subcriteria
- Major criteria
Diagnosis
- Punch, shave or excisional skin biopsy
Case reports
- 34 year old Japanese man with asymptomatic nodule (J Cutan Pathol 2008;35:74)
- 36 year old man with 1.5 cm fibrotic nodule on right suprascapular region (Einstein (Sao Paulo) 2015;13:103)
- 40 year old man with 1.5 cm lesion on the right temporal scalp (J Clin Aesthet Dermatol 2009;2:36)
- 60 year old woman with clinical basal cell carcinoma (Case #190)
Treatment
- Simple excision is curative
- Treatment is not required as these are benign
- Sclerotic fibromas are not in the diagnostic criteria for Cowden syndrome and their presence alone should not prompt genetic testing
- NCCN Clinical Practice Guidelines recommend PTEN genetic testing for the following cases (NCCN: Genetic / Familial High Risk Assessment: Breast, Ovarian, Pancreatic and Prostate [Accessed 24 December 2024])
- Relatives of families with known pathologic variants of the PTEN gene
- Patients with a history of Bannayan-Riley-Ruvalcaba syndrome
- Meets the diagnostic criteria for Cowden syndrome
- Patients who do not meet the clinical diagnostic criteria for Cowden syndrome but meet
- 2 or more major criteria (1 must be macrocephaly); or
- 3 major criteria without macrocephaly; or
- 1 major and at least 3 minor criteria; or
- At least 4 minor criteria
- PTEN pathogenic variant detected by tumor genomic testing on any tumor type in the absence of germline analysis
Clinical images
Microscopic (histologic) description
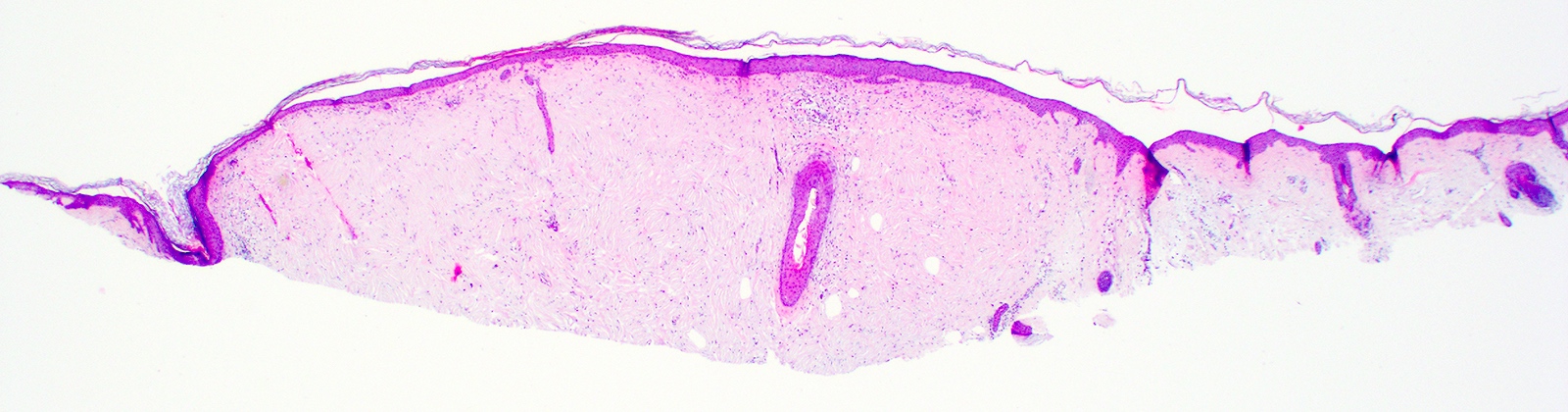
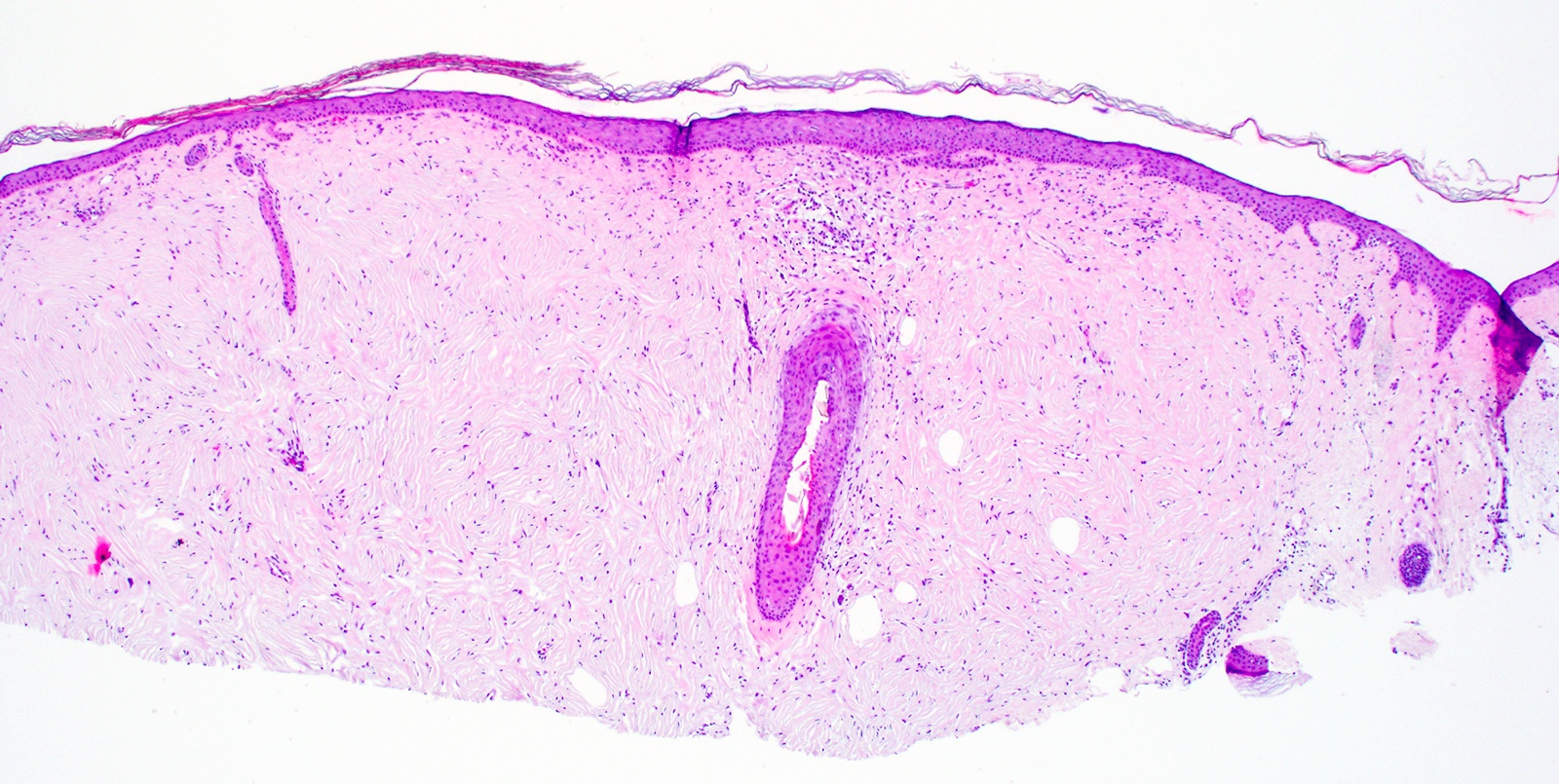
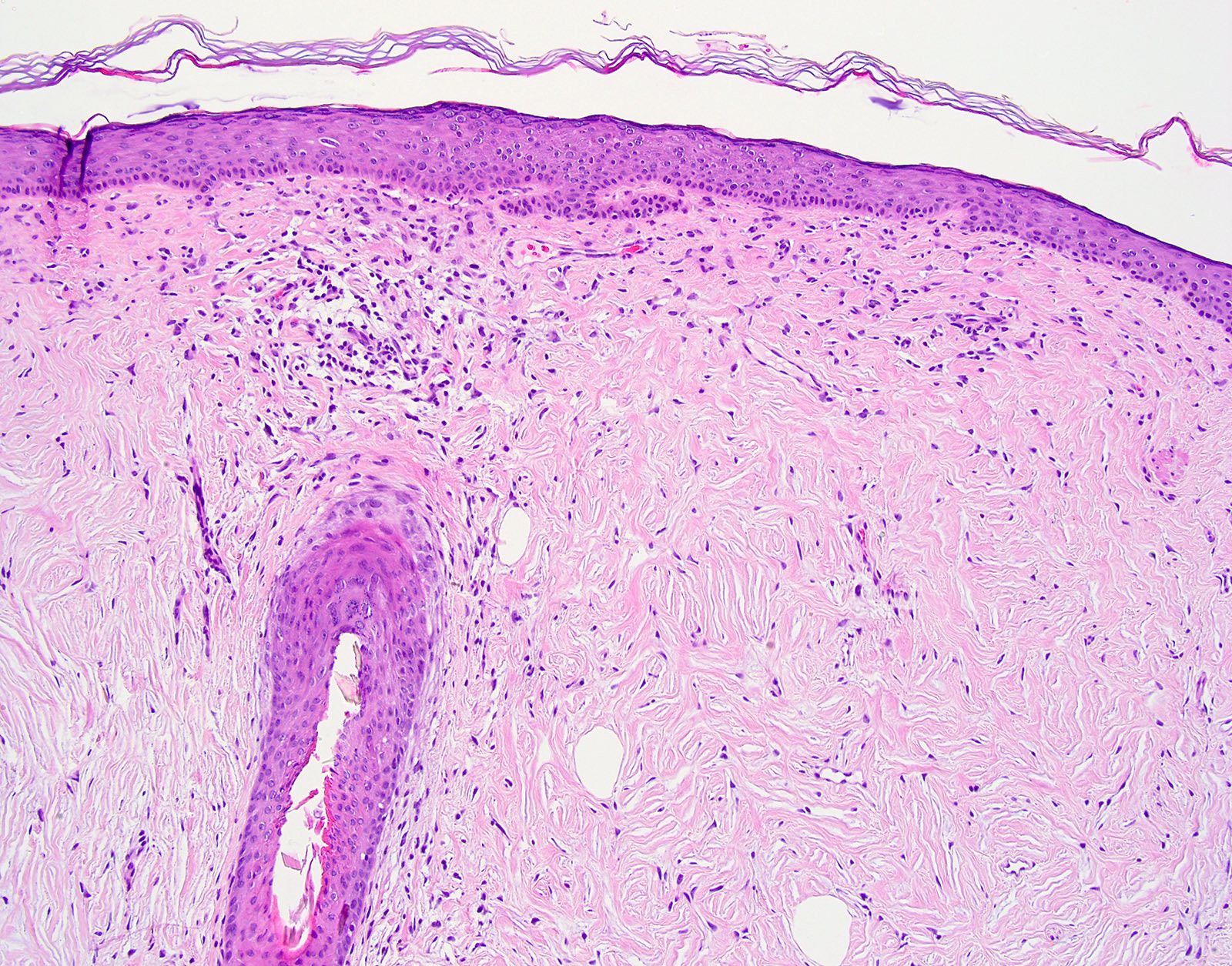
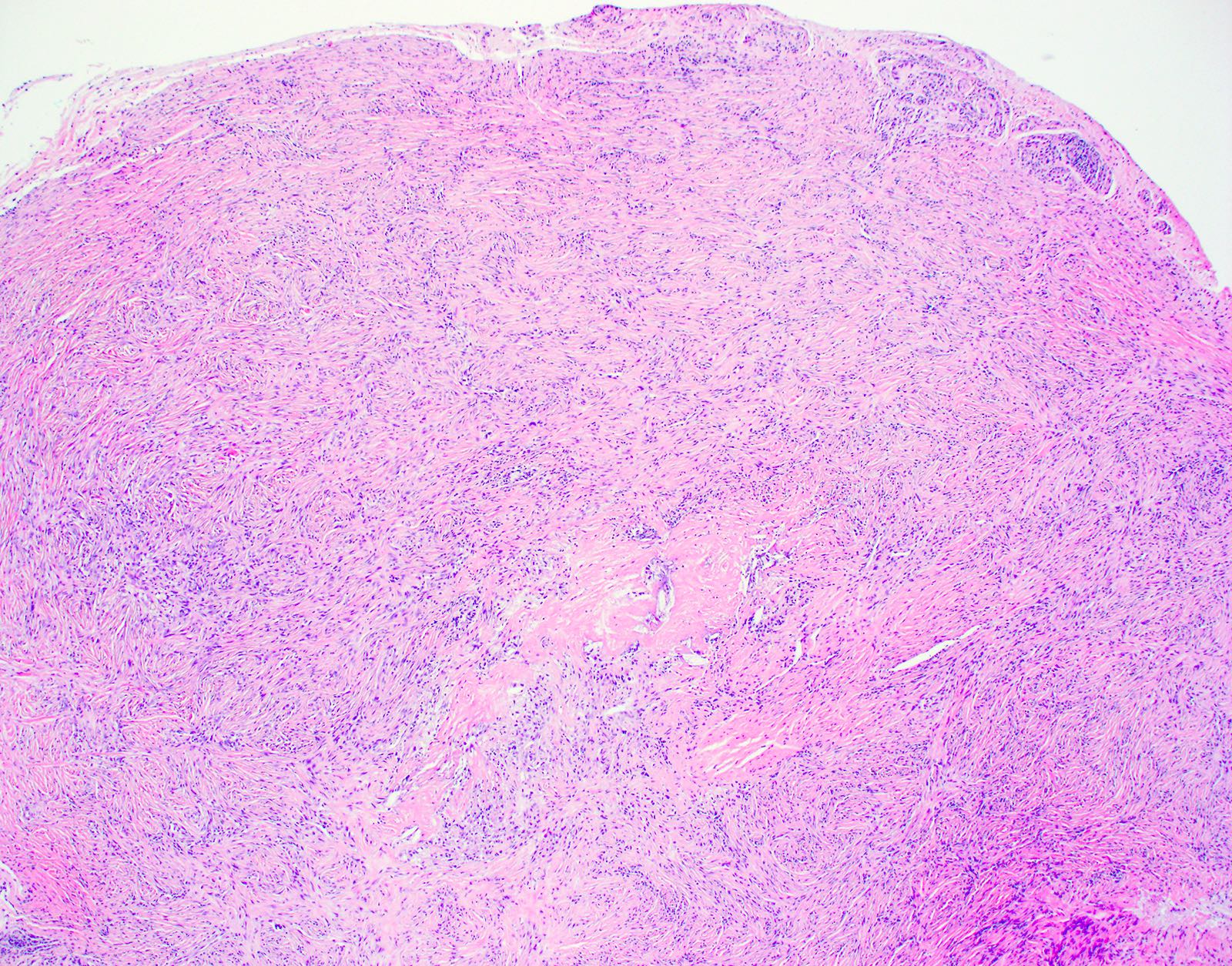
- Unencapsulated dermal nodule
- Attenuated overlying epidermis
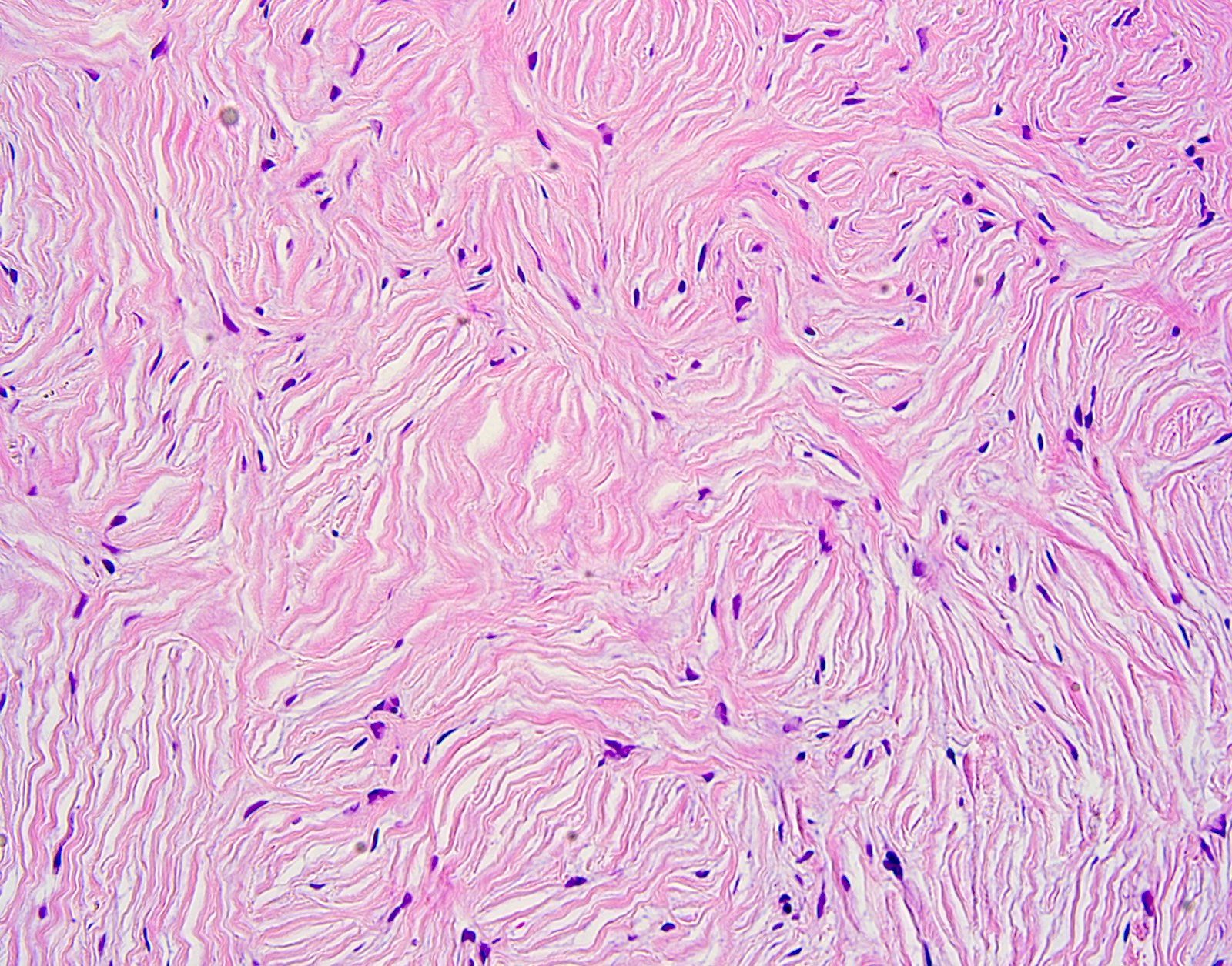
- Starry night or plywood appearance of whorled thickened collagen bundles (J Cutan Pathol 2008;35:74)
- Low cellularity
- Absent elastic fibers
- Stromal mucin may be present
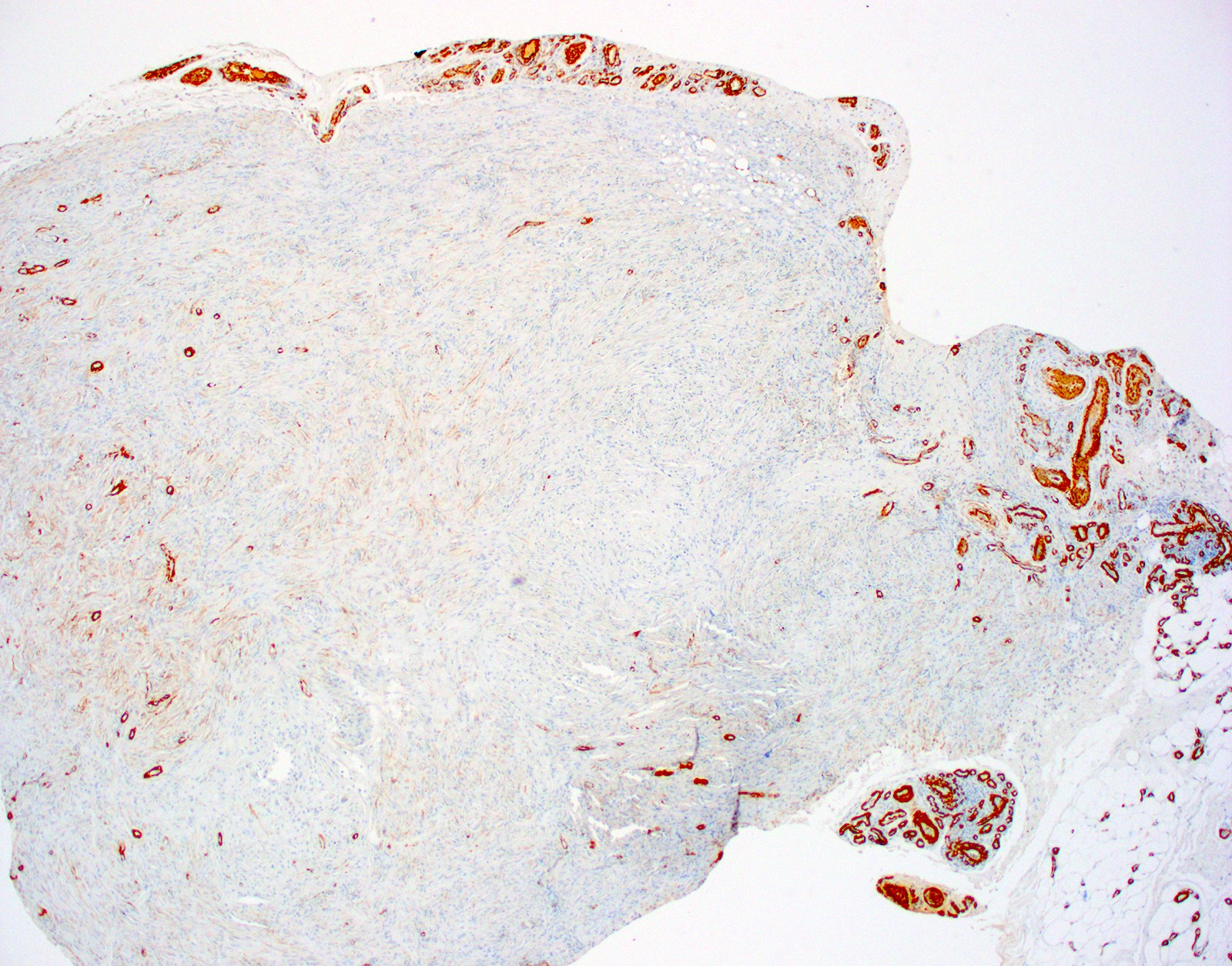
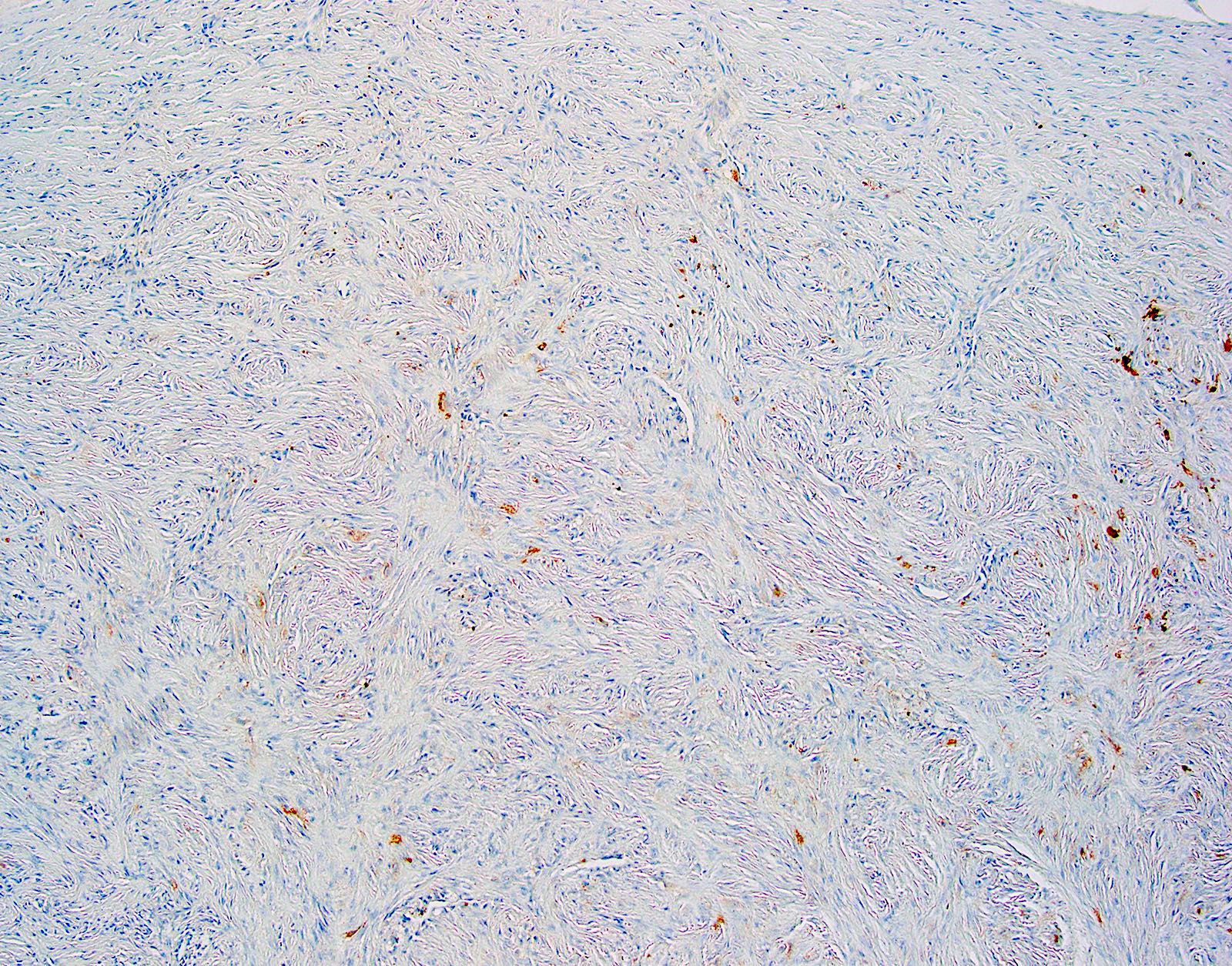
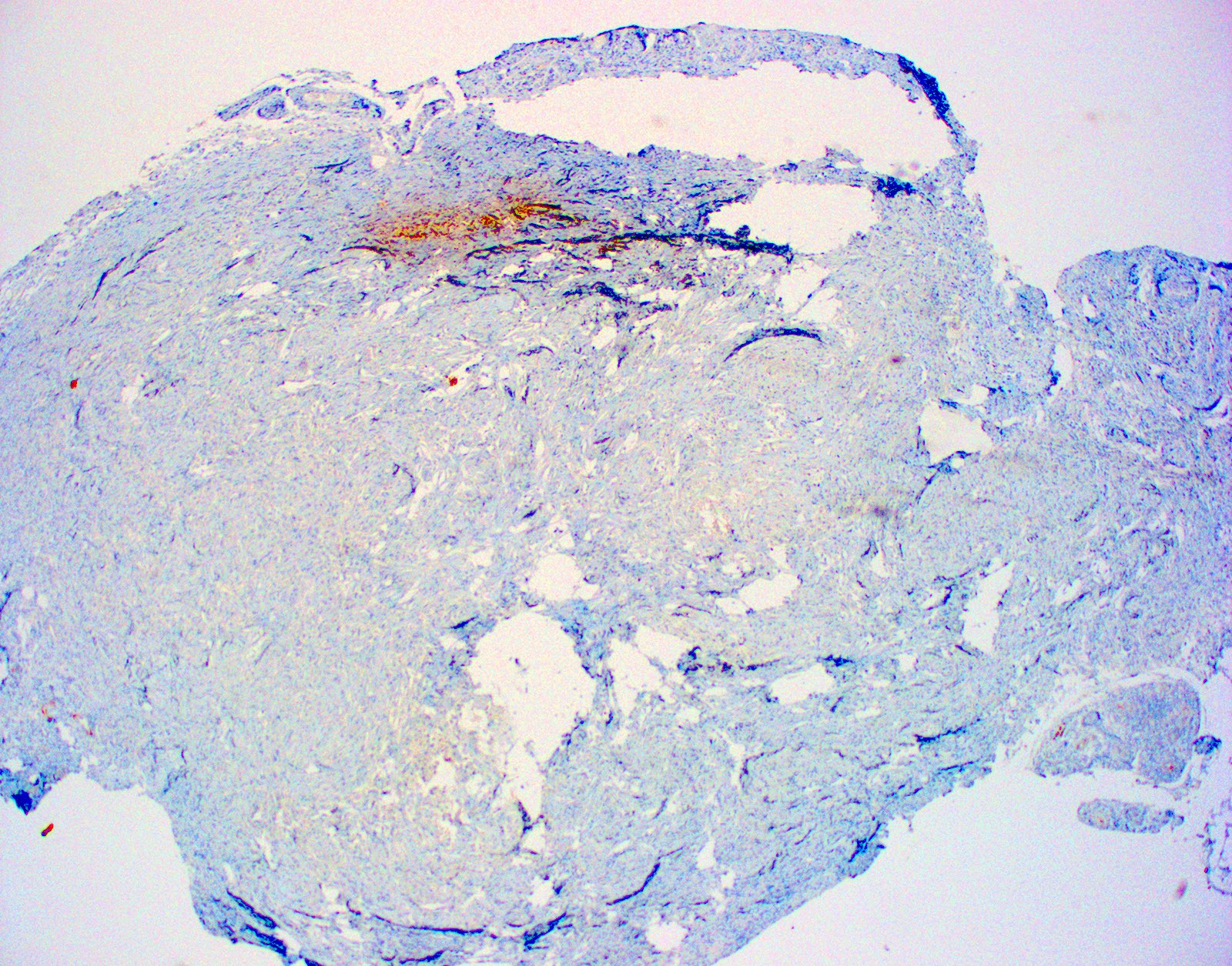
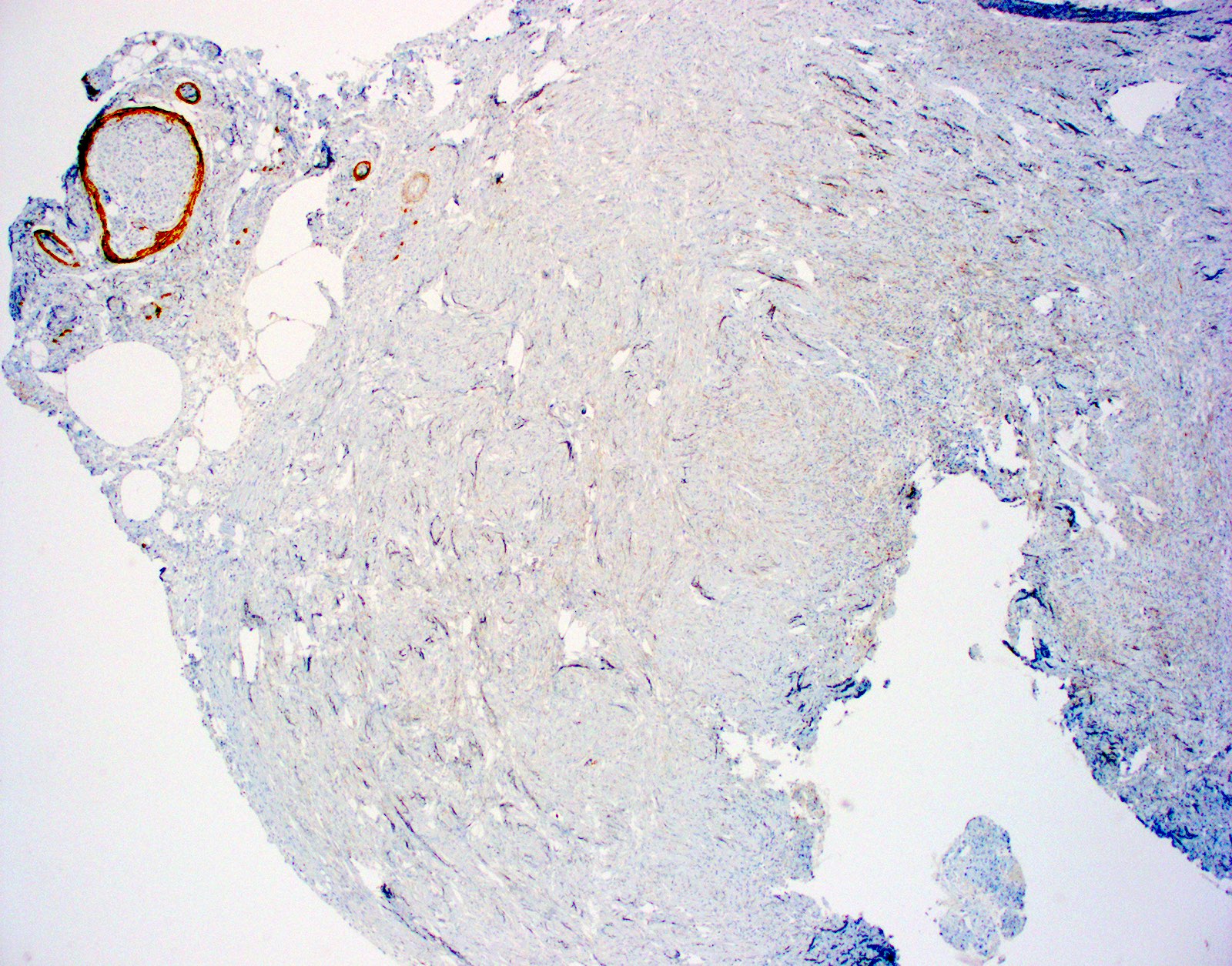
Microscopic (histologic) images
Positive stains
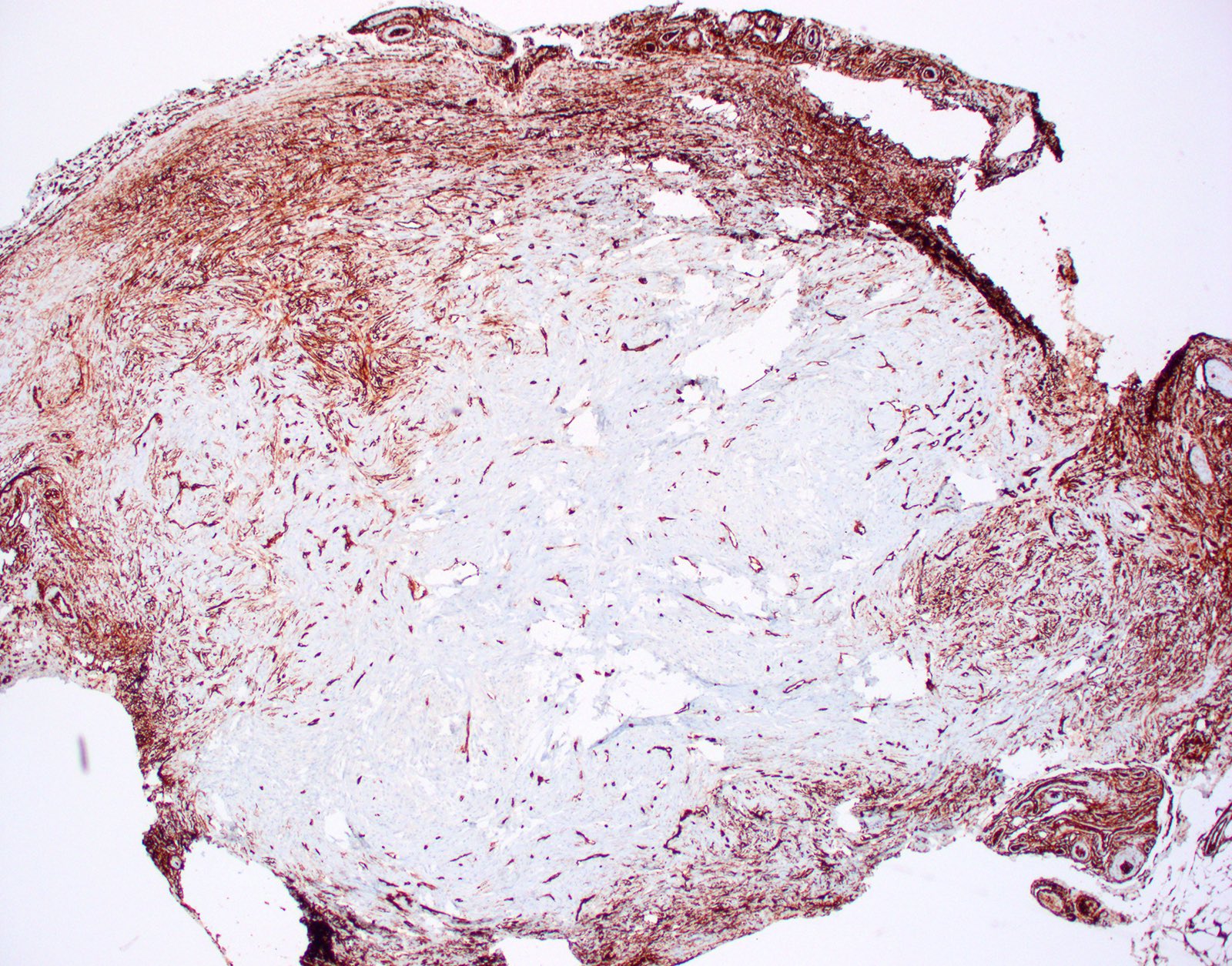
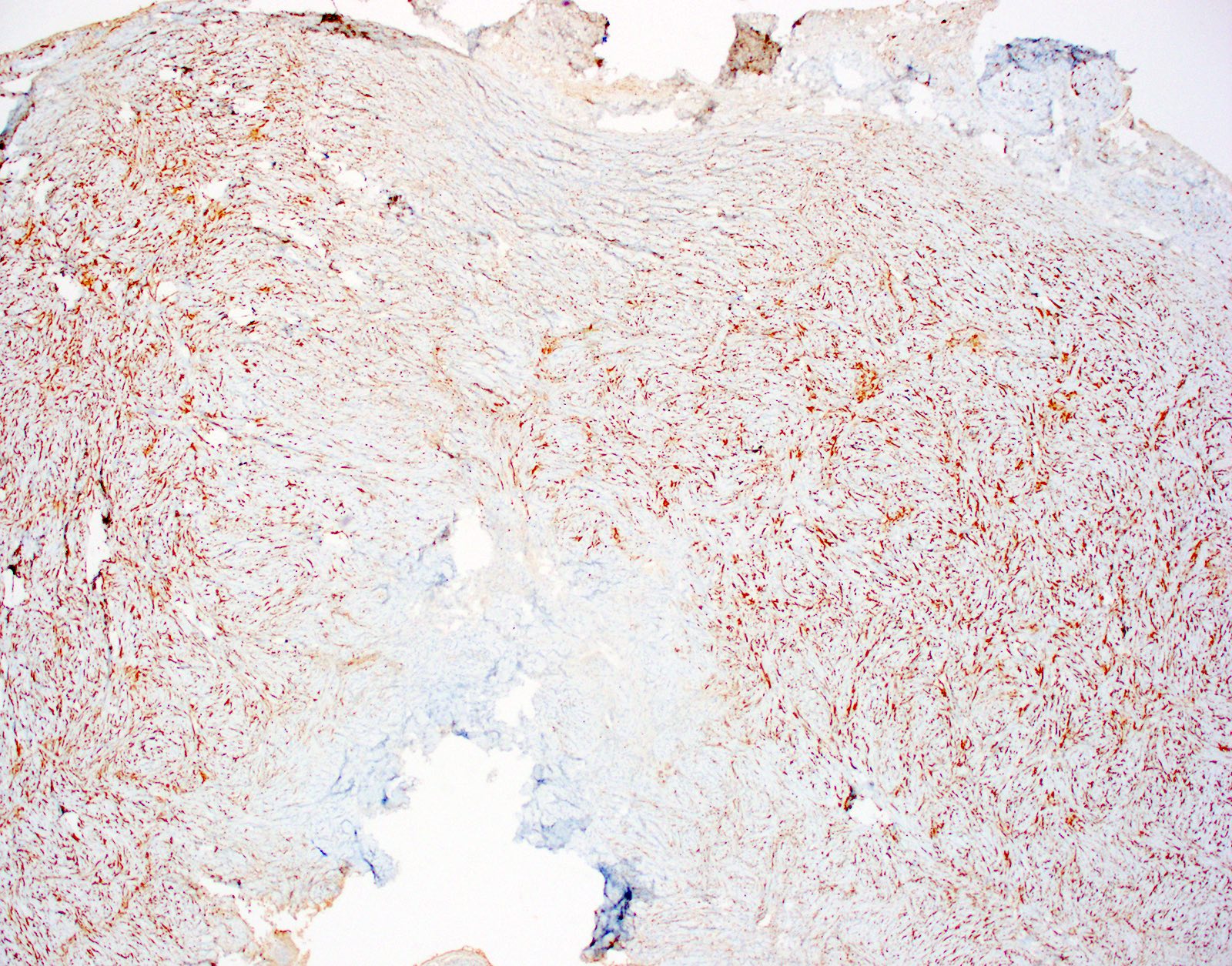
- CD34 (Am J Dermatopathol 1995;17:339, Am J Dermatopathol 2000;22:17, Histopathology 2002;41:134)
- Vimentin
- Actin / SMA variable weak to moderate positivity possible (J Cutan Pathol 2008;35:74)
- Factor XIIIa (Am J Dermatopathol 1991;13:122)
- CD99
Negative stains
Electron microscopy description
- Widened collagen bundles containing tightly bundled collagen fibrils
Videos
Sclerotic fibroma by Dr. Jerad Gardner
Sample pathology report
- Skin, punch biopsy:
- Sclerotic fibroma (see comment)
- Comment: Sections demonstrate whorls of collagen bundles.
Differential diagnosis
- Sclerotic perineurioma:
- These uncommon neural tumors can have similar architecture to sclerotic fibromas, with whorled dense connective tissue; however, they are more cellular than sclerotic fibromas, which demonstrate low cellularity
- Sclerotic perineuriomas stain positive for EMA, whereas sclerotic fibromas are negative for EMA
- Fibrolamellar nerve sheath tumor (Pacinian neurofibroma):
- These variants of Pacinian neurofibromas can also resemble the architecture of a sclerotic fibroma; however, fibrolamellar nerve sheath tumors demonstrate increased amounts of mucin, which is not seen in sclerotic fibromas
- Fibrolamellar nerve sheath tumors demonstrate scattered S100+ cells with small nuclei, whereas S100 is negative in sclerotic fibromas
- Occasional pigmented dendritic melanocytes can be seen in fibrolamellar nerve sheath tumors but not in sclerotic fibromas
- Dermatofibroma:
- Dermatofibromas are banal dermal spindle cell proliferations of fibroblasts with peripheral collagen trapping and overlying epidermal induction
- Dermatofibromas tend to have negative staining for PCNA and Ki67, whereas these indicators of proliferation have been reported positive in sclerotic fibromas, indicating a growing neoplasm
- Fibroma of the tendon sheath:
- Stroma of these tumors is hyalinized and whorled with artifactual clefting, which can resemble a sclerotic fibroma; however, they are found attached to tendon sheaths and never in the dermis where sclerotic fibromas are found
- Dermatofibrosarcoma protuberans (DFSP) - sclerosing variant (Am J Dermatopathol 2017;39:83):
- DFSPs are dermal tumors of spindle cells that extend deep into the subcutis
- They can have a storiform architecture but tend to be more cellular than sclerotic fibromas
- There are variants of DFSP described with more sclerotic changes and abundant collagen, which can make the diagnosis challenging
- Both sclerotic fibromas and DFSP typically stain positive for CD34, further complicating the challenge
- Negative factor XIIIa can help favor DFSP, whereas it is typically positive in sclerotic fibromas
- Clinically, DFSPs typically range in size from 2 to 5 cm, whereas sclerotic fibromas are typically smaller, ranging from 0.5 to 3 cm
- DFSP will demonstrate COL1A1::PDGFB fusion on FISH, whereas sclerotic fibromas will not
Additional references
Board review style question #1
A 38 year old man presents with a several month history of an asymptomatic skin colored papulonodule on the right side of his neck. On physical exam, he also has several skin colored papules on the face. A punch biopsy of the lesion of concern is obtained, which reveals plywood-like layers of collagen. Which syndrome may be associated with the tumor described?
- Birt-Hogg-Dubé syndrome
- Brooke-Spiegler syndrome
- Cowden syndrome
- Gardner syndrome
- Muir-Torre syndrome
Board review style answer #1
C. Cowden syndrome.
The lesion of concern described is a sclerotic fibroma (storiform collagenoma). These may occur sporadically or be associated with Cowden syndrome. Cowden syndrome is a PTEN hamartoma tumor syndrome (PHTS), a group of autosomal dominant disorders characterized by mutations in PTEN, a negative regulator of the PIK3 / AKT and mTOR pathways. Cowden syndrome cutaneous findings include sclerotic fibromas, facial trichilemmomas, punctate palmoplantar keratoses, keratotic papules and lipomas.
Answer E is incorrect because Muir-Torre syndrome is associated with sebaceous neoplasms, keratoacanthomas and colonic adenocarcinomas.
Answer D is incorrect because Gardner syndrome is associated with multiple fibromas, epidermoid cysts and lipomas.
Answer A is incorrect because Birt-Hogg-Dubé syndrome is associated with multiple fibrofolliculomas, trichodiscomas, renal cell carcinoma and spontaneous pneumothorax.
Answer B is incorrect because Brooke-Spiegler syndrome is associated with multiple cylindromas, trichoepitheliomas and basal cell carcinomas.
Comment Here
Reference: Sclerotic fibroma
Comment Here
Reference: Sclerotic fibroma
Board review style question #2
A 38 year old man presents with a several month history of an asymptomatic skin colored papulonodule on the right side of his neck. On physical exam, he also has several skin colored papules on the face. A punch biopsy of the lesion of concern is obtained, which reveals plywood-like layers of collagen. This patient is most at risk for which malignancy?
- Gastric adenocarcinoma
- Glioblastoma
- Invasive ductal carcinoma
- Non-small cell lung cancer
- Squamous cell carcinoma
Board review style answer #2
C. Invasive ductal carcinoma.
PTEN hamartoma syndromes (PHTS) are associated with breast cancer, primarily invasive ductal, endometrial and thyroid cancers most commonly. They can also be associated with other genitourinary, renal and gynecologic cancers, melanoma, dysplastic gangliocytoma of the cerebellum and colorectal carcinomas. National Comprehensive Cancer Network (NCCN) guidelines specify screening recommendations for breast, endometrial, thyroid, renal and colorectal cancers.
Answers D and E are incorrect because non-small cell lung cancer and squamous cell carcinoma have not been associated with PTEN hamartoma tumor syndrome.
Answer A is incorrect because gastric adenocarcinoma has not been associated with PTEN hamartoma tumor syndrome; colorectal carcinoma and benign GI polyps have been associated.
Answer B is incorrect because glioblastoma has not been associated with PTEN hamartoma tumor syndrome; dysplastic gangliocytoma of the cerebellum has been associated.
Comment Here
Reference: Sclerotic fibroma
Comment Here
Reference: Sclerotic fibroma