Table of Contents
Definition / general | Essential features | ICD coding | Epidemiology | Sites | Pathophysiology | Etiology | Clinical features | Diagnosis | Laboratory | Prognostic factors | Case reports | Treatment | Clinical images | Microscopic (histologic) description | Microscopic (histologic) images | Virtual slides | Immunofluorescence description | Positive stains | Electron microscopy description | Videos | Sample pathology report | Differential diagnosis | Additional references | Board review style question #1 | Board review style answer #1 | Board review style question #2 | Board review style answer #2Cite this page: Franklin M, Somach S. Granuloma annulare. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/skinnontumorgranulomaannulare.html. Accessed April 2nd, 2025.
Definition / general
- Idiopathic, self limited dermatosis typically characterized by erythematous papules and plaques and characterized histologically by palisaded or interstitial granulomatous inflammation
Essential features
- Benign, self limited dermatosis characterized by erythematous papules and plaques, classically in an arciform or annular configuration
- 2 classic morphologic patterns
- Palisaded granulomas with central necrobiosis (collagen degradation) with peripheral histiocytes and admixed lymphocytes
- Histiocytes intercalating among collagen bundles with interstitial mucin
- Associations with hyperlipidemia and diabetes mellitus
- No proven treatment for this recurring, idiopathic disease
ICD coding
- ICD-10: L92.0 - granuloma annulare
Epidemiology
- F:M = 2:1 (G Ital Dermatol Venereol 2008;143:359)
- Favors children (especially subcutaneous granuloma annulare / pseudorheumatoid nodule) and young adults (Ann Acad Med Singap 2000;29:714)
- Usually asymptomatic
Sites
- Classically extremities but virtually any site possible (J Am Acad Dermatol 2016;75:457)
- Pseudorheumatoid nodule (subcutaneous variant)
- Classically periarticular (J Pediatr Orthop 1993;13:582)
- Distal lower extremity, scalp (Pediatr Dev Pathol 1998;1:300)
Pathophysiology
- Delayed type hypersensitivity reaction plausible based on T cell subpopulations (Arch Dermatol 1983;119:125)
- Th1 cytokines (e.g. IFNγ, TNFα) (Arch Dermatol Res 2000;292:384)
- Sequestration of macrophages in dermis via macrophage inhibitory factor (Br J Dermatol 1976;95:481)
Etiology
- Numerous inciting factors reported
- Viral infections (J Am Acad Dermatol 2000;43:918)
- Arthropod bites (Biochem Int 1991;23:507)
- Ultraviolet radiation (Arch Dermatol 1990;126:830)
- Borrelia infection (J Cutan Pathol 2008;35:1050)
- HIV (Int J STD AIDS 2019;30:206)
- Medications (e.g. TNFα inhibitors) (Curr Health Sci J 2020;46:203)
- Paraneoplastic (J Am Acad Dermatol 2018;79:913)
Clinical features
- Variants
- Classic: localized, annularly arranged pink to red nonscaly macules or papules, sometimes forming arciform to annular plaques, favoring extremities
- Approximately 75% of cases (J Am Acad Dermatol 2016;75:457)
- Generalized: macules, papules, patches, plaques or nodules widely distributed over trunk and extremities
- Annular or nonannular
- Mean age: 51.7 years (J Am Acad Dermatol 1989;20:39)
- Associated with diabetes mellitus in 21% of cases (versus 9.7% in localized) (J Am Acad Dermatol 1989;20:39)
- 45% have lipid abnormalities (J Am Acad Dermatol 1989;20:39)
- Possible association with HLA-Bw35 (Br J Dermatol 1978;98:425)
- Deep variants
- Subcutaneous
- Pseudorheumatoid nodule / juxta-articular nodular
- Predominantly disease of childhood (J Pediatr Orthop 1993;13:582)
- Periarticular or scalp
- Not associated with connective tissue disease (Pediatrics 2001;107:E42)
- Patch
- Trunk and proximal extremities
- May be mistaken for mycosis fungoides, morphea or contact dermatitis (J Cutan Pathol 2020;47:785)
- F > M
- Rare
- Perforating (Case Rep Dermatol 2019;11:233)
- Palmoplantar (An Bras Dermatol 2018;93:878)
- Linear (J Dtsch Dermatol Ges 2012;10:434)
- Classic: localized, annularly arranged pink to red nonscaly macules or papules, sometimes forming arciform to annular plaques, favoring extremities
- F:M = approximately 2:1
- Favors children and young adults
- Usually asymptomatic
Diagnosis
- Histopathologic evaluation confirms diagnosis
Laboratory
- Associated with dyslipidemia and diabetes (Arch Dermatol 2012;148:1131)
Prognostic factors
- Self limited with 40 - 50% chance of recurrence (Lippincotts Prim Care Pract 1997;1:33)
- Generalized form may be more resistant to treatment (Dermatology 2020;236:369)
- Benign (Dermatology 2020;236:369)
Case reports
- 58 year old woman with generalized granuloma annulare treated unsuccessfully with tildrakizumab (JAAD Case Rep 2020;7:3)
- 59 year old man with photoinduced granuloma annulare confirmed by experimental exposure to UVA light (Actas Dermosifiliogr 2020 Oct 17 [Epub ahead of print])
- 62 year old man with granuloma annulare arising under systemic psoriasis therapy; successfully treated with adalimumab (JAAD Case Rep 2020;6:832)
- 74 year old woman with recalcitrant generalized granuloma annulare treated successfully with dupilumab (JAAD Case Rep 2020;7:1)
Treatment
- Largely ineffective (J Eur Acad Dermatol Venereol 2010;24:103)
- Topical or intralesional corticosteroids
- Cryotherapy
- Phototherapy (Photodermatol Photoimmunol Photomed 2005;21:68)
- Laser therapy
- Antimalarial medications
- TNFα inhibitors (also reported to incite disease) (J Drugs Dermatol 2011;10:1466)
- Fumaric acid esters
- Oral antibiotics
- Rifamicin, ofloxacin and minocycline (Indian J Dermatol Venereol Leprol 2015;81:35)
- Oral retinoids (Australas J Dermatol 2016;57:327)
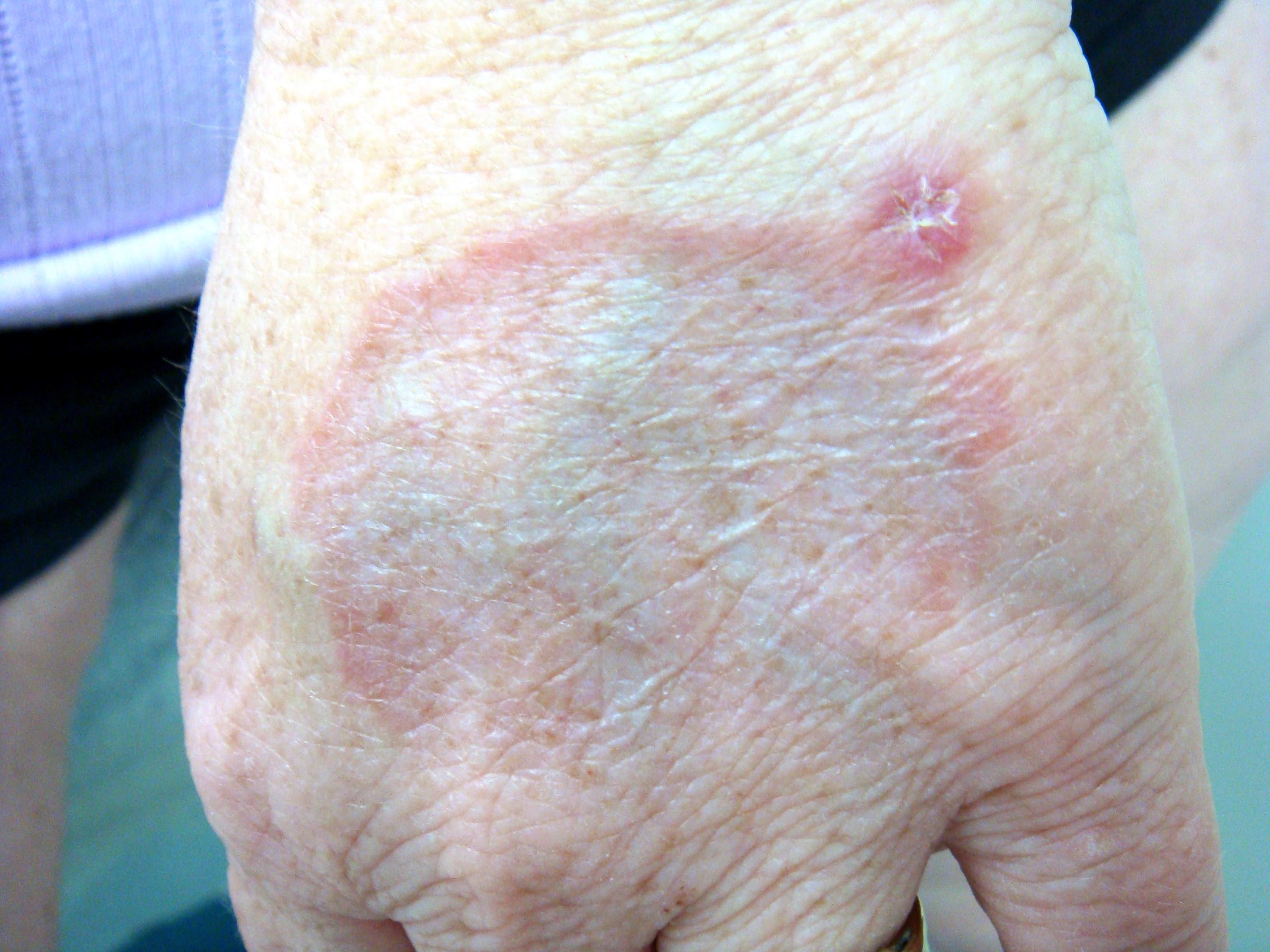
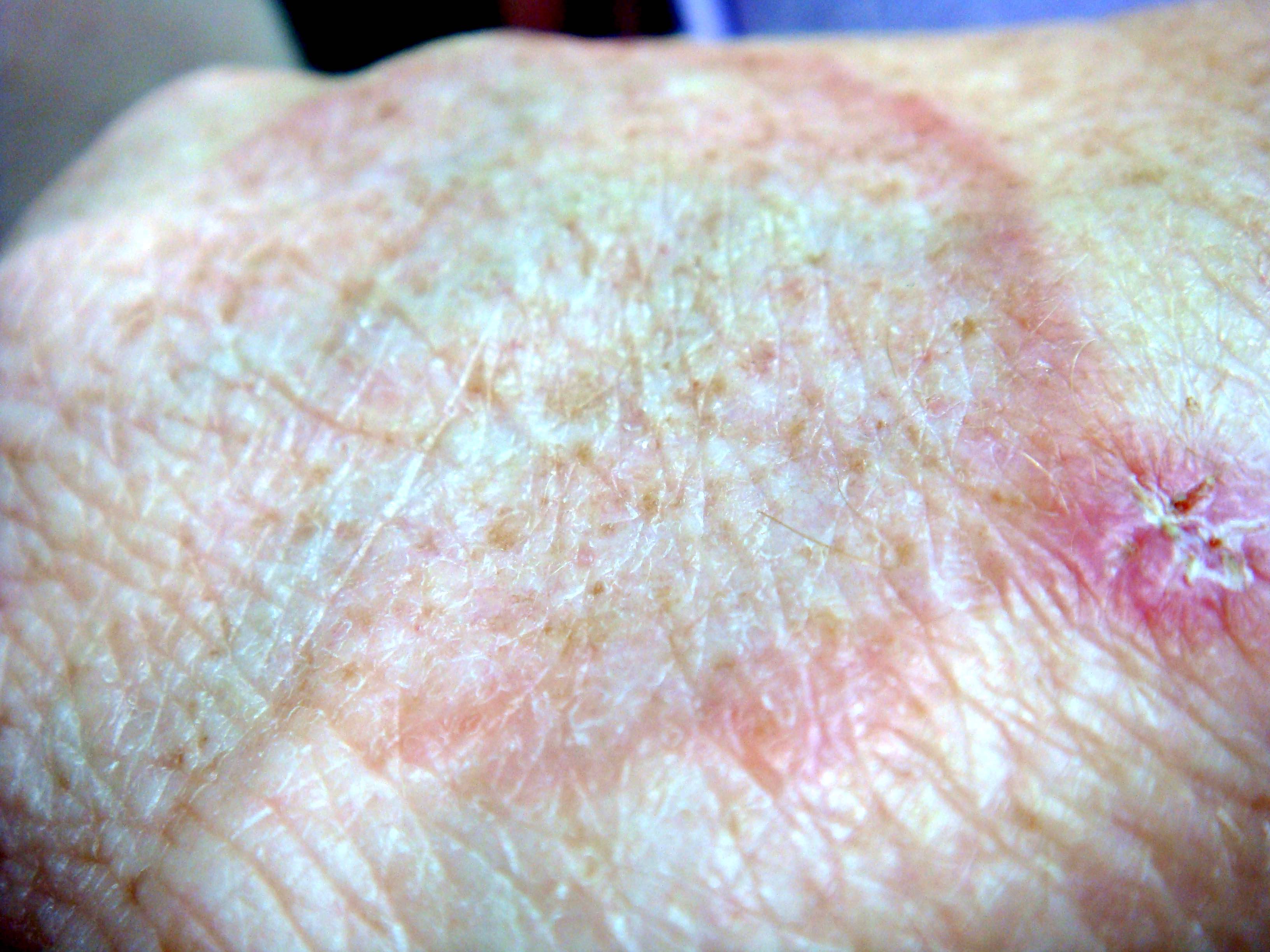
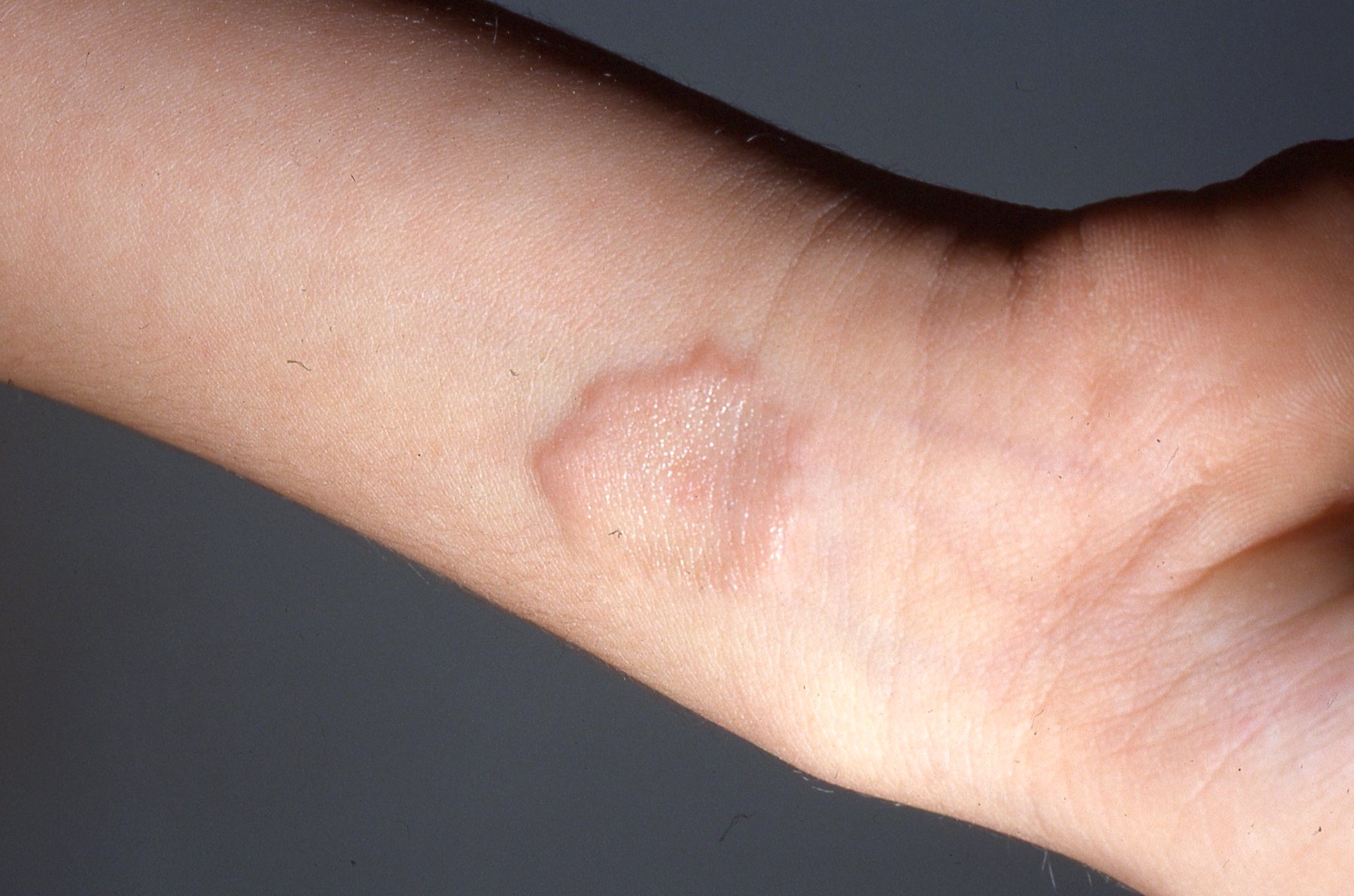
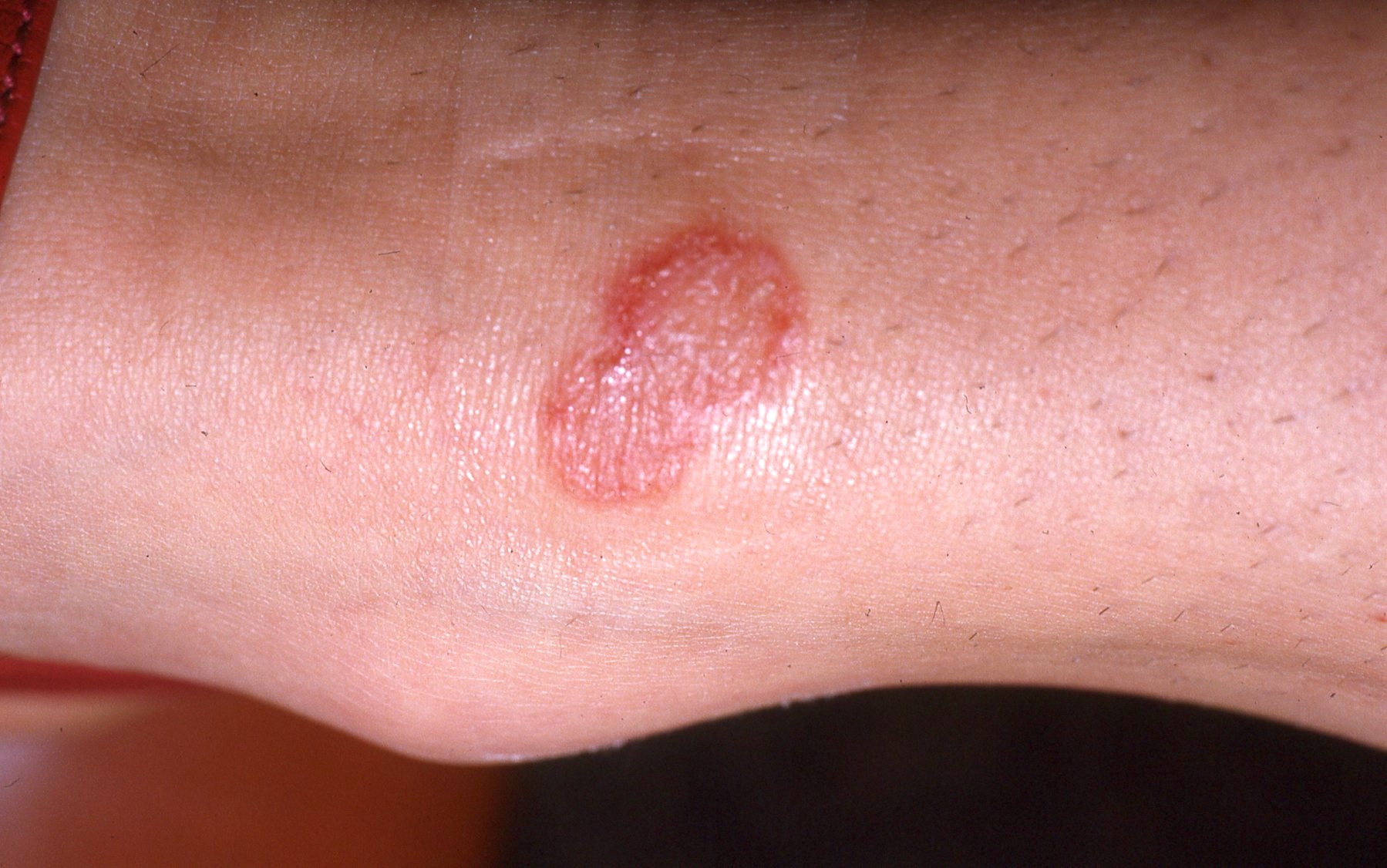
Clinical images
Microscopic (histologic) description
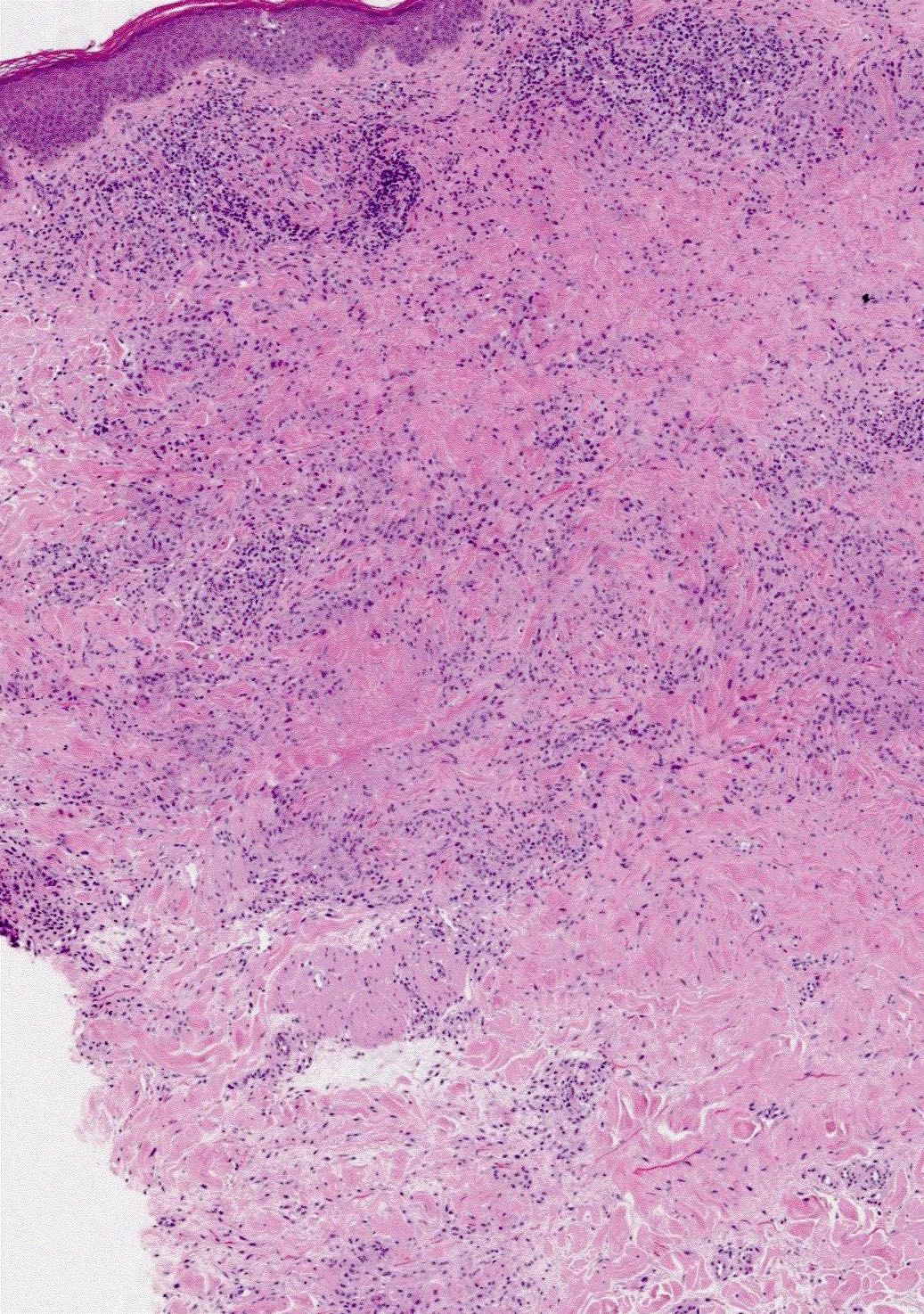
- Palisaded or interstitial granulomatous inflammation with mucin unites all forms (Arch Dermatol 1977;113:1681)
- Interstitial may be most common pattern (Indian Dermatol Online J 2018;9:409, Arch Dermatol 1977;113:1681)
- Variable histopathology
- Interstitial pattern may be associated with patch (rather than papular / plaque) presentation (J Am Acad Dermatol 2000;42:417, Br J Dermatol 2019;181:198)
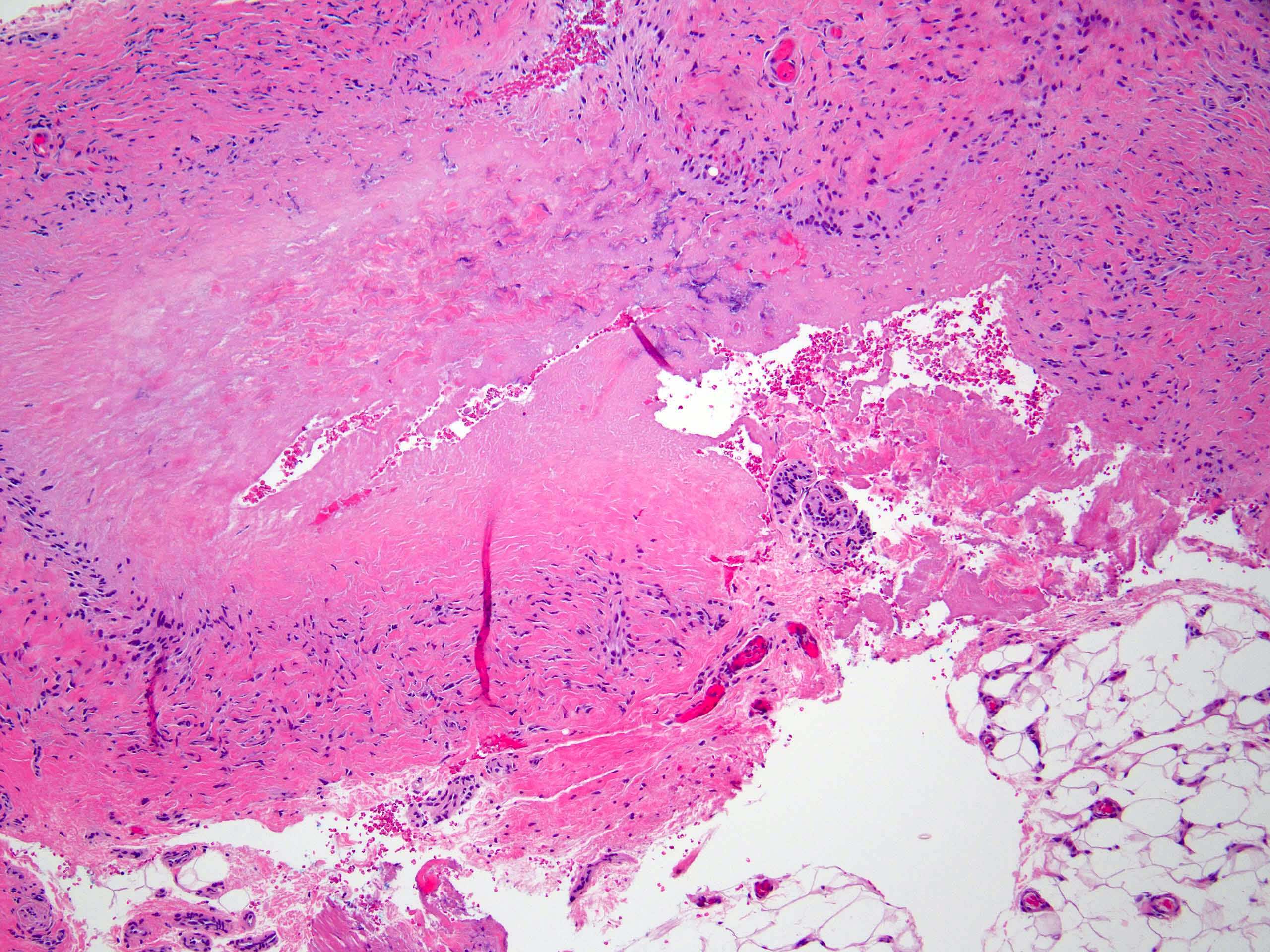
- Necrobiotic (collagenolytic) granulomas
- Granulomas characterized by central areas of degraded collagen surrounded by lymphocytes and histiocytes, occasionally palisaded, are present in dermis
- Occasional multinucleate giant cells
- Deep variants
- Subcutaneous
- May extend from deep dermis through subcutis to fascia and synovium (Clin Exp Dermatol 1991;16:218)
- Pseudorheumatoid nodule
- Nodules composed of palisaded granulomas with central eosinophilic material (degraded collagen) are separated by thickened collagen bundles
- Minimal or absent mucin
- Subcutaneous
- Interstitial (or incomplete)
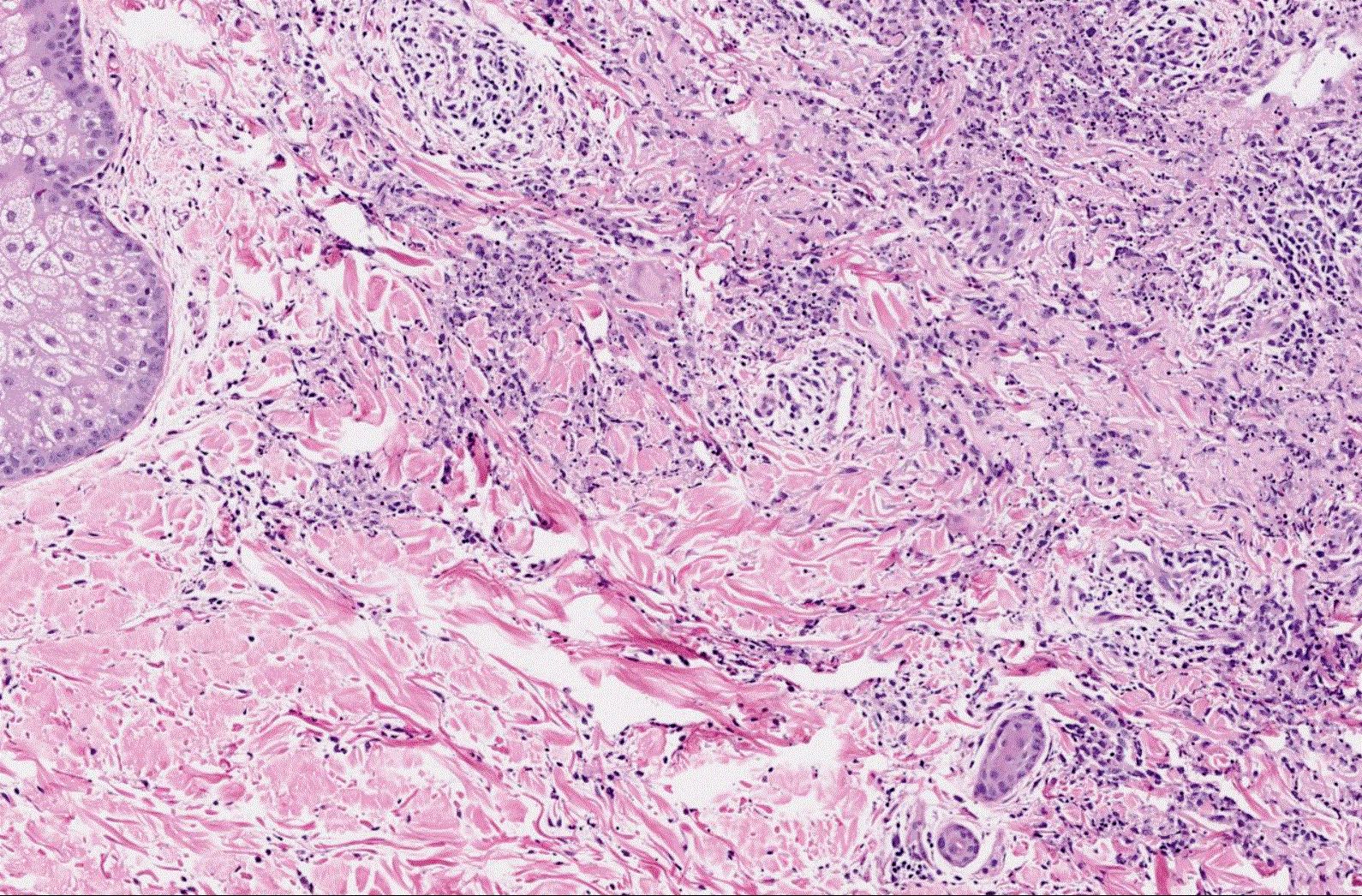
- Busy dermis (interstitial lymphohistiocytic inflammation)
- Histiocytes and lymphocytes arranged around vessels and intercalating between collagen bundles with conspicuous interstitial mucin
- Lacks necrobiosis
- Patch granuloma annulare more likely to be only or predominantly interstitial pattern (without palisaded granulomas) (J Cutan Pathol 2020;47:785)
- Nonnecrobiotic (sarcoidal or tuberculoid)
- Mimics sarcoidosis or tuberculous granulomas (Am J Dermatopathol 2015;37:547)
- Increased mucin or eosinophils may suggest granuloma annulare over mimics
- Eosinophils in ~40% of cases (J Cutan Pathol 1985;12:13)
- In generalized granuloma annulare, interstitial and palisading patterns roughly equal in frequency (Ann Dermatol 2009;21:113)
- Transepithelial excretion of altered collagen in perforating granuloma annulare
- Minimal epidermal changes
- Potential overlap with other granulomatous disorders
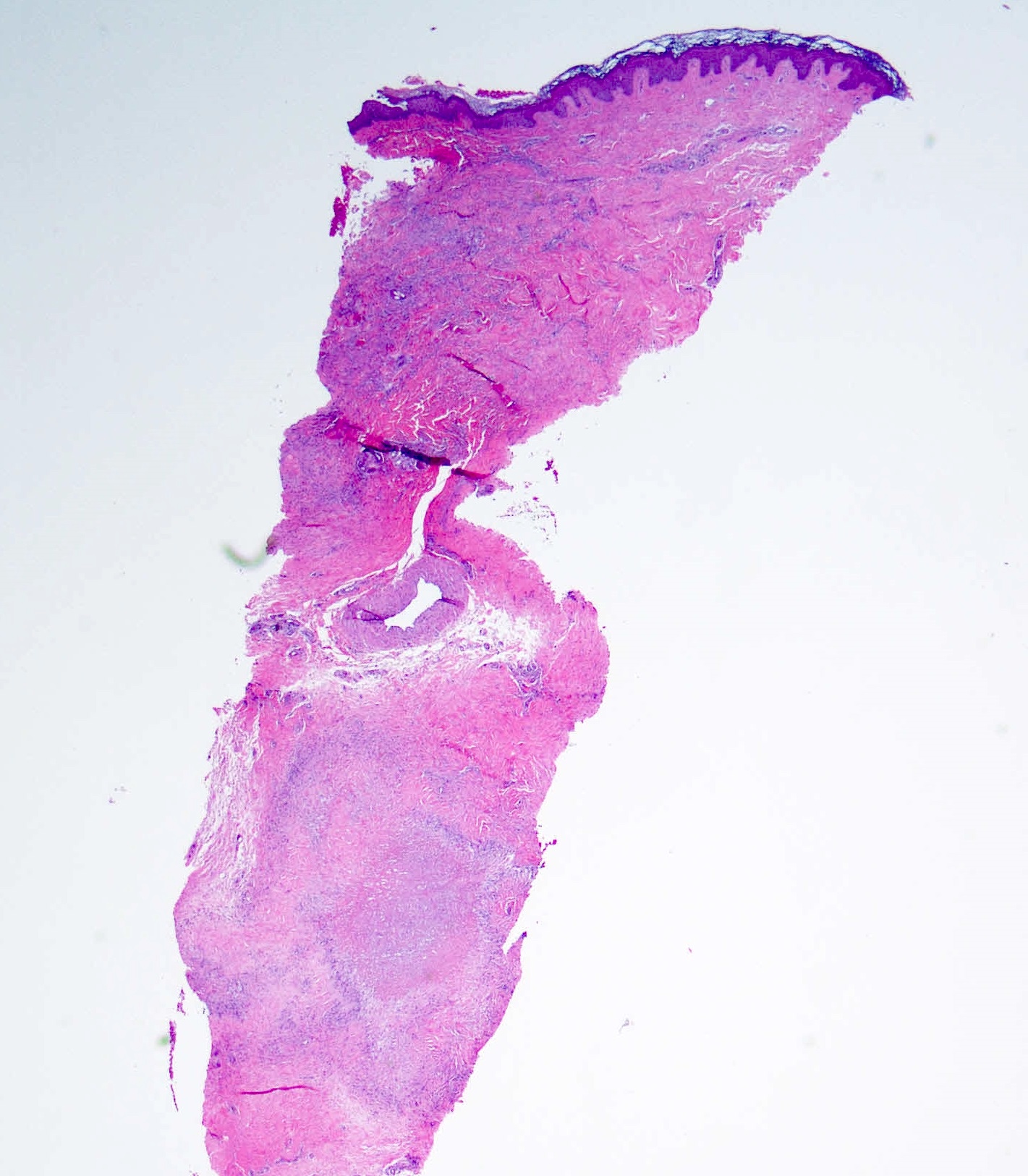
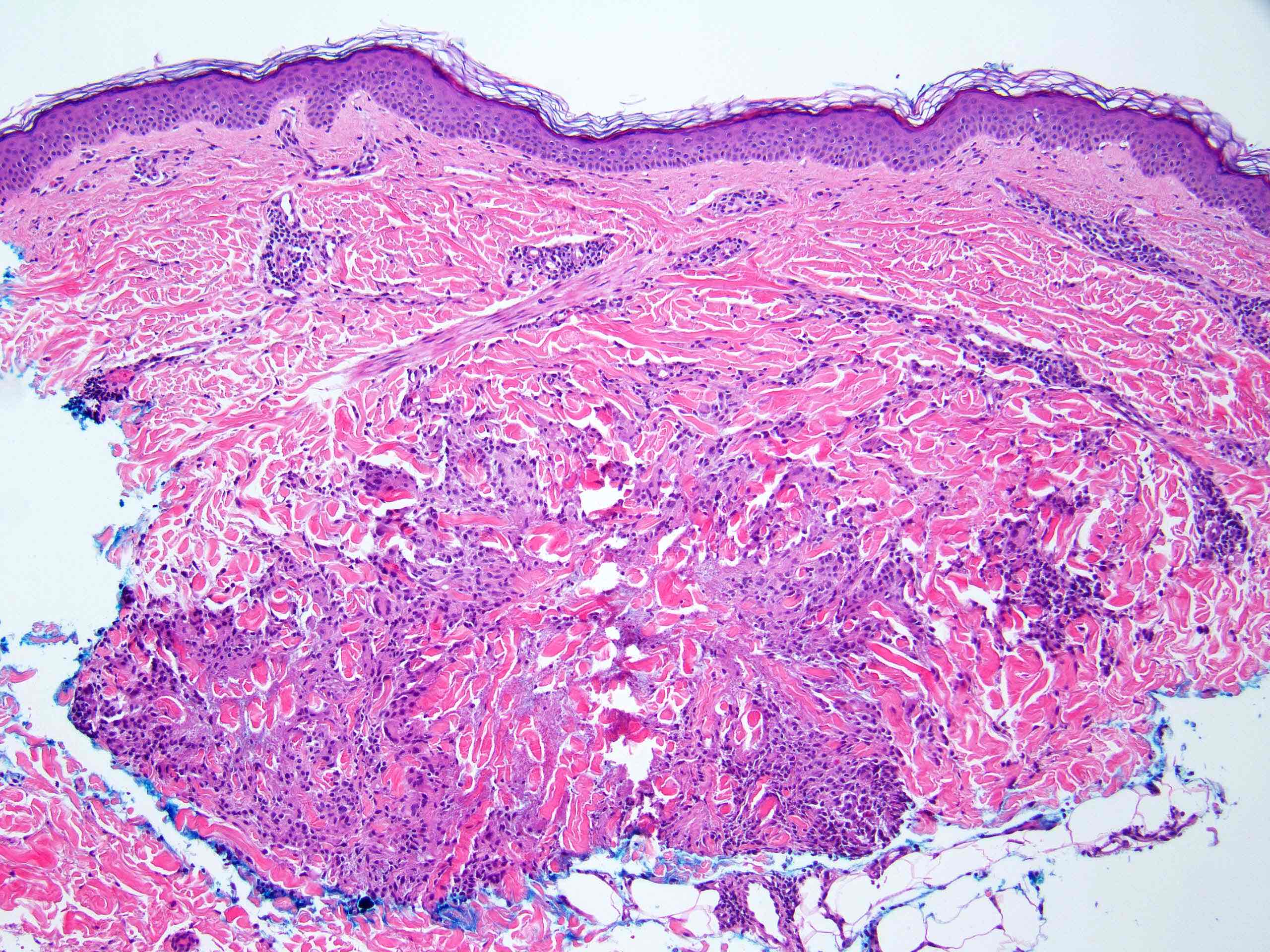
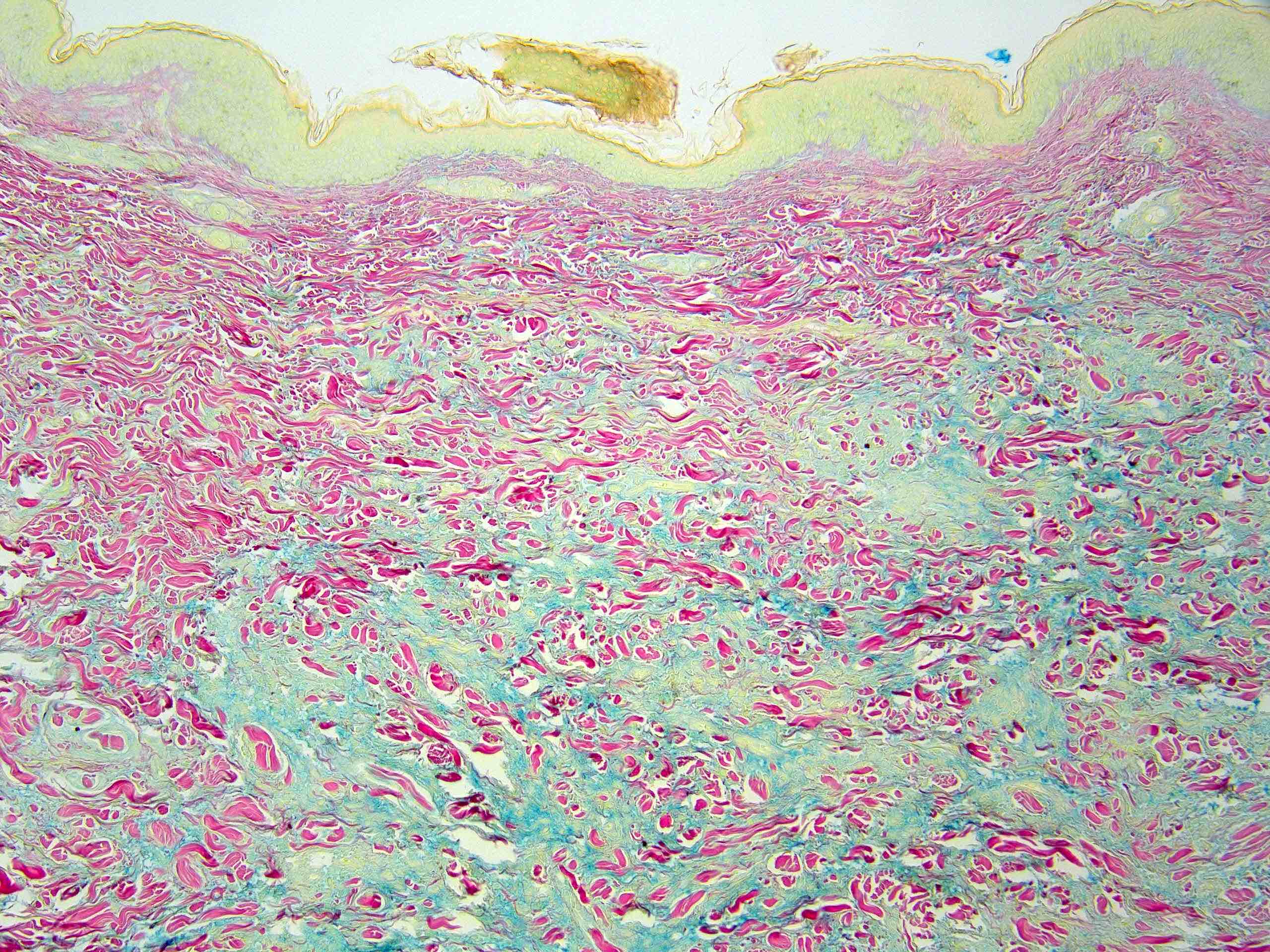
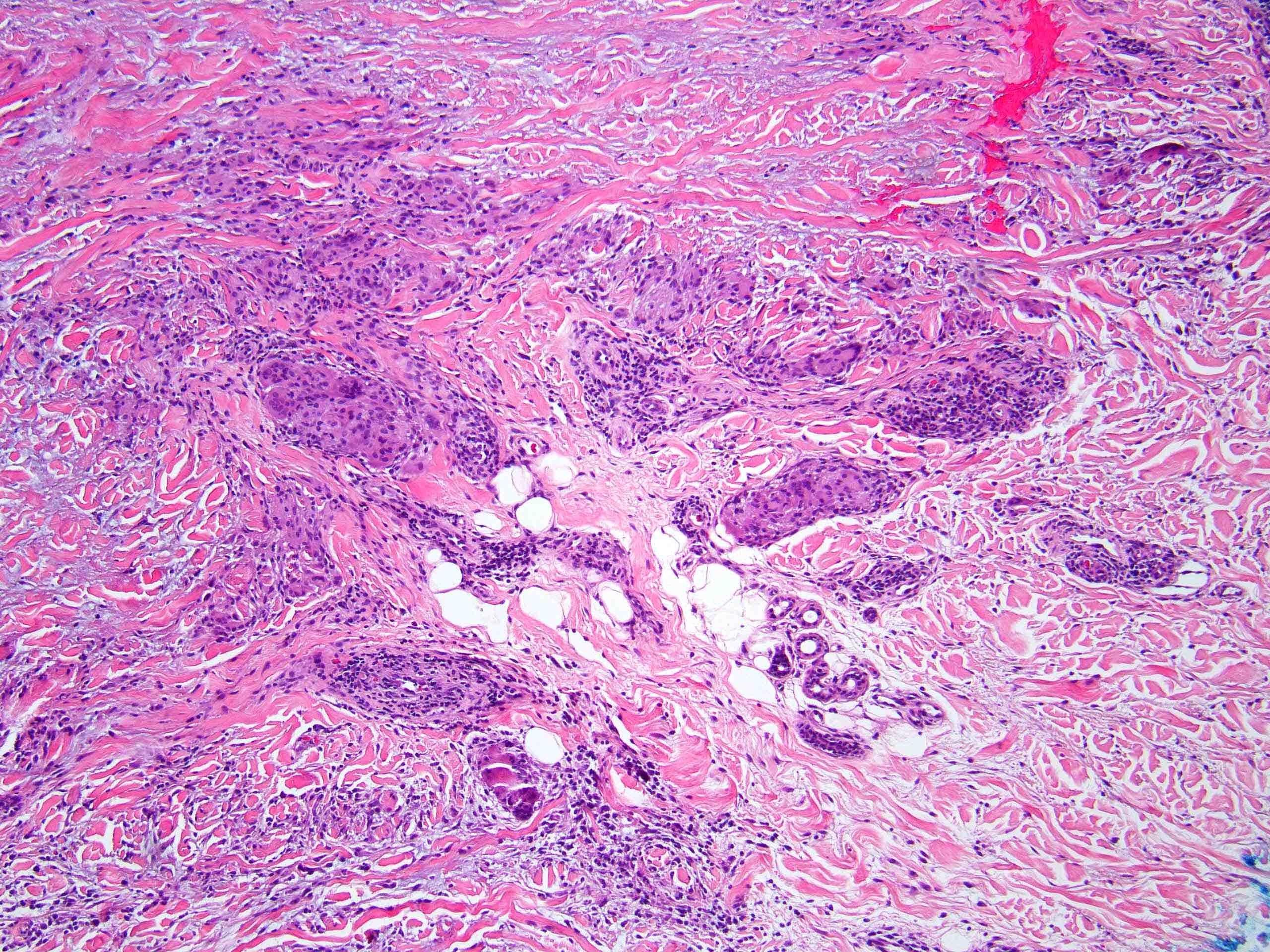
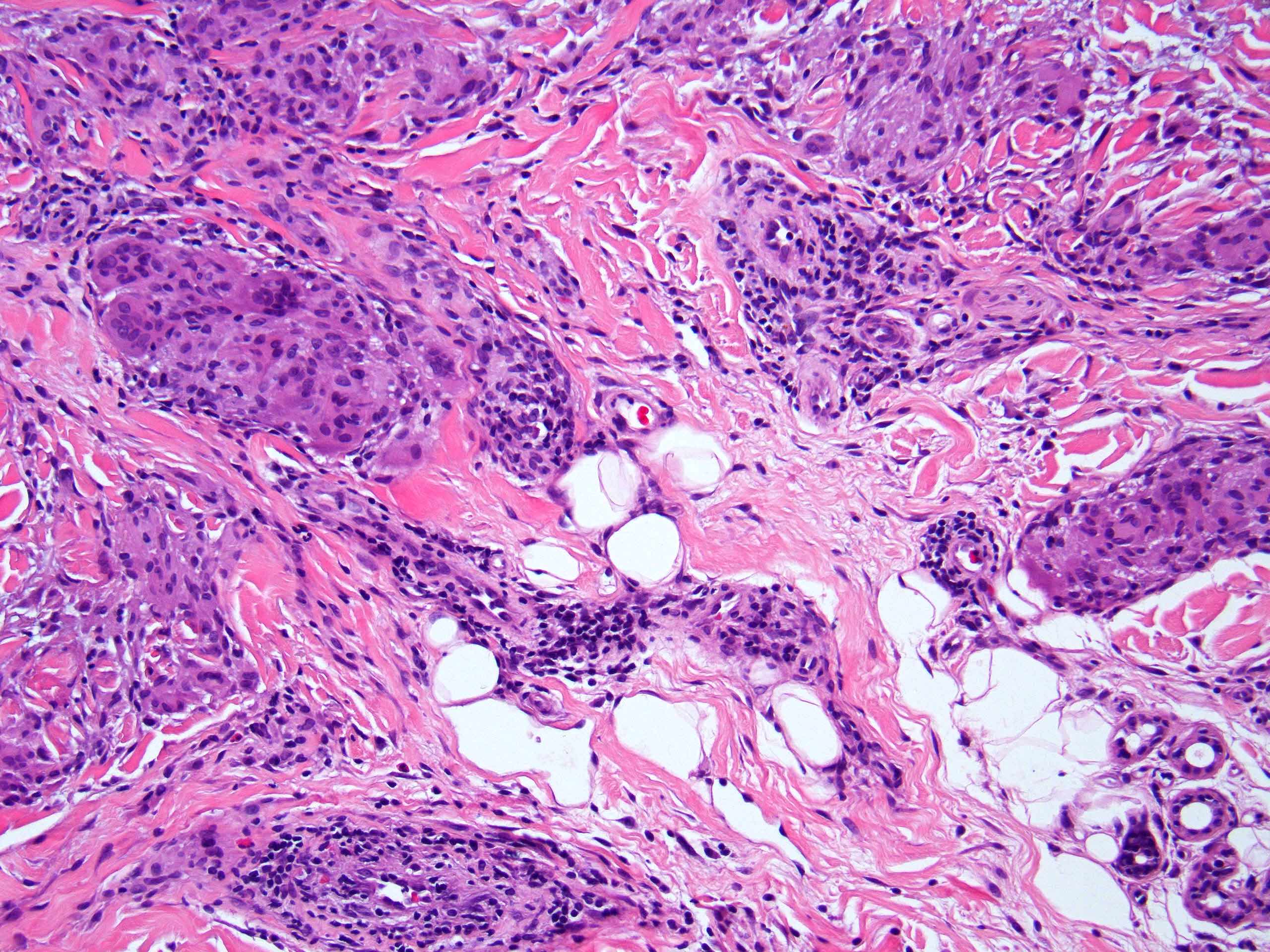
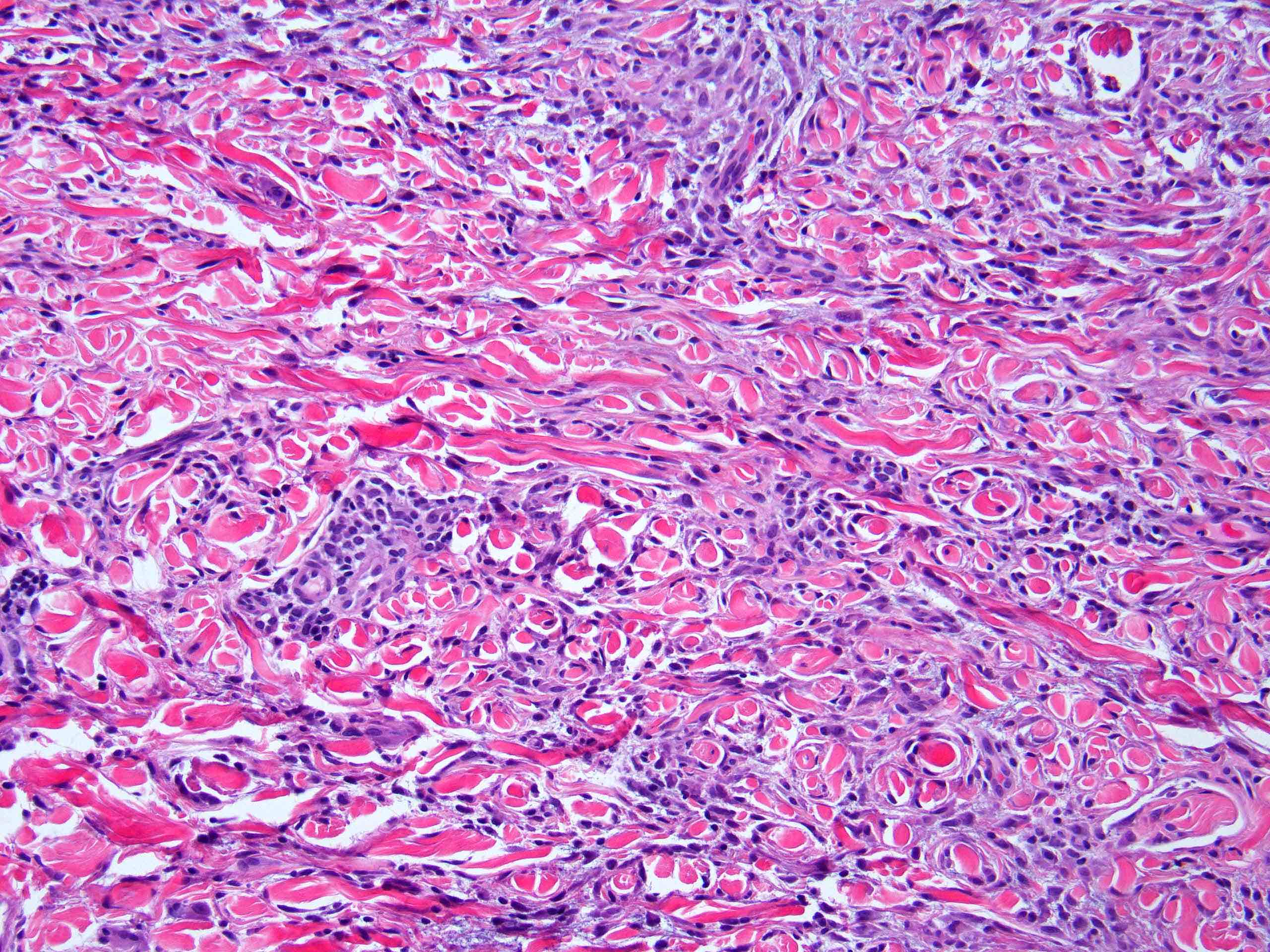
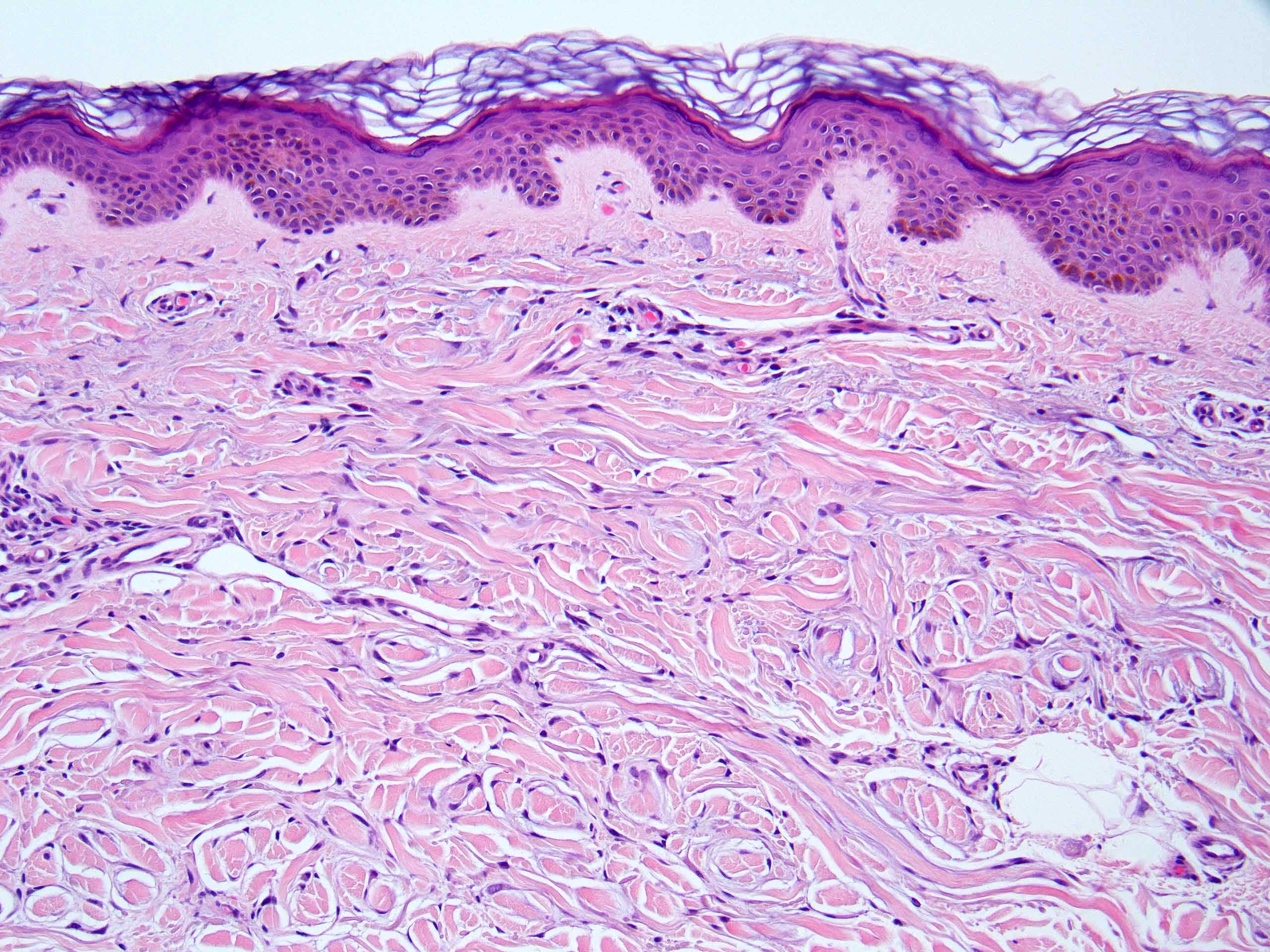
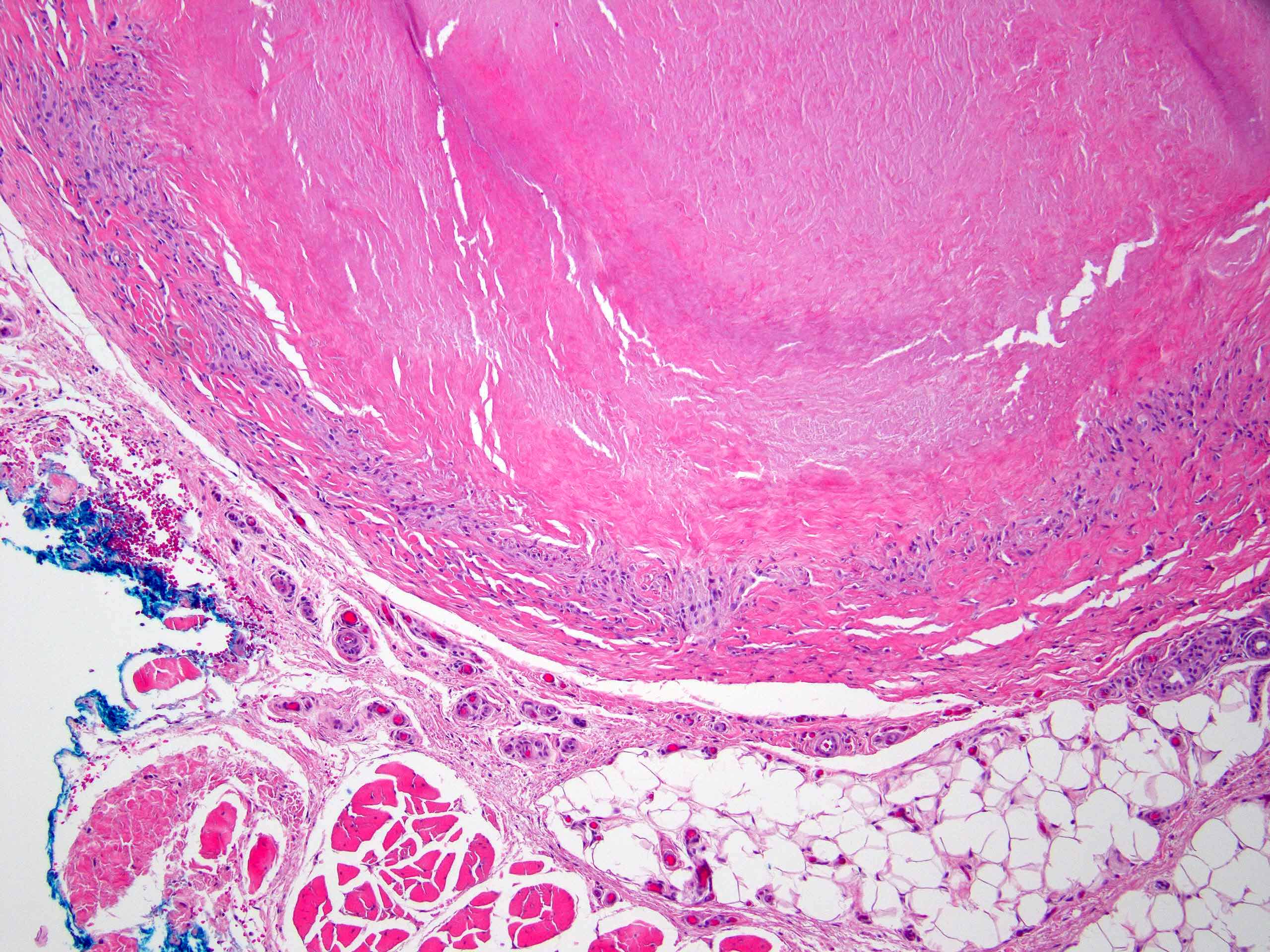
Microscopic (histologic) images
Contributed by Stephen Somach, M.D.
Virtual slides
Immunofluorescence description
- Fibrin in areas of collagen degradation (Br J Dermatol 1977;97:481)
Positive stains
- CD68 / PGM1
- May be more frequently positive in palisaded, rather than interstitial pattern (J Cutan Pathol 2019;46:471)
- CD163
- Alcian blue
- Colloidal iron
Electron microscopy description
- Cytoplasm of histiocytes contains dense cup-like structures in plasma membrane, pinocytic vacuoles, vesicular structures and large intracellular organelles (Arch Dermatol 1977;113:1681)
- Few secondary lysosomes within histiocytes (Arch Dermatol 1977;113:1681)
- Large amount of cytoplasmic vesicles and debris (Arch Dermatol 1977;113:1681)
- Granular material coating blood vessels (Arch Dermatol 1977;113:1681)
- Degenerating collagen and elastin (Arch Dermatol 1977;113:1681)
- Fibrin within areas of necrobiosis (Arch Dermatol 1977;113:1681)
Videos
Granuloma Annulare
Dr. James Carton
Sample pathology report
- Skin, left forearm, punch biopsy:
- Consistent with granuloma annulare (see comment)
- Comment: Sections show a punch biopsy specimen with a normal epidermis. Within the reticular dermis is a palisaded array of histiocytes associated with central collagen degeneration and mucin deposition.
Differential diagnosis
- Annular elastolytic giant cell granuloma (actinic granuloma):
- May be variant of granuloma annulare (Am J Dermatopathol 1979;1:43)
- Mucin often absent (Cutis 1998;62:181)
- Elastophagocytosis may be seen in both granuloma annulare and annular elastolytic giant cell granuloma (J Am Acad Dermatol 1986;14:975)
- Central atrophy can occasionally be noted
- Minimal or absent necrobiosis
- Interstitial granulomatous dermatitis (with arthritis):
- Histologically (and often clinically) similar to interstitial form of granuloma annulare
- Interstitial histiocytic infiltrate with variable degeneration of collagen and elastin
- May be more diffuse (Br J Dermatol 2012;166:775)
- Mucin infrequently observed
- Clusters of histiocytes rimming collagen (floating sign) (Br J Dermatol 2012;166:775)
- Interstitial granulomatous dermatitis may be best differentiated from granuloma annulare based on clinical context
- Interstitial granulomatous dermatitis usually reported in association with autoimmune disease (especially rheumatoid arthritis) / autoantibodies (especially anti-DNA antibodies) or as an adverse drug reaction (most commonly calcium channel blockers, statins) (J Am Acad Dermatol 2001;45:286, Dermatol Clin 2015;33:373)
- When reported in association with drug, may be termed interstitial granulomatous drug reaction (IGDR)
- Interstitial granulomatous drug reaction may have an accompanying interface dermatitis and has been reported as having pseudolymphomatous features (J Cutan Pathol 1998;25:72, Am J Dermatopathol 2001;23:295)
- Eosinophils may be seen in both connective tissue disease related interstitial granulomatous disease and IGDR (Am J Case Rep 2014;15:94, Am J Dermatopathol 2010;32:408)
- Overlap with drug induced granuloma annulare and IGDR (JAAD Case Rep 2018;4:152)
- Histologically (and often clinically) similar to interstitial form of granuloma annulare
- Necrobiosis lipoidica (J Dtsch Dermatol Ges 2015;13:211):
- Layer cake appearance
- Minimal mucin
- Involves the entire dermis and extends into subcutis, often producing a septal panniculitis
- Plasma cells, giant cells
- Rheumatoid nodule (J Dtsch Dermatol Ges 2015;13:211):
- Histologically very similar to pseudorheumatoid nodule variant of deep granuloma annulare
- Palisaded histiocytes with fibrinoid necrosis
- Mucin typically sparse or absent
- Typically subcutis rather than dermal (versus deep granuloma annulare)
- Palisaded neutrophilic granulomatous dermatitis (G Ital Dermatol Venereol 2018;153:243):
- Prominent neutrophils and frequent leukocytoclasis
- Deep basophilic degeneration
- Associated with connective tissue disease, rheumatoid arthritis and lymphoproliferative disease
- Acne agminata (Skinmed 2005;4:234):
- Ruptured folliculosebaceous units
- Tuberculoid granulomas with caseous (coagulative) necrosis
- Perifollicular fibrosis
Additional references
Board review style question #1
A 44 year old woman presents with an eruption involving her proximal upper extremities characterized by slightly erythematous papules coalescing into annular and arciform plaques. Which of the following systemic abnormalities is most strongly associated with granuloma annulare?
- Obesity
- Hematologic malignancy
- HIV
- Hyperlipidemia
- Intravenous drug abuse
Board review style answer #1
Board review style question #2
A 51 year old woman with diabetes presents with skin colored papules on her chest and abdomen that have a vague annular configuration. A 4 mm punch biopsy is taken from her abdomen. Sections demonstrate palisaded histiocytes forming granulomas with peripheral lymphocytes and central eosinophilic material. Which interstitial extracellular substance would you expect to be most prevalent in this granulomatous dermatosis?
- Calcium
- Mucin
- Urate crystals
- Lipid
- Amyloid
Board review style answer #2