Table of Contents
Definition / general | Essential features | Terminology | ICD coding | Epidemiology | Pathophysiology | Etiology | Diagrams / tables | Clinical features | Diagnosis | Laboratory | Radiology description | Prognostic factors | Case reports | Treatment | Gross description | Microscopic (histologic) description | Microscopic (histologic) images | Cytology description | Cytology images | Positive stains | Negative stains | Molecular / cytogenetics description | Sample pathology report | Differential diagnosis | Additional references | Board review style question #1 | Board review style answer #1 | Board review style question #2 | Board review style answer #2Cite this page: Yeh YA. Schistosomiasis (bilharziasis). PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/bladderschistosomiasis.html. Accessed April 3rd, 2025.
Definition / general
- Parasitic infection of the bladder with blood flukes (trematodes), Schistosoma species (mainly Schistosoma haematobium)
Essential features
- Bladder schistosomiasis is most commonly caused by Schistosoma haematobium
- Eggs of Schistosoma haematobium: 110 - 170 μm, oval with terminal spine
- Eggs of Schistosoma mansoni: 115 - 175 μm, oval with lateral spine
- Few case reports of bladder schistosomiasis caused by Schistosoma mansoni and Schistosoma haematobium - Schistosoma mansoni hybrid (Emerg Infect Dis 2019;25:365)
- Coinfection with Schistosoma haematobium and Schistosoma mansoni occurs (East Afr Med J 2013;90:36)
Terminology
- Bladder bilharziasis is named after Theodor Bilharz, a German physician who discovered the first blood fluke causing urinary schistosomiasis in 1851 (Wikipedia: Schistosomiasis [Accessed 9 February 2022])
- Bladder schistosomiasis
- Genitourinary schistosomiasis
- Schistosomiasis related cystitis
ICD coding
- ICD-10: B65.0 - schistosomiasis due to Schistosoma haematobium [urinary schistosomiasis]
Epidemiology
- Endemic in Africa and the Middle East (Nat Rev Dis Primers 2018;4:13)
- Transmission in the Nile River valley in Egypt and Mahgreb area in North Africa
- Recent focus of infection in Corsica, France (Trends Parasitol 2017;33:600)
Pathophysiology
- After penetration of skin or mucous membranes, schistosomulae migrate through the lungs to portal venous system and mature into adults
- About 6 weeks later, adult worms migrate to bladder venules (Nat Rev Dis Primers 2018;4:13)
- Females lay eggs that reach the bladder wall, penetrate bladder mucosa and excrete into urine
- Bladder wall shows eggs and mixed inflammatory reaction with lymphocytic, neutrophilic and eosinophilic infiltrate and scarring of the vesicular vessels
- Parasitic eggs provoke chronic granulomatous inflammation with calcifications and fibrotic thickening of the bladder wall, deposits of calcified eggs in later stage (Nat Rev Dis Primers 2018;4:13)
- Eggs may block drainage of urine into the bladder, causing hydroureter
- May develop secondary bacterial urinary tract infections, renal failure and pulmonary hypertension (Hum Pathol 1986;17:333)
- May progress to bladder cancer (squamous cell carcinoma [80 - 85%], adenocarcinoma [5 - 15%] and rarely urothelial carcinoma) (Front Med (Lausanne) 2018;5:223)
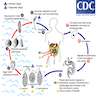
Etiology
- Humans are infected with schistosomes after exposure to cercariae released by snails (Bulinus species) in fresh water
- Penetration of skin or mucous membranes by cercariae (survives 3 - 4 days in fresh water)
- Schistomulae migrate to bladder plexus and nearby veins and venules (Nat Rev Dis Primers 2018;4:13)
- Female schistomulae deposit their eggs
- Some eggs reach the bladder wall, penetrate bladder mucosa and excrete in urine
- Eggs hatch and release miracidia
- Miracidia penetrate snail intermediate hosts (Bulinus species)
- After 2 generations of sporocysts, the snails produce cercariae and release them in fresh water (CDC: Parasites - Schistosomiasis [Accessed 9 February 2022])
Clinical features
- Swimmer's itch: cercarial dermatitis (days after infection)
- Local erythema, pruritic maculopapular rash
- Acute schistosomiasis (2 - 8 weeks after infection) (Lancet Infect Dis 2007;7:218)
- Katayama syndrome: fever ("snail fever"), cough, muscle pain, malaise, abdominal pain
- Hematuria, dysuria, suprapubic pain, urinary tract infections
- Chronic schistosomiasis (within months after infection)
- May progress to hydroureter, hydronephrosis, chronic kidney disease and bladder cancer (J Egypt Soc Parasitol 2017;47:211)
- May progress to bladder carcinoma, known as carcinogen (group 1) related to bladder cancer (Front Med (Lausanne) 2018;5:223)
Diagnosis
- Detection of Schistosoma haematobium or Schistosoma mansoni eggs in urine samples or bladder tissues (J Egypt Soc Parasitol 2017;47:211)
- Schistosoma haematobium eggs: 110 - 170 μm × 40 - 70 μm, oval with terminal spine (Hum Pathol 1986;17:333)
- Schistosoma mansoni eggs: 115 - 175 μm × 45 - 47 μm, oval with lateral spine
Laboratory
- Detection of Schistosoma specific antibody in serum or urine by enzyme linked immunosorbent assay (ELISA) (Parasitol Res 2011;108:1457)
- Detection of schistosome DNA or RNA by PCR (real time PCR or multiplex PCR) (Clin Microbiol Rev 2015;28:939)
Radiology description
- For bladder schistosomiasis: bladder wall thickening (usually > 4 mm) on ultrasound
- For carcinoma arising in bladder schistosomiasis: focal bladder wall thickening or mass on ultrasound
Prognostic factors
- Good prognosis for patients with early disease
- Prognosis is worse for chronic infections with complications:
- Immune complex glomerulonephritis
- Obstructive nephropathy
- Obstructive uropathy
- Chronic pyelonephritis
- Amyloidosis
- Bladder cancer (risk 1.72, further increased in smokers)
- References: J Adv Res 2013;4:453, Nat Rev Dis Primers 2018;4:13
Case reports
- 5 year old girl with Schistosoma haematobium in urine (Front Pediatr 2018;6:14)
- 14 year old boy with Schistosoma haematobium - Schistosoma mansoni hybrid parasite (Emerg Infect Dis 2019;25:365)
- 25 year old man with Schistosoma haematobium in bladder biopsy (BMC Clin Pathol 2018;18:13)
- 26 year old man with Schistosoma haematobium (Indian J Pathol Microbiol 2017;60:614)
- 67 year old man with bladder urothelial carcinoma and Schistosoma mansoni (Int J Surg Case Rep 2015;13:76)
Treatment
- Single course of praziquantel treatment can be curative
- Corticosteroids (severe disease), metrifonate (alternative therapy) for bladder schistosomiasis (ChemMedChem 2018;13:2374)
Gross description
- Early active stage: erythematous, sessile or pedunculated polyps, "grainy sandy" patches (Urology 2017;107:e7)
- Chronic stage: fibrotic thickening of bladder wall, stellate ulcers, tumor-like lesions (Hum Pathol 1986;17:333)
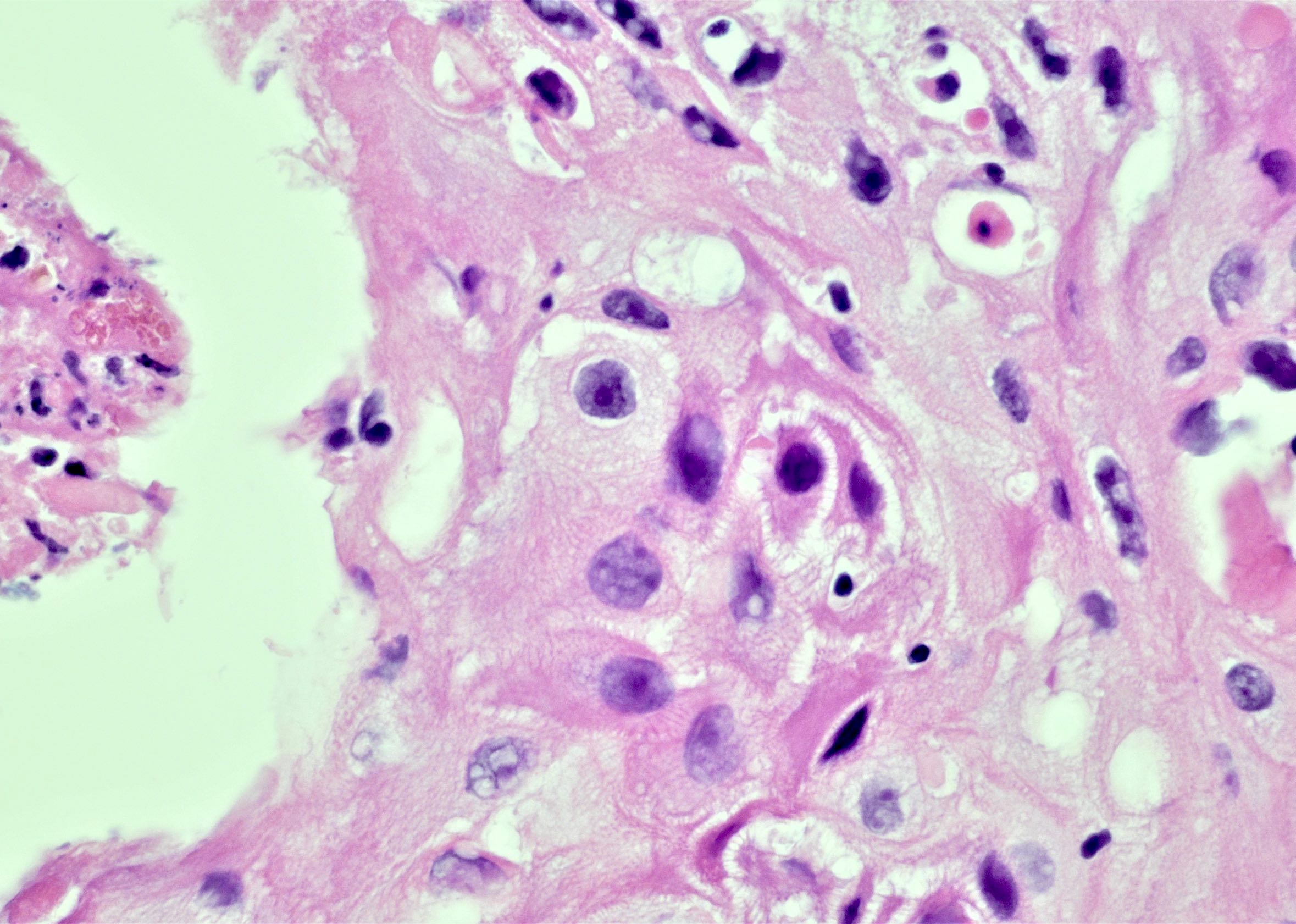
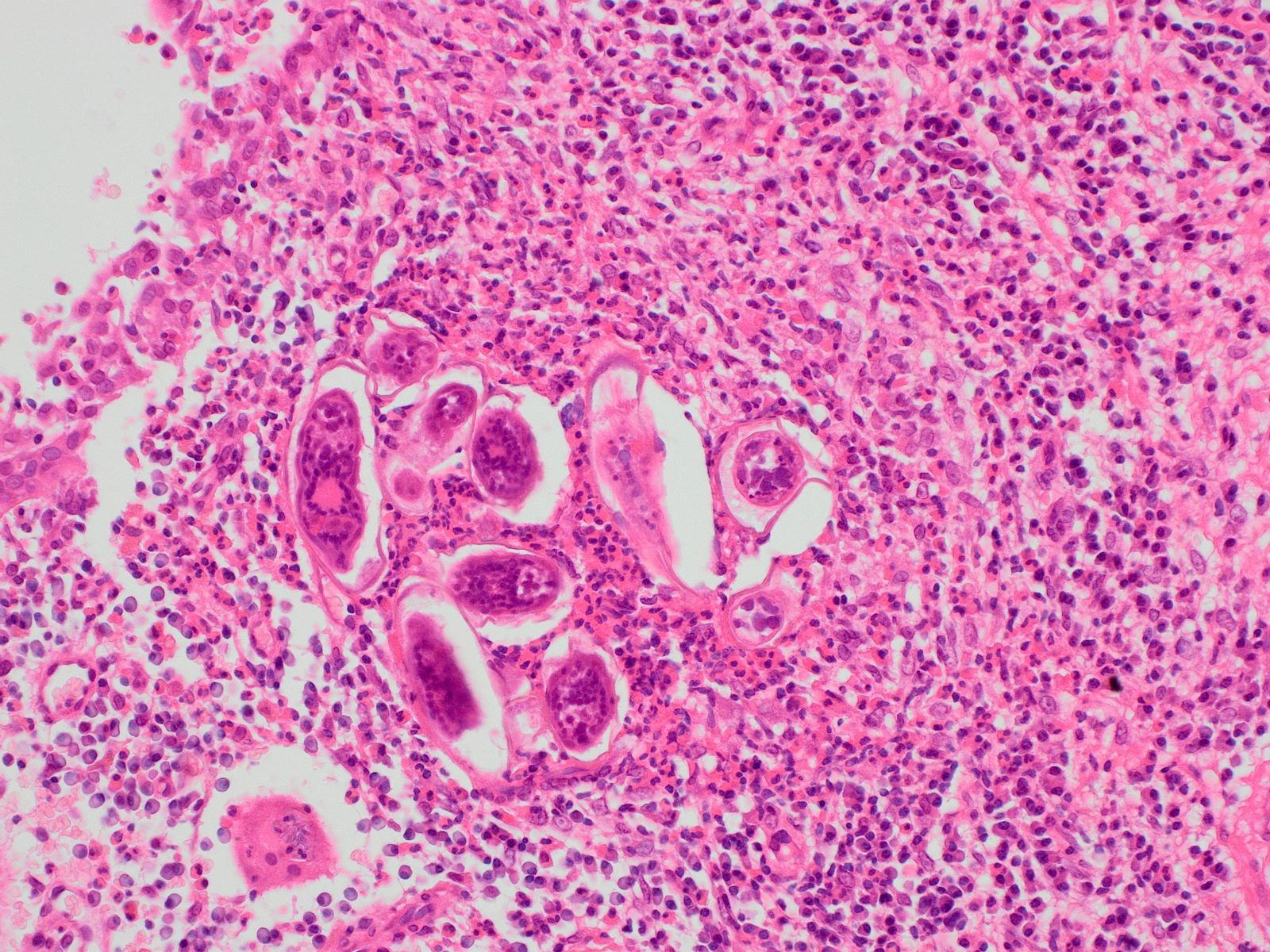
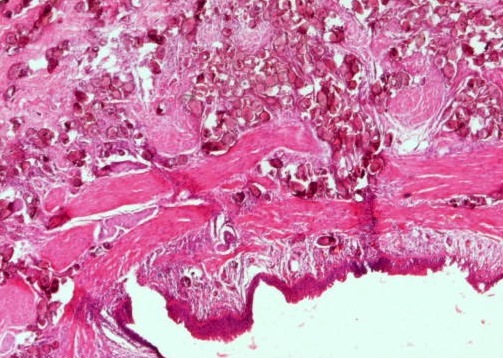
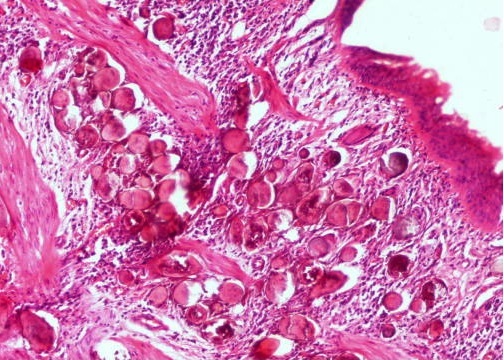
Microscopic (histologic) description
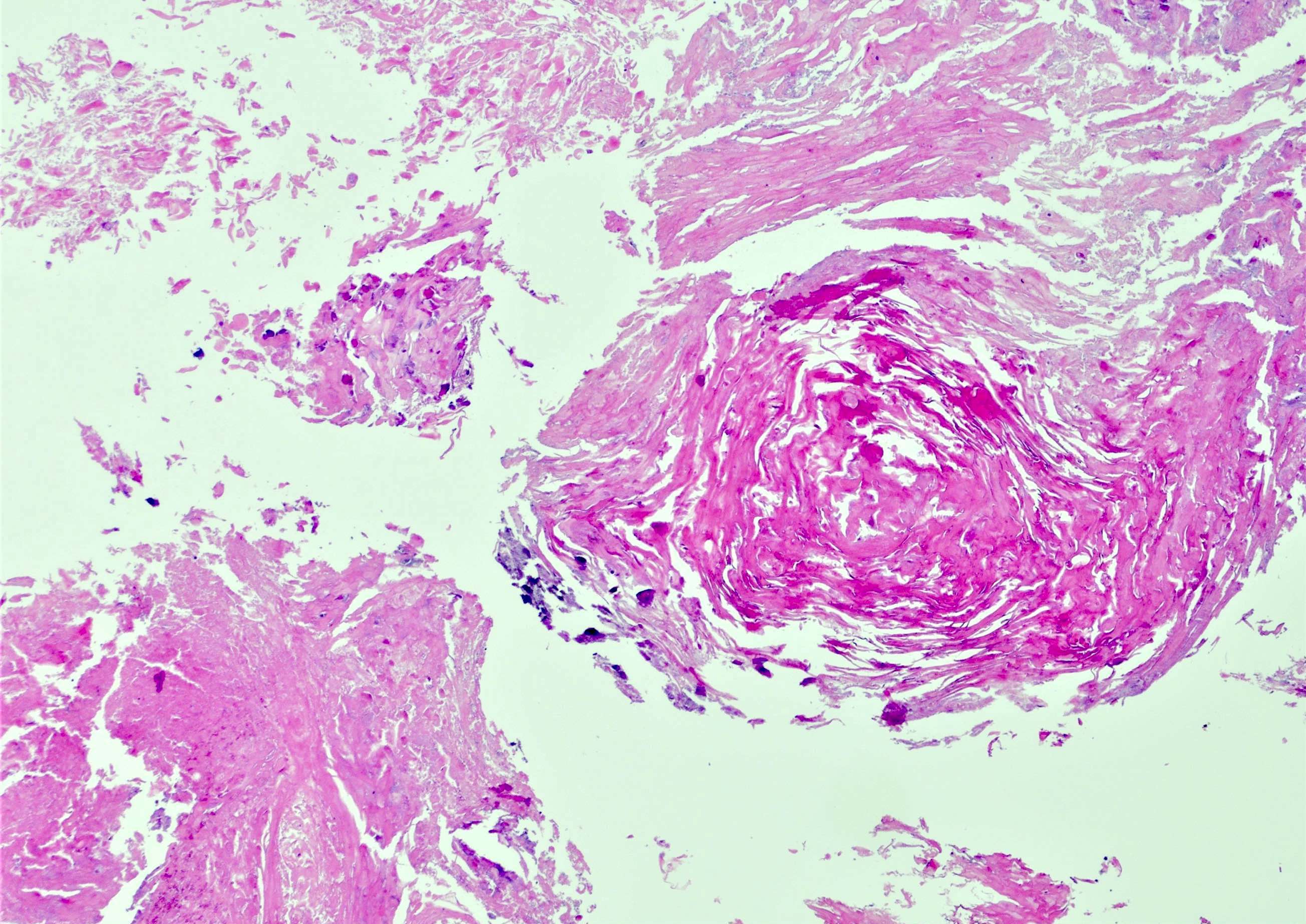
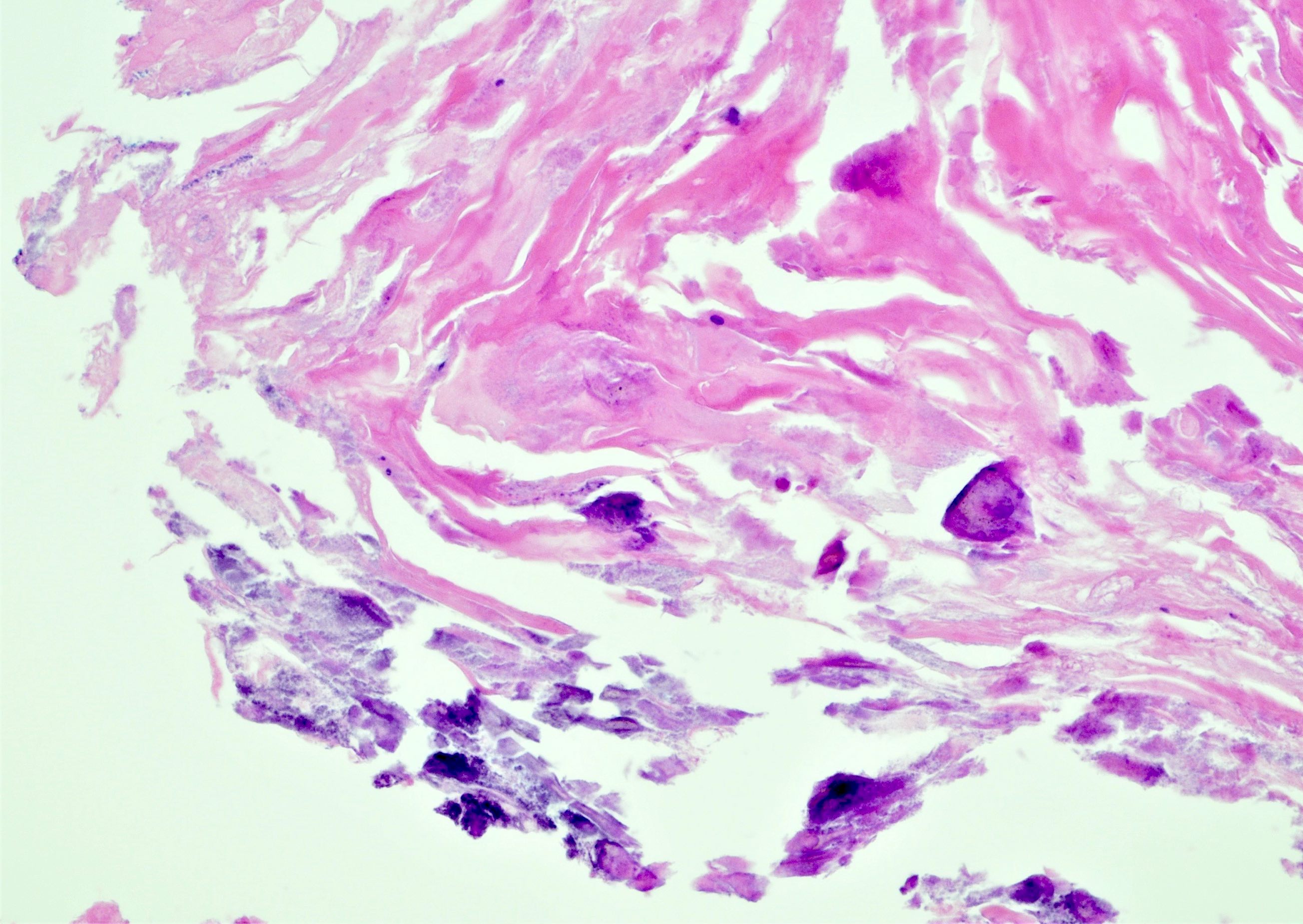
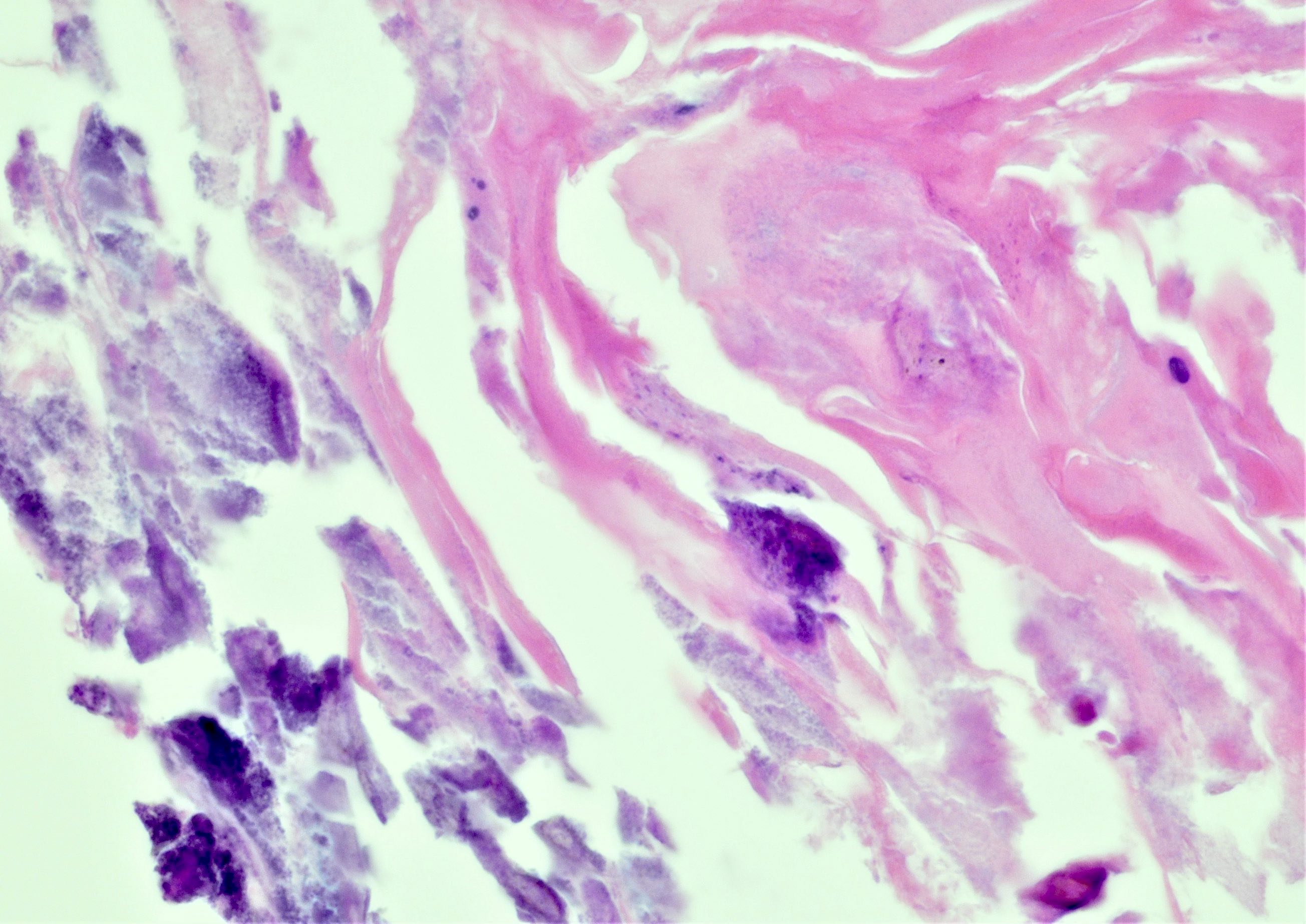
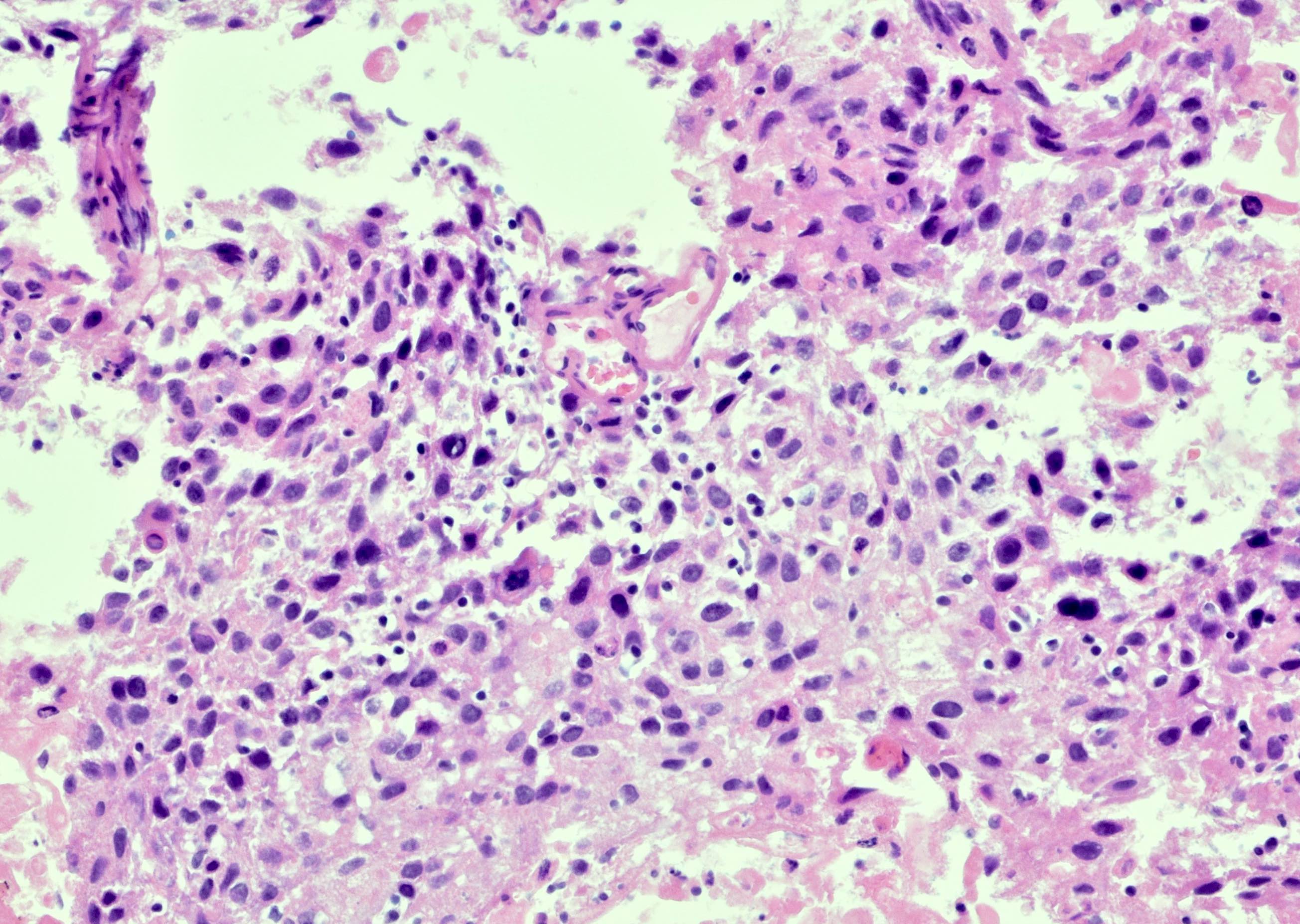
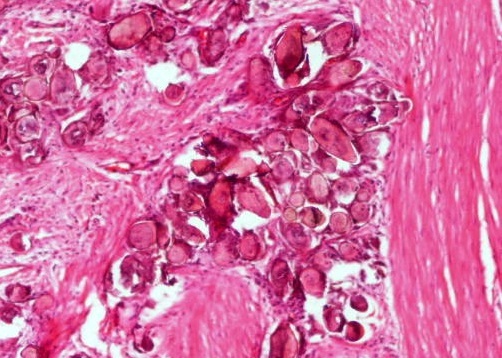
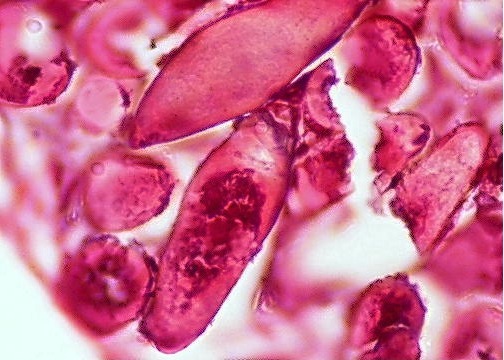
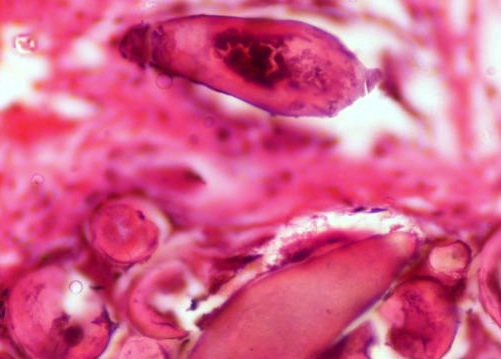
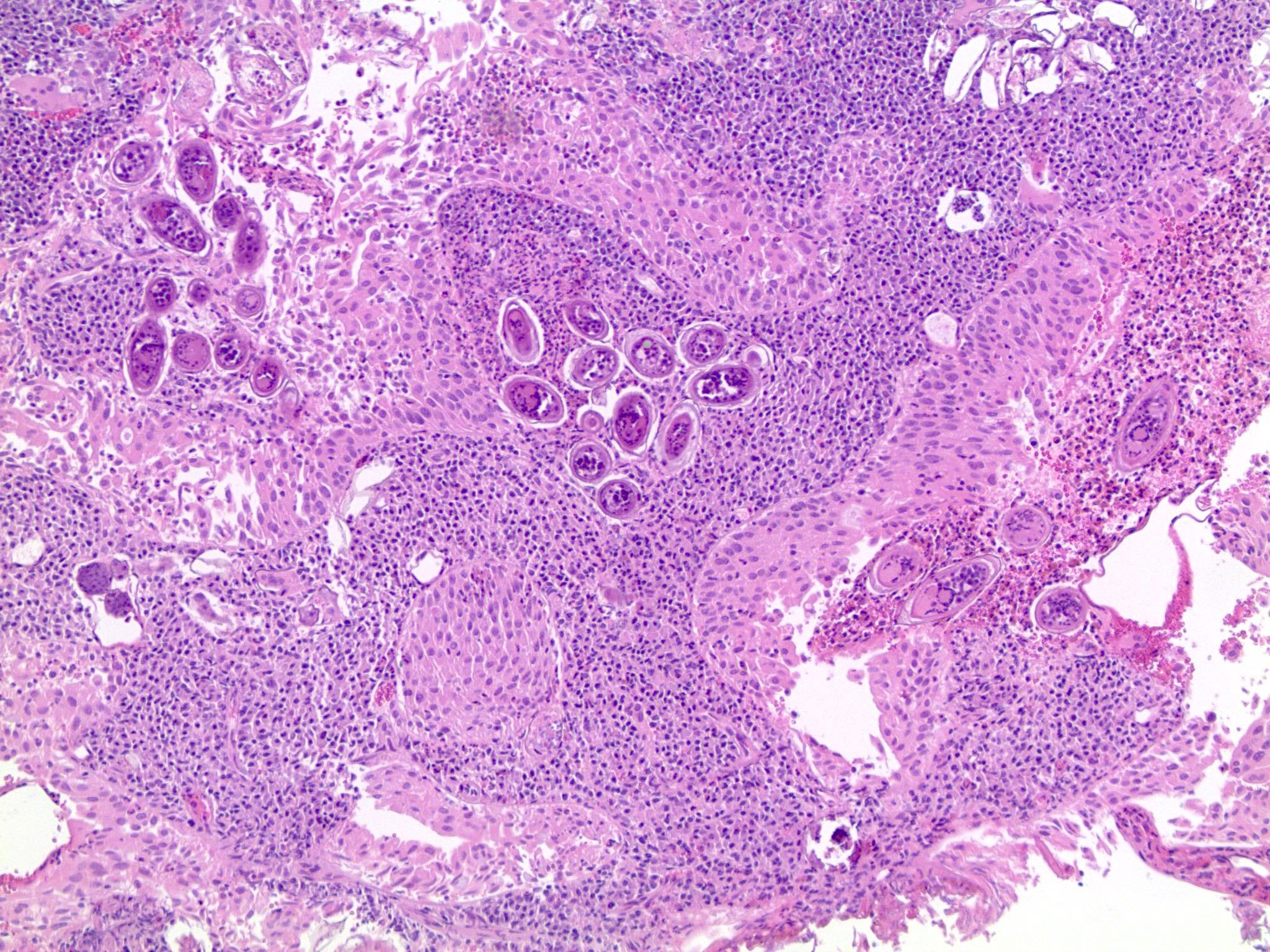
- Bladder mucosa with ulceration, necrosis and mixed inflammatory infiltrate of lymphocytes, neutrophils and eosinophils (Hum Pathol 1986;17:333)
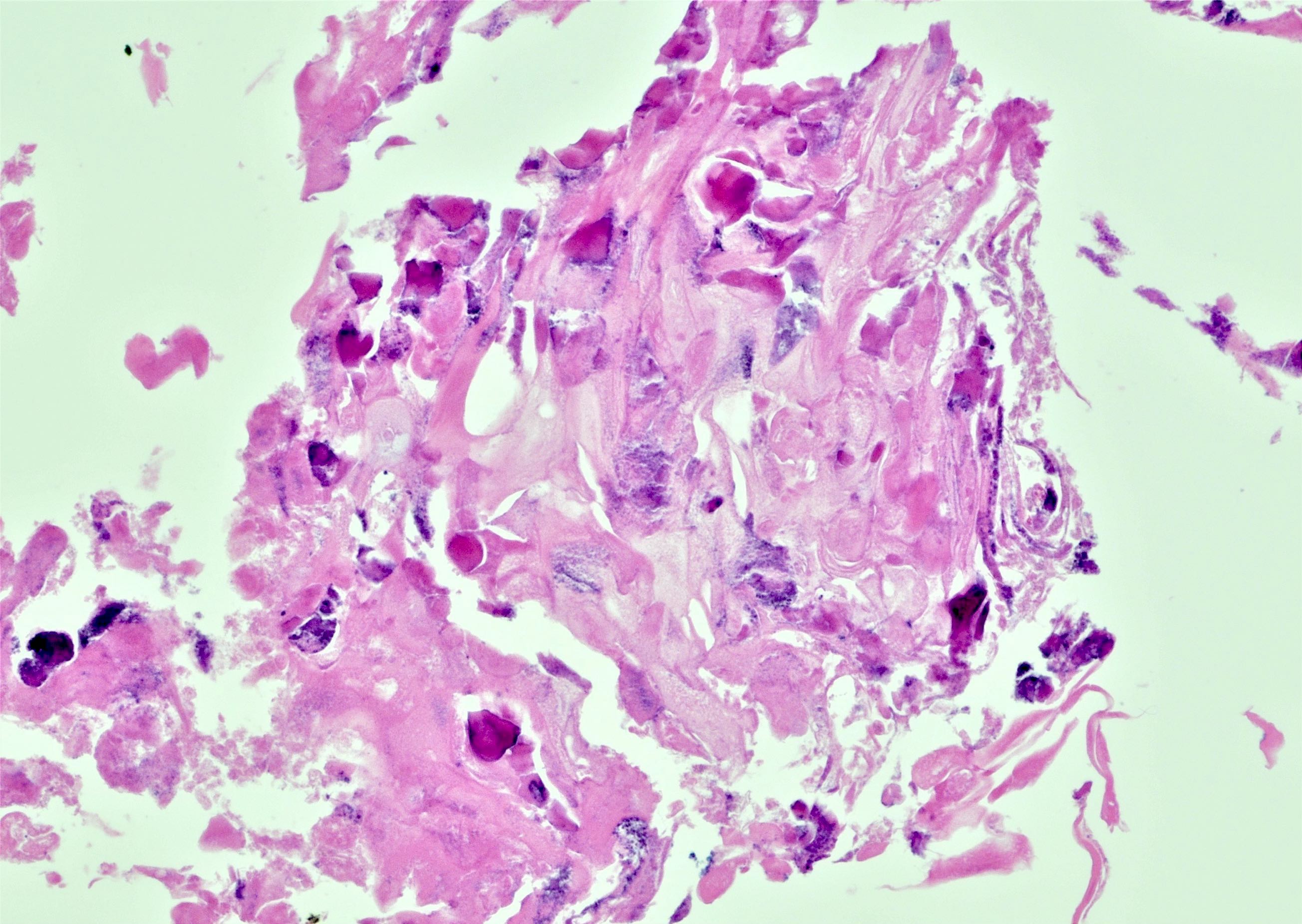
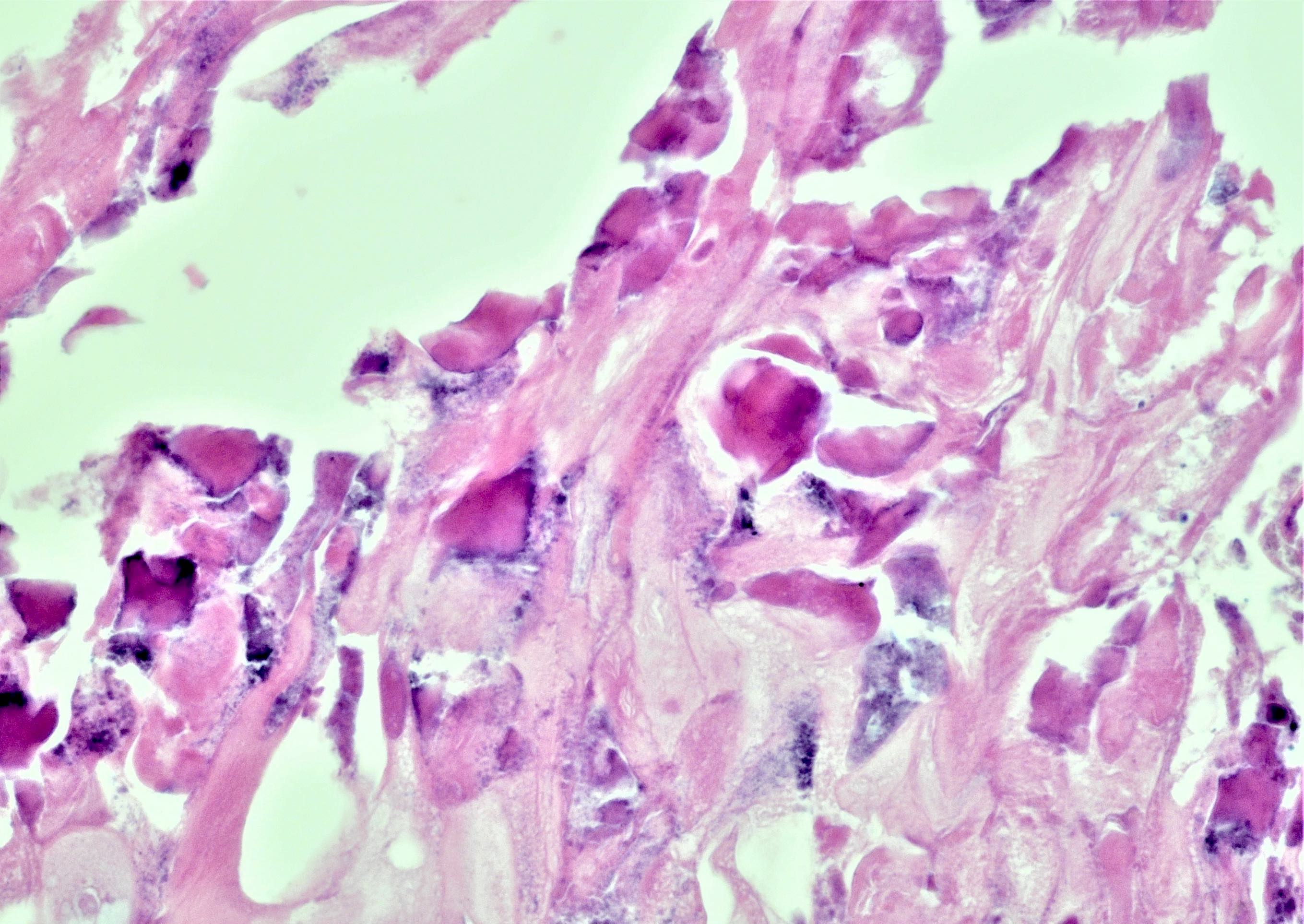
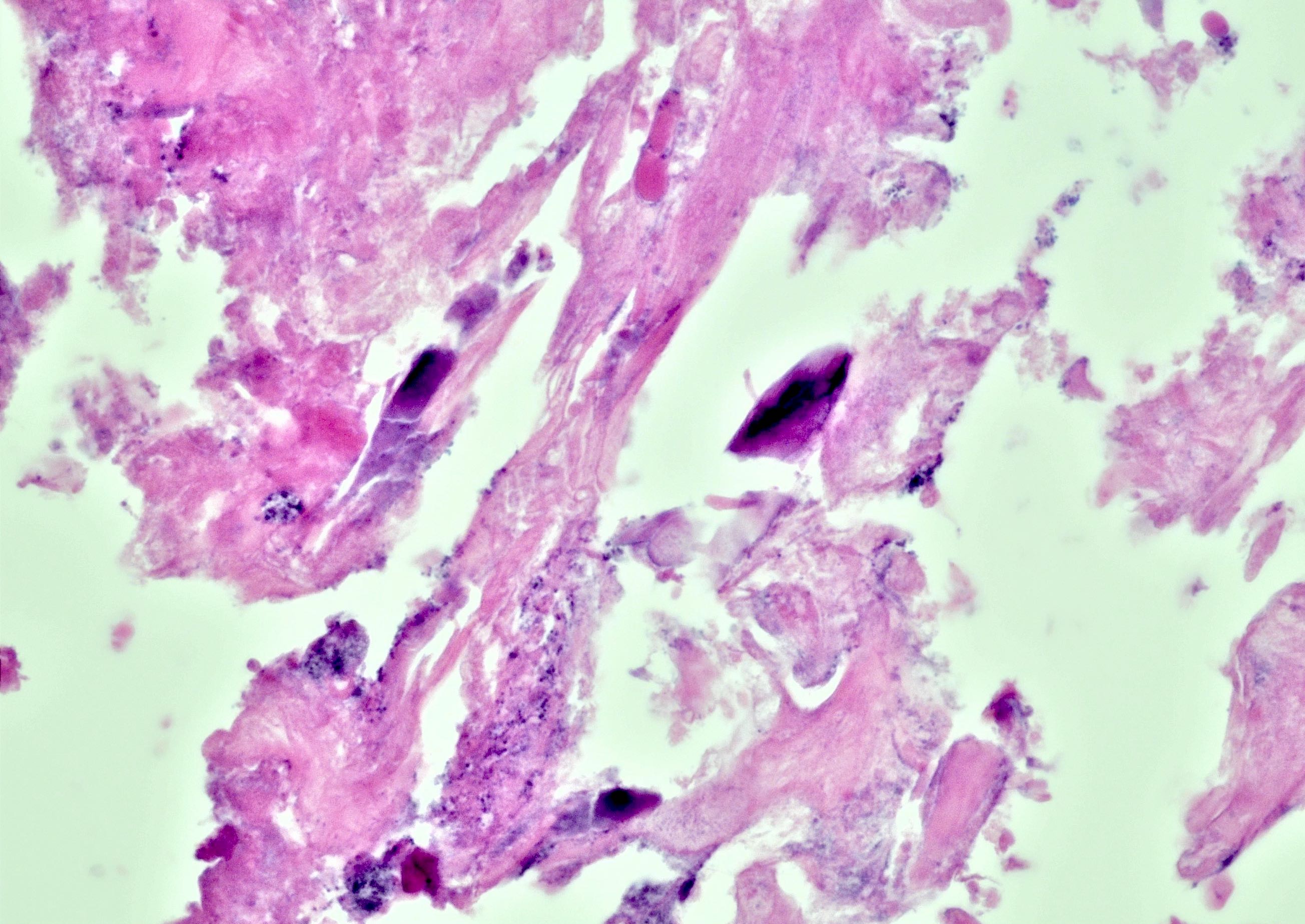
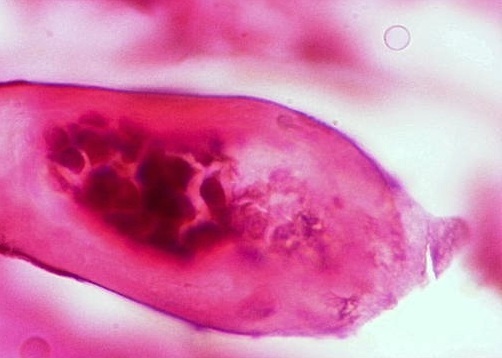
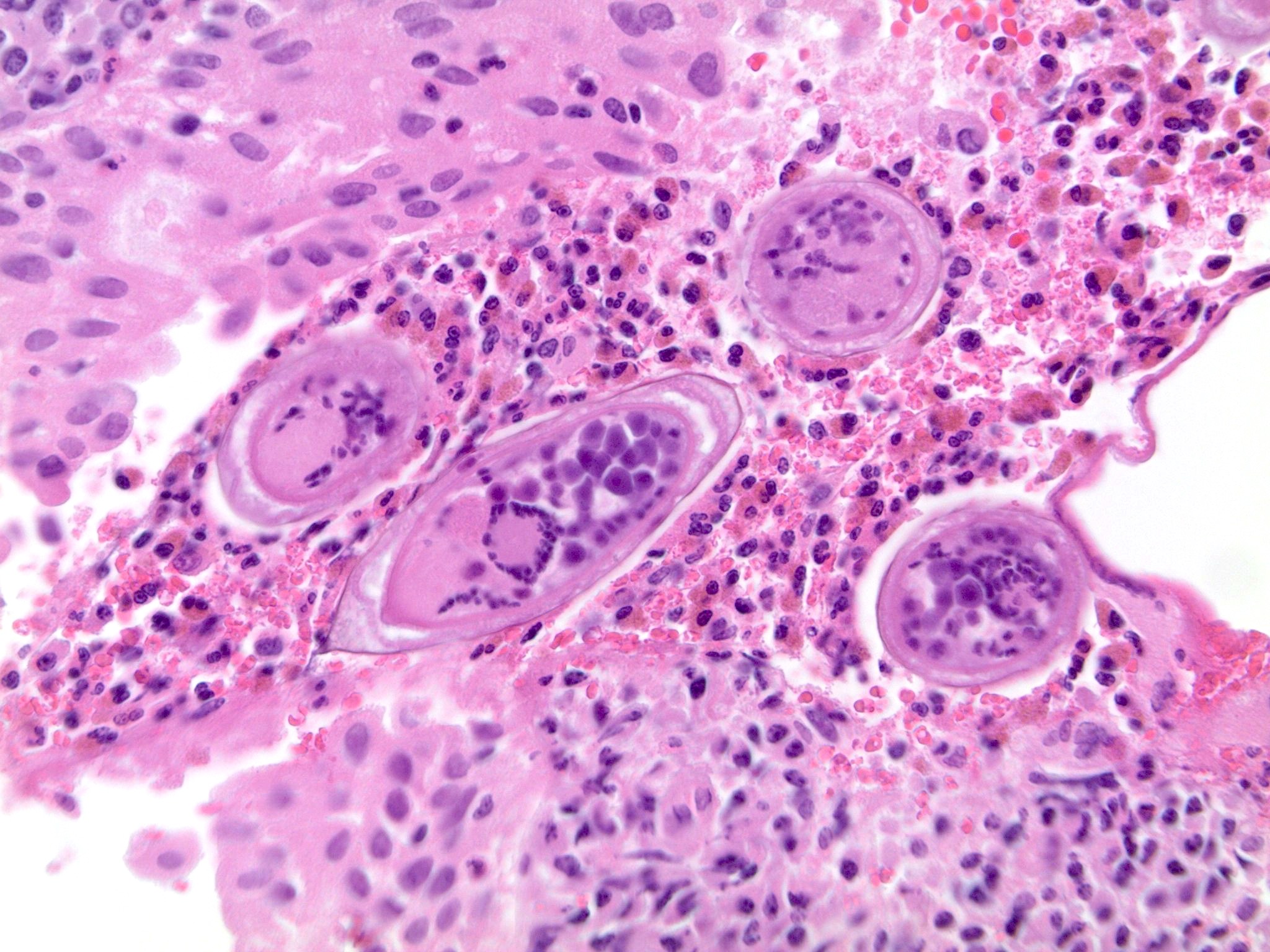
- Calcified eggs with chronic granulomatous inflammation detected in the bladder mucosa and muscularis (BMC Clin Pathol 2018;18:13)
- Calcified eggs measure approximately 120 - 170 μm with terminal spine (Schistosoma haematobium) or lateral spine (Schistosoma mansoni) (Clin Microbiol Rev 2015;28:939)
- Flattening of bladder mucosa with keratinizing squamous cell metaplasia or intestinal metaplasia (Hum Pathol 1986;17:333)
- Fibrosis with thickening of the bladder wall (Hum Pathol 1986;17:333)
- Infiltrating dysplastic squamous cells with keratinization present in schistosomiasis associated squamous cell carcinoma
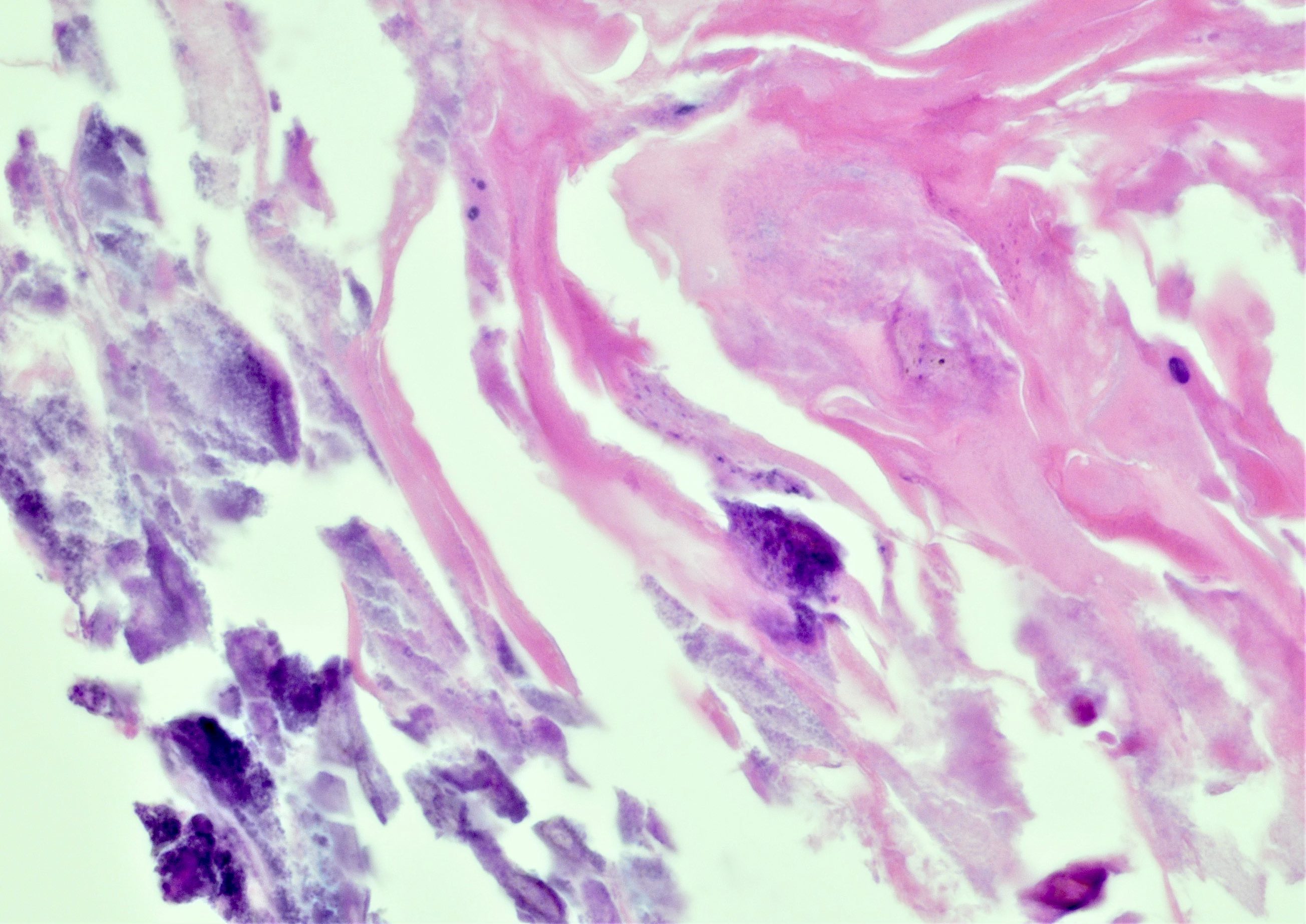
Microscopic (histologic) images
Contributed by Y. Albert Yeh, M.D., Ph.D., Susan Prendeville, M.D. and Kiran Alam, M.D., Anshu Jain, M.D.,
Veena Maheshwari, M.D., Farhan A. Siddiqui, M.B.B.S., Ershadul Haq, M.B.B.S., M.D. and @ThatGlassTho on Twitter
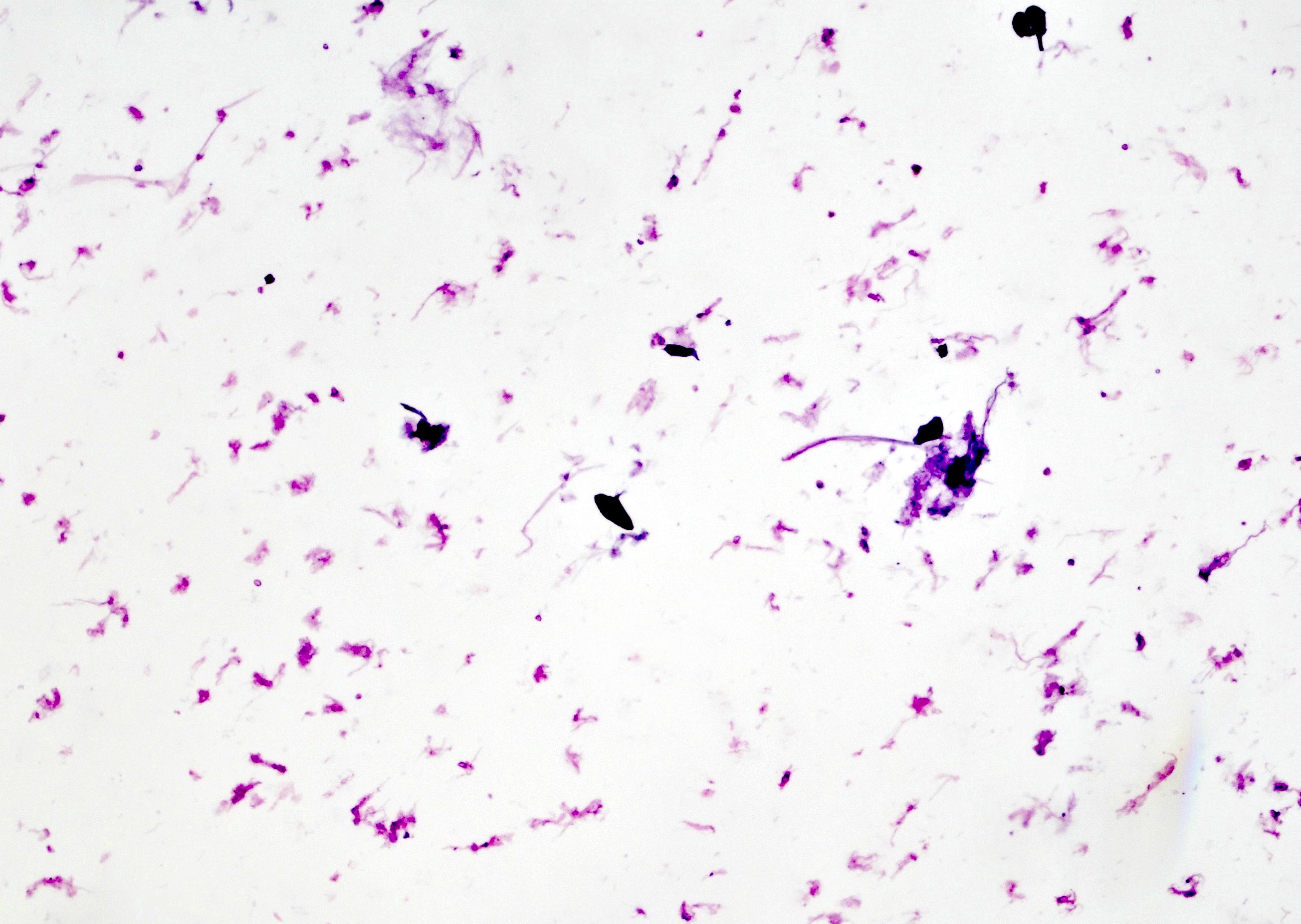
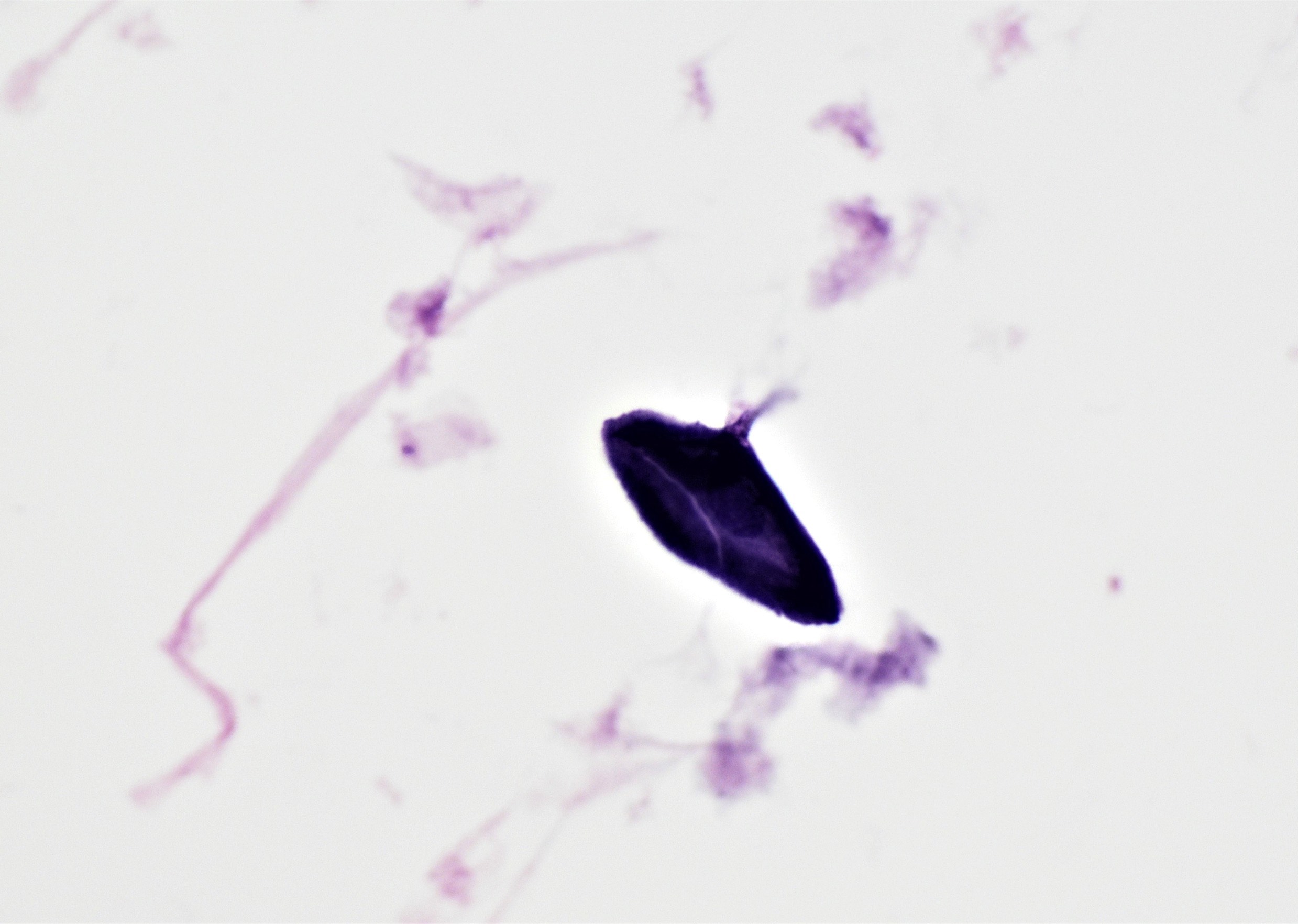
Cytology description
- Uncommon in urine but if present, may show an oval calcified egg with a lateral or terminal spine
Cytology images
Positive stains
- Schistosoma mansoni and Schistosoma japonium egg shells: acid fast (Am J Trop Med Hyg 1954;3:1066)
Negative stains
- Schistosoma haematobium egg shells: acid fast
Molecular / cytogenetics description
- Molecular testing of schistosome eggs in Africa showed hybrids of Schistosoma haematobium and livestock schistosoma species, S. mattheei and S. bovis (Emerg Infect Dis 2019;25:1245)
- Common chromosomal aberrations in schistosomiasis associated bladder cancer (Carcinogenesis 2000;21:1721)
- Loss: 8p, 18q, 17p, 5q, 9p, 10q, 11q, 18p, 11p, 9q, 20p, 6q (in descending order)
- Gain: 17q, 5p, 7q, 7p, 1q (in descending order)
- Most common genetic alterations in schistosomiasis associated bladder cancer (Nat Clin Pract Urol 2005;2:502)
- Low grade urothelial carcinoma: chromosome 9 loss of heterozygosity, FGFR3 activating mutation
- Dysplasia and carcinoma in situ: TP53 mutations, chromosome 9 loss of heterozygosity
- Loss of heterozygosity in schistosomiasis associated bladder cancer versus non schistosomiasis associated bladder cancer (J Natl Cancer Inst 1995;87:1383)
- 9p loss of heterozygosity (twofold higher in schistosomiasis associated bladder cancer)
- 9q loss of heterozygosity (threefold lower in schistosomiasis associated bladder cancer)
- Genes involved in schistosomiasis associated bladder cancer (Clin Microbiol Rev 1999;12:97)
- Mutation of FGFR3 (> 30%, more frequent in low grade papillary tumors)
- Activation of HRAS (7 - 17%, more frequent in low grade papillary tumors)
- Homozygous deletions of p16INK4A (more common in high grade Ta tumors) (Am J Pathol 1999;155:105)
- Inactivation of tumor suppressor genes TP53 and RB (more common in carcinoma in situ and high grade invasive tumors)
- Overexpression of ERBB2 in advanced urothelial carcinoma
- BCL2 expression in later stages of squamous cell carcinoma
Sample pathology report
- Urinary bladder, dome, biopsy:
- Urothelial mucosa with ulcerations, chronic granulomatous inflammation with eosinophils and calcified parasitic eggs, consistent with schistosomiasis related cystitis (see comment)
- Comment: The urothelial mucosa shows urothelial mucosa with granulation tissue and mixed inflammatory infiltrate composed predominantly of lymphocytes, neutrophils and eosinophils. There are many calcified oval parasitic eggs measuring approximately 120 microns with a sharp terminal spine. These changes of cystitis are consistent with Schistosoma haematobium infection. A small fragment of the muscularis propria is also present in the biopsy specimen.
Differential diagnosis
- Bladder with cystitis with calcifications:
- Calcified materials are mostly irregular and no prominent spines (Res Microbiol 2019;170:80)
- Urine crystals:
- Crystals are polarizable (Res Microbiol 2019;170:80)
Additional references
Board review style question #1
Board review style answer #1
Board review style question #2
Which of the following parasitic eggs contains a terminal spine?
- Schistosoma haematobium
- Schistosoma japonicum
- Schistosoma mansoni
- Schistosoma mekongi
Board review style answer #2