Table of Contents
Definition / general | Terminology | Sites | Etiology | Clinical features | Laboratory | Case reports | Clinical images | Gross description | Gross images | Microscopic (histologic) description | Microscopic (histologic) images | Differential diagnosis | Additional referencesCite this page: Rishi A, Cornish TC. Crohn's disease. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/anuscrohns.html. Accessed April 2nd, 2025.
Definition / general
- Anal canal involvement in 25 - 45% of Crohn's patients with small bowel involvement; up to 75% with colonic involvement
Terminology
- Also called granulomatous colitis but this is less specific
Sites
- Anal, anorectal and perianal skin
Etiology
- Etiology of chronic inflammatory bowel disease is unknown - may involve combination of genetic and inflammatory risk factors
- Genetic factors suggested by 10 - 15x increased risk in those with affected first degree relatives, 42 - 58% concordance rate in monozygotic twins
- Environmental factors such as smoking, certain food antigens, NSAID use and infectious agents may be important
- Perianal fistulas may develop from deep fissures or anal gland abscesses
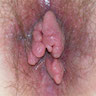
Clinical features
- Symptomatic perianal disease may precede GI symptoms in 5 - 20% of patients (Dis Colon Rectum 1996;39:136, Aust N Z J Surg 1996;66:5, Dis Colon Rectum 1995;38:121)
- The presence of recurrent isolated anal fissures, fistulas or perianal abscesses should raise the suspicion for evolving Crohn's disease; internal fistulas are virtually pathognomic
- Major complications include abscesses, fistulas, anal tags and fissures, which can present as anal pain, purulent discharge, fresh bleeding per rectum or anal incontinence (Am Fam Physician 2010;82:419)
- Disease location and age < 40 years are most common factors associated with perianal complications (Inflamm Bowel Dis 2002;8:244)
- Malignancy (anal canal adenocarcinoma) may be seen in longstanding perianal Crohn's disease (Intern Med 2013;52:445)
- Perianal fistulizing disease is associated with genetic susceptibility involving chromosome 5 with candidate interleukin genes IL3, IL4, IL5, I-13, CSF2 (World J Gastroenterol 2011;17:1939)
Laboratory
- Serum pANCA may be increased in patients with left sided disease with an ulcerative colitis-like clinical phenotype and histological features
Case reports
- 28 year old woman with painful perianal lesions (Am Fam Physician 2010;82:419)
- 50 year old woman with late perianal mucinous adenocarcinoma after Crohn's disease proctectomy (World J Surg Oncol 2005;3:42)
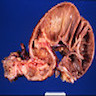
Gross description
- Varies based on location of fistula and associated healing process
- May have firm and fibrotic perirectal areas with adherent perianal skin showing external communication of fistula
- May present as perirectal mass if there has been significant healing
- Some grossing points:
- Recommended to take gross photographs of specimen when fresh
- Communication of fistula is best demonstrated by inserting a blunt metallic probe from the mucosal aspect of unfixed resection specimen - the key is finding the opening of either the sinus or fistula tract at the mucosal aspect
- Formalin fixation of these specimens is best accomplished by opening the luminal aspect of colon in a longitudinal direction and pinning the specimen flat
- This technique may be challenging for large resection specimens with long lengths of colon
- Adhesions or fistulae to other visceral organs or parts of the bowel may also be present, distorting the specimen and making orientation difficult
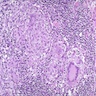
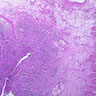
Microscopic (histologic) description
- Features of acute colitis: cryptitis (neutrophils in crypt epithelium), crypst abscesses (neutrophils within crypt lumens), erosions, ulcers
- Features of chronic colitis: crypt distortion, loss of goblet cells, basal plasmacytosis, crypt shortfall (base of crypts not touching the muscularis mucosae), Paneth cell metaplasia in left colon
- Nonnecrotizing granulomatous inflammation with variable giant cells in mucosa or fibroconnective tissue of fistula tract (may resemble foreign body type granulomas)
- Transmural chronic inflammation (best visualized on resection specimens)
- Patchy mucosal involvement with skip lesions which looks near normal on histology or may have mild reactive epithelial changes
- Acute and chronic inflammatory granulation tissue secondary to ulceration and fistula formation
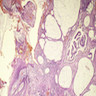
Microscopic (histologic) images
Differential diagnosis
- Perianal tuberculosis and fungal infections
- Rare ulcerative colitis induced perirectal fistulas: internal fistulas are rare
Additional references