Table of Contents
Definition / general | Essential features | Terminology | Epidemiology | Pathophysiology | Diagrams / tables | Clinical features | Symptoms | Screening | Donor deferral | Prevention | Laboratory | Radiology description | Radiology images | Case reports | Treatment | Microscopic (histologic) description | Sample assessment & plan | Differential diagnosis | Additional references | Board review style question #1 | Board review style answer #1 | Board review style question #2 | Board review style answer #2Cite this page: George MR. Transfusion related acute lung injury. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/transfusionmedtrali.html. Accessed April 3rd, 2025.
Definition / general
- Transfusion related acute lung injury (TRALI) is an adverse outcome of transfusion in which acute respiratory distress occurs within 6 hours of a transfusion
- Antibody mediated process in which antibodies in the transfused product or less commonly in the recipient attract neutrophils to the pulmonary vasculature
- TRALI features noncardiogenic, protein rich edema, while transfusion associated circulatory overload (TACO) features cardiogenic, protein poor edema
Essential features
- Respiratory distress / acute lung injury developing within 6 hours of cessation of transfusion
- Radiographic evidence of new bilateral infiltrates
- Hypoxemia
- PaO2/FiO2 ≤ 300 mmHg
- Oxygen saturation < 90% on room air
- No previous evidence of acute lung injury (ALI), such as circulatory overload or acute respiratory distress syndrome (ARDS)
- No evidence of left atrial hypertension (i.e., circulatory overload)
Terminology
- Transfusion related acute lung injury (TRALI)
- Acronym TRALI was coined in 1985 by Popovsky and Moore (Transfusion 1985;25:573)
Epidemiology
- Difficult to pinpoint the exact incidence due to underreporting, lack of standardization of criteria and differences in study population, thus complicating meta analysis (Transfusion 2023;63:104)
- Incidence is likely decreasing with increased use of leukoreduced products, leading to decreased alloimmunization and also reverse TRALI
- TRALI has been reported following transfusion of all blood products
- Most common with plasma rich blood products (> 60 mL of plasma)
- Plasma from female donors increases risk (see Prevention)
- Directed blood donation from mother to child increases risk
Pathophysiology
- A 2 hit hypothesis has been proposed
- Hit 1: patient's underlying condition
- Proinflammatory conditions prime neutrophils, endothelial cells and effector cells
- High interleukin (IL) 8 in recipient's plasma pretransfusion is an independent risk factor
- Hit 2: transfused blood component activates the neutrophils within the pulmonary vasculature, which in turn causes plugging and endothelial damage
(Transfusion 2019;59:2465, Ann Am Thorac Soc 2022;19:705)
- Cognate human leukocyte antigen (HLA) class I or II or human neutrophil antigen (HNA) antibody
- Granulocyte antibody positive by granulocyte immunofluorescence test (GIFT)
- Higher volume of female plasma
- Hit 1: patient's underlying condition
- Antibody mediated
- Passive transfer of HLA class I or class II or HNA antibodies from donor blood to a transfusion recipient (Blood 2019;133:1840)
- HLA class II antibodies are more frequent than class I in TRALI (Vox Sang 2008;95:313)
- Exposure to foreign HLA or HNA molecules through transfusion, transplantation or pregnancy can cause alloimmunization against foreign antigens
- Antibodies can cause immediate destruction of cells bearing cognate antigens → cascade of inflammatory events leading to TRALI (Vox Sang 2008;94:324)
- Antibodies are not always found in suspected TRALI cases (JAMA 2002;287:1968, Vox Sang 2007;93:70, Blood Transfus 2022;20:454)
- Mechanism of action of lung damage (Blood 2019;133:1840)
- Neutrophils normally tether to endothelium under shear stress
- Neutrophils are normally spherical with a diameter of 6 - 8 μm
- Pulmonary capillaries, which range in diameter from 2 to 15 μm, force neutrophils to flatten out to pass through and make them unable to roll (J Appl Physiol 1995;79:493)
- Priming of neutrophils (caused by HLA and HNA antibodies) disrupts neutrophil shape change and leads to mechanical plugging of pulmonary vessels
- Pulmonary inflammation → emigration of neutrophils from capillary beds into the alveolar spaces (J Appl Physiol 1995;79:493)
- Primed neutrophils release cytokines → damage endothelium → protein rich fluid leaks through endothelial gaps → exudate into alveolar spaces → respiratory distress = TRALI (N Engl J Med 2005;353:2788)
- Inverse TRALI (induced by transfusion of neutrophils to a patient with preformed antibodies against HLA / HNA)
- HLA or HNA alloimmunized patients receiving blood components that contain neutrophils, e.g., granulocytes
Diagrams / tables
Clinical features
- 2019 consensus TRALI definition (Transfusion 2019;59:2465, Ann Am Thorac Soc 2022;19:705)
- TRALI type I: patients with no risk factors for acute respiratory distress syndrome (ARDS) meeting the following criteria
- Acute onset
- Hypoxemia (PaO2/FiO2 ≤ 300 mmHg* or SpO2 < 90% on room air)
- *Correction factor needed for high altitude geographies
- Bilateral pulmonary edema on imaging
- No evidence of left atrial hypertension (LAH) or LAH not thought to be a major contributor
- Onset within 6 hours of transfusion
- No temporal relationship to alternative risk factor for ARDS
- TRALI type II: patients with risk factors for ARDS or that have existing mild ARDS but suffer further respiratory deterioration
- Findings as above with the exception of no temporal relationship to ARDS
- Stable respiratory status in 12 hours before transfusion
- TRALI type I: patients with no risk factors for acute respiratory distress syndrome (ARDS) meeting the following criteria
- Clarification of non-TRALI lung injury / pulmonary edema
- Acute respiratory distress syndrome (ARDS): patients with risk factors for ARDS who worsen not due to transfusion but rather underlying factors
- Onset of ARDS within 6 hours of transfusion, unstable / worsening respiratory status in the 12 hours prior to transfusion
- Existing ARDS that worsens after transfusion but was already worsening in the 12 hours prior to transfusion
- TRALI / TACO cannot be distinguished; risk factors for both, possibly both conditions occurring simultaneously
- Acute respiratory distress syndrome (ARDS): patients with risk factors for ARDS who worsen not due to transfusion but rather underlying factors
- Findings that may be helpful but are not required for diagnosis include
- Frothy pink secretions in ventilator tubing
- No response to diuretics, as opposed to transfusion associated circulatory overload, which does respond
- Short lived, sudden drop in white blood cell count, particularly with neutropenia, resulting from neutrophil sequestration in small alveolar blood vessels
- While the presence of antibodies against HLA or HNA is helpful for diagnosis, they are not absolutely required
- References: CDC: National Healthcare Safety Network Biovigilance Component Hemovigilance Module Surveillance Protocol [Accessed 4 November 2024], Blood 2019;133:1840
Symptoms
- Sudden onset of respiratory distress within 6 hours of transfusion
- Fever, hypotension, tachycardia
- Physical exam should not show any sign of fluid overload
- Varies from mild to life threatening
Screening
- Women who have been pregnant have a higher likelihood of developing HLA and HNA antibodies due to alloimmunization from the fetus
- Most significant in plasma rich products such as fresh frozen plasma and apheresis platelets
- Initial efforts to limit products from female donors → use of male only plasma in United Kingdom and United States → dramatically reduced rate of TRALI
- Screening donors for anti-HLA
- References: Hematology Am Soc Hematol Educ Program 2018;2018:585, Blood 2019;133:1840
Donor deferral
- Donor lookback and deferral is critical to protect future patients
- Very important to identify cocomponents
- Hospital should notify blood center following a potential case of TRALI
- Investigate pregnancy, transfusion or transplantation history of the donor
- Determine if the donor has anti-HLA or HNA antibodies; if yes, then the patient is also tested to see whether an antigen - antibody interaction could be implicated
- Donors with anti-HLA or HNA antibodies matched to recipient antigens in a possible case of TRALI are deferred indefinitely (AABB: TRALI Risk Mitigation for Plasma and Whole Blood for Allogeneic Transfusion [Accessed 4 November 2024])
Prevention
- Defer donors confirmed to be implicated in TRALI
- Use only male plasma to avoid the risk of anti-HLA antibodies formed in females during pregnancy
- Screen female donors of apheresis platelets for HLA antibodies, indefinitely defer those with antibodies
- Use of solvent detergent treated plasma to dilute possible antibodies (large pools of donors), mainly in European countries
- References: Hematology Am Soc Hematol Educ Program 2018;2018:585, Vox Sang 2017;112:694, AABB: TRALI Risk Mitigation for Plasma and Whole Blood for Allogeneic Transfusion [Accessed 4 November 2024]
Laboratory
- Short lived, sudden drop in white blood cell count, particularly with neutropenia, resulting from neutrophil sequestration in small alveolar blood vessels
- No elevation in brain natriuretic peptide (BNP) as in TACO
- Pleural fluid is exudate rather than transudate (as in TACO) with a protein content of > 2.9 g/dL, fluid protein to serum protein ratio of > 0.5 and cholesterol content of > 45 mg/dL
- References: Hematology Am Soc Hematol Educ Program 2018;2018:585, Cohn: Technical Manual, 21st Edition, 2023, Blood 2019;133:1840
Radiology description
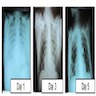
- Bilateral patchy infiltrates indicative of pulmonary edema
- Chest Xrays show initial TRALI reaction showing severe pulmonary edema on day 1 with significant resolution through days 3 and 5
Case reports
- 7 year old girl and 54 and 56 year old men with hematological malignancies and suspected TRALI following transfusions of buffy coat derived granulocytes and peripheral blood stem cells (Transfus Apher Sci 2022;61:103466)
- 19 year old man with TRALI caused by HLA-II antibodies (Lab Med 2023;54:e117)
- 28 year old woman treated with convalescent plasma for COVID-19 complicated by ARDS due to TRALI (BMJ Case Rep 2021;14:e239762)
- 48 year old Caucasian man with a history of chronic alcohol abuse, current smoking, community acquired pneumonia and suspected TRALI type II (Pulmonology 2024;30:495)
- 69 year old man without ARDS risk factors developed TRALI caused by a unit of solvent detergent treated plasma (Transfusion 2022;62:594)
- 17 cases of TRALI after intravenous immunoglobulin (IVIG) (Clin Rheumatol 2020;39:541)
Treatment
- Stop the transfusion
- Report the transfusion to the transfusion medicine service to start the investigation
- Supportive management only
- Mechanical ventilation may be needed in severe cases
- Most patients improve within 48 - 96 hours
- Mortality is 5 - 10%
- Indefinite deferral of blood donor to prevent future cases
- Future directions may include interleukin 10 (IL10) therapy, downregulation of C reactive protein (CRP) levels, targeting reactive oxygen species (ROS) or blocking interleukin 8 (IL8) receptors
- Reference: Blood 2019;133:1840
Microscopic (histologic) description
- Acute respiratory distress syndrome with extensive intra-alveolar edema and presence of neutrophils
- Hyaline membranes and distortion of pulmonary architecture
- Capillary leukostasis
- Electron microscopy shows degranulation of neutrophils in contact with injured endothelium (Transfusion 1986;26:278, Chest 2001;119:219)
Sample assessment & plan
- Assessment:
- Patient is a 75 year old man who developed respiratory distress 2 hours after a packed red blood cell (pRBC) transfusion. He had normal ejection fraction, no elevation in brain natriuretic peptide (BNP) and treatment with diuretics did not resolve his respiratory distress. The blood supplier was notified and performed testing of the donor sample. Testing of the donor sample identified anti-HLA DR11, DR13 and DR52. Patient had matching cognate antigens - HLA type DR11, DR13 and DR52.
- Plan:
- The patient presentation and laboratory workup are consistent with a diagnosis of transfusion related acute lung injury (TRALI).
Differential diagnosis
- Transfusion associated circulatory overload:
- Fluid overload → increased pulmonary capillary pressure → cardiogenic edema = congestive heart failure
- Patient often has a predisposition to congestive heart failure
- Hypertension rather than the hypotension typically seen in TRALI
- Elevated BNP, e.g., post to pretransfusion ratio of BNP ≥ 1.5 (indicates stretched ventricular muscle due to volume overload)
- Transudative rather than exudative alveolar edema
- All blood components have been implicated, volume issue, no particular product is more commonly associated
- See Diagrams / tables
- Transfusion associated dyspnea:
- Diagnosis of exclusion that does not meet criteria for TRALI or TACO
- No specific underlying pathophysiology has been identified
Additional references
Board review style question #1
What is a key feature seen in transfusion related acute lung injury (TRALI) but not in transfusion associated circulatory overload (TACO)?
- Decreased oxygen saturation
- Hypotension
- New pulmonary infiltrates
- Pre-existing, underlying cardiac dysfunction
- Response to diuretics
Board review style answer #1
B. Hypotension is often seen in TRALI, as opposed to hypertension seen in TACO, as a result of expansion of intravascular fluid volume. Answers A and C are incorrect because new pulmonary infiltrates and decreased oxygen saturation are seen in both. Answers D and E are incorrect because response to diuretics and pre-existing, underlying cardiac dysfunction are more commonly seen in TACO than TRALI.
Comment Here
Reference: Transfusion related acute lung injury
Comment Here
Reference: Transfusion related acute lung injury
Board review style question #2
A 55 year old woman with acute myeloid leukemia, status postallogeneic bone marrow transplant with severe neutropenia and unresponsive fungal infection is receiving granulocytes. She develops severe respiratory distress shortly after the transfusion is completed, necessitating mechanical ventilation. Her fluid balance is neutral and she has no pre-existing cardiac dysfunction. What laboratory testing would help confirm a diagnosis of inverse transfusion related acute lung injury (TRALI)?
- Anti-HLA / HNA antibodies in the donor that match antigens in the recipient
- Anti-HLA / HNA antibodies in the recipient that match antigens in the donor
- Elevated brain natriuretic peptide (BNP)
- Pleural fluid with protein content < 2.5 g/dL and fluid protein to serum protein ratio of < 0.5 and cholesterol content of < 45 mg/dL
- Short lived, sudden increase in neutrophils in complete blood count
Board review style answer #2
B. Anti-HLA / HNA antibodies in the recipient that match antigens in the donor. Inverse transfusion related acute lung injury refers to the recipient having antibodies against antigens in the donor. Answers C and D are incorrect because elevated BNP and transudative pulmonary fluid are seen in transfusion associated circulatory overload (TACO). Answer A is incorrect because it describes traditional TRALI occurring when antibodies in the donor match cognate antigens in the recipient. Answer E is incorrect because TRALI may feature a sudden, short lived decrease rather than an increase in neutrophils in a complete blood count.
Comment Here
Reference: Transfusion related acute lung injury
Comment Here
Reference: Transfusion related acute lung injury