Table of Contents
Definition / general | Essential features | Clinical features | Diagnosis | Radiology description | Case reports | Gross description | Microscopic (histologic) description | Microscopic (histologic) images | Positive stains | Board review style question #1 | Board review style answer #1 | Board review style question #2 | Board review style answer #2Cite this page: Garg S. Metastases. PathologyOutlines.com website. https://www.pathologyoutlines.com/topic/placentamets.html. Accessed April 23rd, 2024.
Definition / general
- Metastatic involvement of placenta by maternal or fetal tumors
- Placental metastases during pregnancy affect about 0.1% of pregnant women and most of them are of maternal origin, rarely of fetal origin (Cancer 1970;25:380)
- Infrequent occurrence of this condition suggests that biological protective mechanisms may exist for the placento - fetal unit disrupted only by malignancies with particular invasive properties like melanoma (Singapore Med J 2008;49:e71)
- Women presenting with maternal neoplasms metastatic to the placenta usually have widespread disease and poor prognosis (Fetal Pediatr Pathol 2017;36:465)
Essential features
- Most common metastatic maternal tumors are melanoma (30%) (J Clin Oncol 2003;21:2179), breast carcinoma (14%), leukemia and lymphoma (15%), small cell carcinoma of lung (N Engl J Med 2002;346:1501) and gastric carcinoma (Oncol Lett 2014;8:2509)
- Metastatic fetal tumors are very rare and include neuroblastoma (Int J Clin Exp Pathol 2014;7:8198), adenoid cystic carcinoma of trachea (Hum Pathol 1989;20:193), hepatoblastoma, melanoma and rhabdoid tumor
- Fetal and maternal circulation is separated by trophoblast, connective tissue of the villus and the capillary wall (which prevents tumor spread from the placenta to the fetus in most cases); only when the tumor cells from the intervillous space invade into the villous capillaries can the metastases to fetus occur (Cancer 1970;25:380); spread to fetus more likely occurs in metastases with villous invasion and is rare in metastases confined to the intervillous space
Clinical features
- Placental abruption with disseminated intravascular coagulation and fetal death can occur due to placental metastases in the intervillous space
- Rarely, the mother may suffer from antepartum effects, such as sweating, flushing, palpitations and hypertension due to production of catecholamine by fetal neuroblastoma
Diagnosis
- Meticulous histologic examination of the placenta is necessary in patients with previous diagnosis of malignancy and in those with fetal neoplasia detected antenatally
Radiology description
- Nonspecific increased placental thickness
Case reports
- 29 year old gravida 4, para 3 woman with cervical squamous cell carcinoma metastatic to placenta (Int J Gynecol Pathol 2013;32:516)
- 35 year old gravida 2, para 0 woman with gastric carcinoma metastatic to placenta (Oncol Lett 2014;8:2509)
- Two patients with gastric carcinoma metastatic to placenta (Fetal Pediatr Pathol 2017;36:465)
Gross description
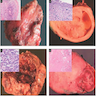
- Placenta may appear bulky, pale and heavy
- Tumor deposits are usually not macroscopically detectable (being identified mostly on histologic examination)
Microscopic (histologic) description
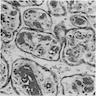
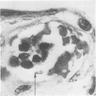
- Multifocal clusters of malignant cells adjacent to intact villi
- Metastases from maternal melanoma may show infiltration of villous stroma by malignant cells with Hofbauer cells containing melanin, even in the absence of villous invasion
- Most cases of placental involvement are associated with minimal fetal complications but massive placental infiltration by maternal metastasis can lead to intrauterine fetal death (IUFD)
- Presence of malignant cells in the intervillous space has been classified as placental metastasis although in reality the tumor cells remain within the maternal vascular space and in most cases do not truly invade placental tissue
- Maternal leukemia with circulating malignant hematopoietic cells is associated with similar cells admixed within the intervillous space without true invasion (Ultrasound Obstet Gynecol 2009;33:235)
Positive stains
- Stains specific for the primary maternal or fetal malignancy
Board review style question #1
When is the risk of fetal metastasis by a maternal malignant tumor highest during pregnancy?
- When the placenta is normal microscopically
- When the tumor cells are present in the chorionic membranes
- When the tumor cells are seen in the intervillous space
- When the tumor cells invade into the chorionic villi
Board review style answer #1
Board review style question #2
Which maternal and fetal tumors, respectively, have been shown to have the highest proportion of placental metastases?
- Breast carcinoma and adenoid cystic carcinoma
- Gastric carcinoma and hepatoblastoma
- Leukemia and rhabdoid tumor
- Melanoma and neuroblastoma
Board review style answer #2